IBD Literature Report
Coverage: May 24, 2026 - May 31, 2026
157
Papers This Week
18
Categories
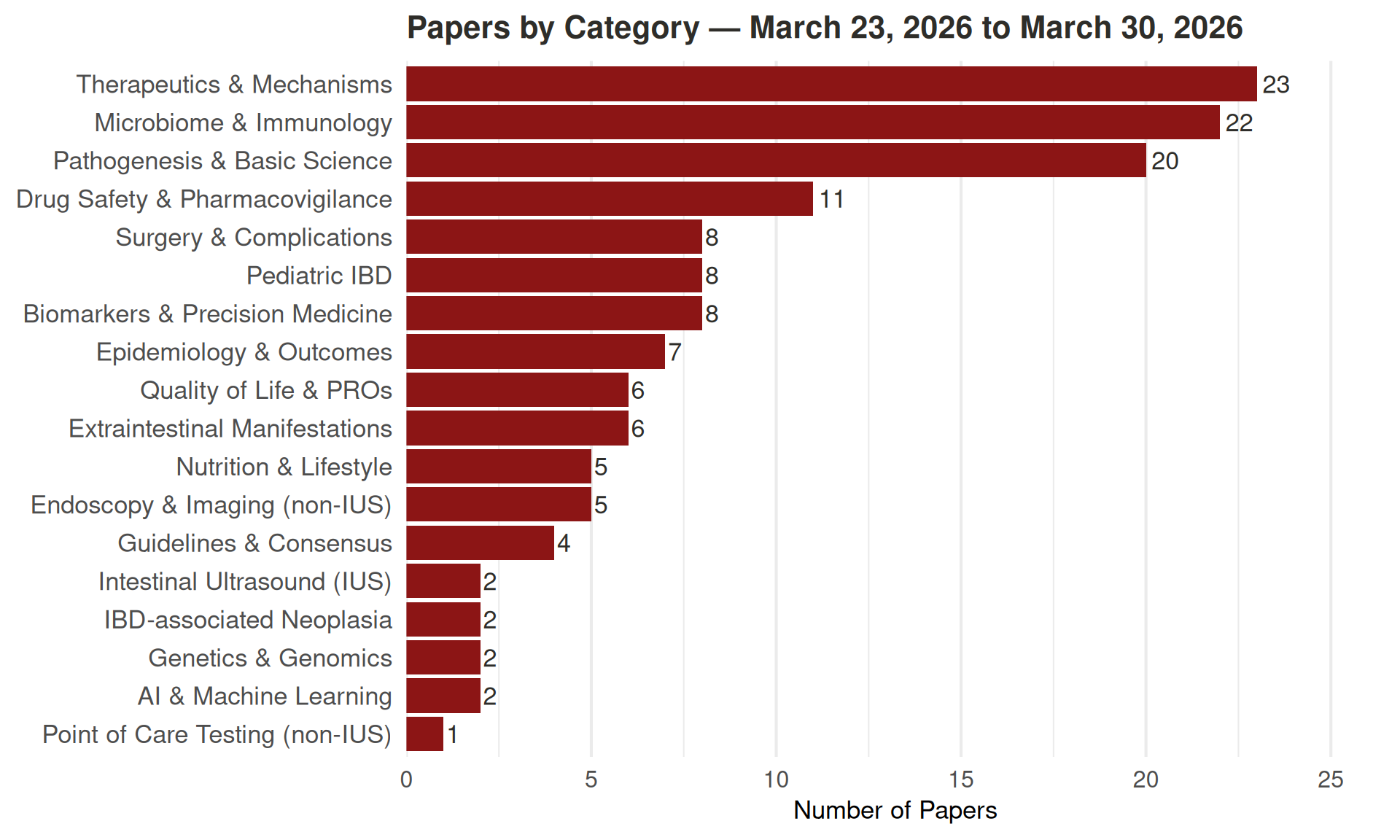
Papers by Category
Click a category to expand. Click a paper title to read its abstract.
Microbiome & Immunology (19 papers)
ABCG2 Upregulation Involving AKT/NF-κB Signaling Contributes to Intestinal Barrier Dysfunction in Inflammatory Bowel Disease. Digestive diseases and sciences | 2026-05-29
Previous investigations demonstrated significant upregulation of ATP-binding cassette subfamily G member 2 (ABCG2) in renal, hepatic, colonic, and intestinal tissues within a 2,4,6-trinitrobenzenesulfonic acid (TNBS)-induced murine model of Crohn’s disease (CD). Nevertheless, the regulatory mechanisms governing ABCG2 expression within inflammatory microenvironments and its consequent impact on intestinal barrier integrity remain incompletely elucidated. This study aimed to elucidate the signaling pathway responsible for ABCG2 upregulation under inflammatory conditions and to investigate the functional role of ABCG2 in intestinal barrier integrity both in vitro and in vivo. Intestinal epithelial barrier integrity was evaluated by measuring transepithelial electrical resistance (TEER), paracellular permeability to fluorescein isothiocyanate (FITC)-dextran, and immunofluorescence/immunoblot analysis of tight junction proteins. Abcg2-/- mice were utilized to evaluate the contribution of ABCG2 to intestinal barrier homeostasis. ABCG2 expression was observed to be significantly elevated in lipopolysaccharide (LPS)-stimulated intestinal epithelial cells. This induction coincided with enhanced phosphorylation of AKT and P65. Pharmacological inhibition of AKT (LY294002) or NF-κB (BAY117082) attenuated the LPS-mediated upregulation of ABCG2. Functional assessments revealed that pharmacological inhibition of ABCG2 (using Ko143) or its genetic ablation enhanced intestinal barrier integrity. This was evidenced by increased TEER, reduced permeability to FITC-dextran, and restored expression of key tight junction proteins (ZO-1, occludin, and claudin-1) following LPS challenge. Specifically, Abcg2 knockout improved colon length, preserved mucosal architectural integrity, and diminished inflammatory cell infiltration in both dextran sulfate sodium (DSS)-UC and TNBS-induced CD models. ABCG2 reprents a promising therapeutic target for inflammatory bowel disease (IBD), particularly in patient populations exhibiting dysregulated transporter activity or genetic variants influencing drug response.
Shi P, Deng J, Song X, Tang L, Guo H, Yin F
Polyclonal antibodies and probiotics improve immune dysfunction in a mouse model of inflammatory bowel disease. Scientific reports | 2026-05-28
Inflammatory bowel disease (IBD) is a chronic digestive disorder caused by the overactivity of the mucosal immune system in response to natural intestinal bacteria and environmental factors, affecting genetically susceptible individuals. This research investigates the preventive effect of probiotics (P), specifically Lactobacillus fermentum, Lactobacillus L. reuteri, and polyclonal antibodies (AB), on morphological changes and markers of intestinal inflammation in the IBD mice model. Our study spanned 54 days. For the first 21 days, we observed microbial populations and immunoglobulin levels. Then, we induced chronic inflammation over three 11-day cycles. In each cycle, subjects received 2% dextran sulfate sodium (DSS) for 4 days, followed by 7 days of normal water. 75 C57BL/6 mice have been used in 5 groups: DSS, control, DSS + P, DSS + AB, and a combined treatment group of antibodies and probiotics (DSS + ABP). Throughout the study period, clinical symptoms were monitored, and morphological changes and histological scores were assessed after the course. Levels of IBD biomarkers in serum such as nitrite, malondialdehyde enzyme (MDA), and myeloperoxidase enzyme (MPO), were measured along with alterations in cytokines Tumor Necrosis Factor-alpha (TNF-α), interleukin (IL)-4, IL-6, and IL-22, IgA and IgG in the blood serum. Results showed that All treatment groups, significantly reduced the Disease Activity Index (DAI), total histological score and oxidative stress markers MDA and MPO compared to the DSS group (p < 0.05). Additionally, the oral administration of polyclonal antibodies increased mucosal immunoglobulin levels, helping to prevent the rise in serum immunoglobulin levels and the associated increase in IL-4 (p < 0.05). Meanwhile, treatment with probiotics significantly (p < 0.05) reduced inflammation by modulating cytokine levels (TNF-α and IL-6). In conclusion, the co-administration of probiotics and polyclonal antibodies effectively mitigates IBD progression by synergistically improving histological parameters and regulating systemic immune responses, offering a more potent preventive strategy than individual treatments.
Ghaedi S, Harsij Z, Rizi MD, Rezaei M, Moein F, Mirasadi Z, Tanhaeivash N, Jamshidi N, Nasr-Esfahani MH, Hajian M
Beyond Suppression: The Plasticity, Dysfunction, and Therapeutic Reprogramming of Regulatory T Cells in Inflammatory Bowel Disease. Journal of leukocyte biology | 2026-05-28
Inflammatory bowel disease (IBD) is a chronic relapsing inflammatory disorder of the gut, whose pathogenesis is closely related to immune dysregulation. Regulatory T cells (Tregs), as a key cell population maintaining intestinal immune tolerance, exhibit not only reduced frequency but, more critically, profound functional deficiencies, including the generation of pro-inflammatory ex-Tregs, and loss of lineage stability in the inflamed gut microenvironment of IBD. This review systematically delineates the sophisticated biological characteristics of Tregs, with a particular focus on the epigenetic and metabolic checkpoints that govern their stability. We critically summarize the aberrant changes of Tregs in IBD, emphasizing mechanisms such as inflammatory cytokine-induced Treg plasticity (e.g., Th1-like or Th17-like conversion) and microbiota-metabolite axis-mediated functional modulation. Furthermore, we provide an in-depth analysis of emerging therapeutic strategies aimed at restoring Treg suppressive capacity, including selective cytokine therapy (e.g., low-dose/engineered IL-2), adoptive transfer of engineered antigen-specific Tregs (including CAR-Tregs), microbiome/dietary interventions, and pharmacological modulation of Treg differentiation. We also discuss the disrupted crosstalk between Tregs and other innate and adaptive immune cells within the IBD milieu. Finally, this review highlights how cutting-edge technologies like single-cell multi-omics and spatial transcriptomics are delineating the heterogeneous landscape and uncovering novel, disease-specific Treg subpopulations, thereby paving the way for precise Treg-targeting therapies. Unlike previous reviews that broadly catalog Treg abnormalities, this review offers a refined conceptual framework centered on the critical distinction between lineage-defective ex-Tregs and exhausted effector Tregs (eTregs), and integrates recent multi-omics insights to redefine Treg functional failure in IBD.
Shao Y, Yu S, Zhang M, Huang Y, Dou Z, Tian B, Lu J
Cross-kingdom metabolic interactions govern Candida albicans overgrowth and colitis progression. Cell host & microbe | 2026-05-28
Inflammatory bowel disease is shaped by complex microbial communities, yet the contribution of fungal-bacterial interactions to disease progression remains poorly defined. Here, we identify Cladosporium tenuissimum (C. tenuissimum) as a gut fungus with potent colitis-alleviating activity. Mechanistically, C. tenuissimum restrains Candida albicans (C. albicans) overgrowth through nutrient competition, particularly via the utilization and subsequent limitation of the amino acid ornithine. C. albicans can evade this suppression and potentiate intestinal inflammation through nutrient escape by preferentially exploiting specific amino acids, such as threonine. We further reveal a bacterial-fungal metabolic axis in which threonine-producing Bacteroides fragilis facilitates C. albicans escape from gut microbiome-mediated fungal control, thereby exacerbating colitis. Notably, dietary threonine restriction markedly attenuates C. albicans-driven colitis in mice. Together, our findings uncover a cross-kingdom metabolic network that determines C. albicans homeostasis and, in turn, governs intestinal inflammatory outcomes, offering new conceptual and therapeutic avenues for IBD.
Zhou Y, Ding J, Ning L, Xu X, Dou L, Shen J, Xuan B, Wang Z, Jiang Y, Zhao Y
Milk extracellular vesicles attenuate pre-inflammatory bowel disease via Lctobacillus murinus-mediated TLR2 signaling modulation.★ Cell reports | 2026-05-28
Pre-inflammatory bowel disease (pre-IBD) represents a transitional state between irritable bowel syndrome and IBD, characterized by heightened susceptibility to mucosal inflammation driven by chronic high-fat diet intake and antibiotic exposure. However, effective intervention strategies remain poorly defined. Here, we identify milk-derived extracellular vesicles (mEVs) as a potent nanotherapeutic capable of attenuating pre-IBD pathology. Pre-IBD mice displayed marked gut microbiota dysbiosis and mucosal inflammation, both of which were substantially ameliorated by oral mEVs administration. Mechanistically, mEVs restored microbial homeostasis by enriching Lactobacillus murinus (L. murinus), which in turn reduced lysophosphatidylcholine (LPC) accumulation, two factors that exerted opposing and functionally instructive effects on intestinal inflammation. LPC activated the TLR2/MAPK axis to promote M1 polarization, whereas L. murinus engaged the TLR2/STAT3 pathway to drive M2 polarization. Collectively, these findings demonstrate that mEVs reprogram TLR2-dependent macrophage responses by modulating LPC and L. murinus, thereby mitigating mucosal inflammation and preventing the progression of pre-IBD.
Xu J, Wei G, Wang J, Wang H, He J, Xu J, Cao W, Wang J, Shen Q, Ai N
The endogenous peptide GPR15L shapes the intestinal microbiota to counteract colitis.★ Gut | 2026-05-28
The peptide GPR15L is produced by colonic epithelial cells and has been implicated in T cell recruitment to the large intestine. However, its role in chronic colitis has been unclear so far. To explore the role of GPR15L in the pathogenesis of experimental colitis and IBD. We studied how genetic deletion or overexpression of Gpr15l as well as rectal application of recombinant GPR15L alters the course of acute dextran sodium sulfate colitis and T cell transfer colitis. The impact of GPR15L on microbiota was explored with co-housing, littermate and faecal microbiota transfer studies, by 16S rRNA sequencing as well as anti-microbial assays and shotgun metagenomics. The expression of GPR15L was evaluated across three independent cohorts of patients with IBD and correlated to microbial diversity and flare-free survival. GPR15L clearly mitigated experimental colitis, but this was independent of T cell recruitment and GPR15. Instead, we observed that the effects of GPR15L were mediated by altered microbiomes in the large intestine and, consistently, showed that GPR15L acts as an antimicrobial peptide under anaerobic conditions and shapes microbial communities towards a homeostatic phenotype. Rectal supplementation of GPR15L counteracted experimental colitis. In patients with IBD, GPR15L expression was decreased in active inflammation, correlated with microbial diversity and was associated with flare-free survival. GPR15L is a host-defence peptide that plays a beneficial role in the pathogenesis of intestinal inflammation. It seems promising to further evaluate its potential as a future therapeutic approach in IBD.
Leggio M, Schramm S, Dietz L, Ocón B, Wirtz S, Puertolas Balint F, Yilmaz B, Petzold J, Liu LJ, Dedden M
Exopolysaccharides from Weissella confusa HYF86 with sugarcane juice as a substrate alleviate colitis in mice by regulating gut microbiota. Food & function | 2026-05-26
Ulcerative colitis is an inflammatory bowel disease with increasing global incidence, which urgently demands safe and sustainable intervention strategies. This work investigated the alleviative effects of exopolysaccharides from Weissella confusa HYF86 with sugarcane juice as a substrate (SEPS86) on DSS-induced acute colitis in mice. Here, in vivo fluorescence imaging revealed that SEPS86 was primarily retained in the gastrointestinal tract with strong fluorescence signals still detectable after 6 h of intervention. In addition, DSS treatment led to weight loss, elevated disease activity index and colon shortening in mice, whereas SEPS86 significantly alleviated colon shortening and showed a trend toward improving weight loss and disease activity index. In particular, SEPS86 upregulated the mRNA expression of claudin-1 by 2.82-fold compared with the DSS group. It is remarkable that SEPS86 significantly decreased the levels of IL-6 and IL-17, respectively. Gut microbiota analysis indicated that SEPS86 partially reversed the DSS-induced dysbiosis by enriching beneficial bacteria, including Dubosiella. In addition, SEPS86 significantly increased the level of butyric acid, which was 2.00-fold that of the DSS group. Overall, SEPS86 exhibited protective effects against colitis and gut microbiota regulation, which lays a foundation for developing functional foods for gut health.
Sun S, Wu J, Wen S, Huang H, Lin Y, Zhang W, Zhang Y, Wang X, Pan L
C5 inhibition restores B cell homeostasis and humoral immunity in CHAPLE disease patients. Journal of human immunity | 2026-05-26
CHAPLE disease is a monogenic disorder in which CD55 deficiency drives gastrointestinal pathology. How CD55 deficiency affects adaptive immunity is unknown. Herein, molecularly, we characterize eight patients with genetically novel CD55 deficiency. Clinically, all patients developed early-onset protein-losing enteropathy, frequently complicated by thrombotic events, inflammatory bowel disease-like lesions, and recurrent respiratory infections. Ex vivo, immunophenotyping revealed disruption of the B cell compartment, marked by depletion of transitional B cells, expansion of CD21lo B cells, and accumulation of class-switched memory B cells and plasmablasts, while T cell subsets were largely preserved. In vivo, eculizumab rapidly resolved intestinal pathology, normalized serum albumin and immunoglobulin levels, and re-established a normal B cell profile. Furthermore, C5 inhibition enabled effective humoral protection and optimal pneumococcal vaccine responses. Together, these findings establish complement inhibition as central to B cell homeostasis in CHAPLE disease.
Tahiat A, Belbouab R, Yagoubi A, Buta Panov S, Cuollo L, Djenouhat K, Bogunovic D
Natural antigen landscape shaping intestinal Treg cells: Self, diet, and microbiota.Review International reviews of immunology | 2026-05-25
The gut represents a melting pot of distinct classes of antigens derived from self antigens, dietary components, and the commensal microbiota. To maintain tolerance to innocuous antigens while preserving the capacity to respond to potentially harmful microorganisms, the immune system has evolved tightly regulated mechanisms centered on the generation of Foxp3+ regulatory T (Treg) cells at mucosal surfaces. Although early insights into intestinal Treg development were largely derived from studies using model dietary antigens or selected microbial species, a substantial gap remains in our understanding of the natural antigen landscape that elicits Treg responses in vivo. In this review, we discuss recent advances based on TCR classification approaches that define intestinal Treg T cell receptor (TCR) responses according to in vivo antigen reactivity, and we highlight key future directions for elucidating the functional roles of antigen-presenting cell subsets and their associated peptide landscapes in shaping intestinal Treg biology. The intestine is constantly exposed to many substances from food, gut bacteria, and the body’s own antigens. The immune system must tolerate harmless substances while still being able to respond to infections. Regulatory T cells are a special type of immune cell that help maintain this balance in the gut. In this review, we explain how regulatory T cells in the intestine respond differently depending on where antigens come from—whether they originate from the body itself, from food, or from gut microbes. Recent studies show that these cells recognize natural antigens in a highly specific way. We also describe how different types of antigen-presenting cells guide regulatory T cell development and how this process can fail during intestinal inflammation, such as in inflammatory bowel disease. Understanding how the immune system normally maintains tolerance to antigens derived from the body itself, food, and gut bacteria may help guide new strategies to treat intestinal inflammatory disorders.
Yi J
miR-9394b from Lactobacillus paracasei extracellular vesicles targets iNOS to reprogram host NO-ornithine metabolism and ameliorate DSS-induced murine colitis. NPJ biofilms and microbiomes | 2026-05-25
Ulcerative colitis (UC) is a growing global health burden, creating an urgent need for new therapies. While extracellular vesicles (EVs) from probiotic bacteria show therapeutic potential, their molecular mechanisms are largely unknown. This study reveals that Lactobacillus paracasei (LPC) and its EVs (LPC-EVs) alleviate Dextran Sulfate Sodium Salt (DSS)-induced colitis in mice through a multi-faceted mechanism involving partial reshaping of the gut microbiota, suppression of TLR4/NF-κB signaling, and reinforcement of tight junctions. We found that miR-9394b carried by LPC-EVs plays a central role in this effect. In MODE-K cells, miR-9394b directly targets iNOS, shifting arginine metabolism away from nitric oxide (NO) production toward ornithine-associated metabolism. The increased ornithine served as a downstream mediator linking epithelial metabolic remodeling to macrophage polarization. Collectively, these findings support a model in which bacterial EVs mediate the transfer of miR-9394b to coordinate a metabolic-immune response, highlighting a potential avenue for miRNA-guided intervention in experimental colitis.
Ding H, Zhang H, Li D, Hu Z, Xiang G, Nie Q, Liu Q, Liang Y, Wang S, Tao S
A Dual-Pathway Wnt-IL-13 Fusion Protein Enhances Human Intestinal Regeneration Through Tuft Cell Activation. The Journal of biological chemistry | 2026-05-23
Compromised intestinal regenerative responses drive severe inflammatory conditions, such as inflammatory bowel disease and graft-versus-host disease, affecting millions of people worldwide each year. Despite extensive research, effective therapies remain limited, and no curative treatments are currently available. We recently discovered that human intestinal tuft cells promote tissue repair following injury through Wnt and IL-4/IL-13 signaling pathways. Building on this discovery, here we report the engineering and functional validation of a synthetic Wnt-IL-13 fusion protein that simultaneously activates both the Wnt and IL-4/IL-13 signaling pathways to enhance human intestinal tuft cell activity. Employing human organoid technology, we demonstrate that this therapeutic approach promotes mucosal healing.
Yang L, Huang L, van Rijt FLH, Zhang B, Giladi A, Bernink JH, Clevers H, Janda CY
Personalized barrier recovery induced by Lactobacillus helveticus SBT2171 in an In Vitro model of ulcerative colitis-derived fecal supernatants. BMC complementary medicine and therapies | 2026-05-23
Disruption of the intestinal epithelial barrier is a hallmark of inflammatory bowel disease (IBD). Although probiotics and postbiotics are increasingly recognized as potential therapeutic approaches, treatment efficacy is often influenced by patient-specific variability. In this study, intestinal inflammation was modeled by exposing HT-29 cells to fecal supernatants (FS) derived from three patients with ulcerative colitis (UC). The expression of pro-inflammatory (IL-8) and barrier-associated (Claudin-1, MUC2) genes was assessed by real-time PCR. Subsequently, the restorative effects of different preparations of Lactobacillus helveticus SBT2171, including live bacteria, cell-free supernatant, and debris-containing supernatant, were evaluated at 24 and 48 h. FS exposure significantly upregulated IL-8 expression while downregulating Claudin-1 and MUC2, thereby recapitulating IBD-associated epithelial disruption. Treatment with L. helveticus preparations partially restored barrier-related gene expression in a patient- and treatment-dependent manner. Live bacteria induced transient or sustained Claudin-1 upregulation depending on the FS source, whereas the cell-free supernatant demonstrated broader and more durable restorative effects across distinct inflammatory contexts. In contrast, debris-containing preparations exerted limited or even suppressive effects, particularly on MUC2 expression. These findings demonstrate that the barrier-restorative effects of L. helveticus in vitro is not uniform but shaped by the unique inflammatory and microbial environment of each patient. Collectively, our results support the potential of postbiotic formulations as safer and effective modulators of epithelial barrier repair and underscore the need for personalized strategies in microbiota-based therapies for IBD.
Khademi M, Kazemifard N, Fathi M, Farmani M, Baradaran Ghavami S, Khanabadi B, Shahrokh S
Fucoidan Oligosaccharides from Kjellmaniella crassifolia Ameliorate Ulcerative Colitis by Regulating the TLR4 and NF-κB Signaling Pathway and Modulating Gut Microbiota. Marine drugs | 2026-05-21
Ulcerative colitis (UC) is a form of inflammatory bowel disease (IBD), which is marked by severe abdominal pain, weight loss, perianal bleeding, and diarrhea. This study successfully isolated and purified four low-molecular-weight fucoidan oligosaccharides through acid hydrolysis and Bio Gel P10 gel filtration. The molecular weights were 2.9 × 104-1.36 × 105 Da, 182-1012 Da, 161-939 Da and 161-939 Da, respectively. A mouse model of colitis was induced using Dextran Sulfate Sodium (DSS). The results indicated that fucoidan and fucoidan oligosaccharides could ameliorate murine ulcerative colitis, with the oligosaccharides (200 mg/kg/d) demonstrating superior therapeutic effects. This superiority was likely attributed to the lower molecular weight and higher content of total sugars and fucose. The primary mechanisms involved the modulation of gene and protein expression levels associated with the Toll-like receptor 4, Myeloid differentiation primary response 88, nuclear factor kappa-light-chain-enhancer of activated B cells, p65, and Inhibitor of kappa light polypeptide gene enhancer in B cells, alpha (TLR4, MYD88, NF-κB p65, and IκB-α) signaling pathways, which reduce the production of inflammatory cytokines such as tumor necrosis factor-alpha, Interleukin-1 beta and Interleukin-6 (TNF-α, IL-1β, and IL-6). Additionally, these oligosaccharides alleviated oxidative stress, enhanced the levels of intestinal barrier proteins (Claudin family member 4 and Zonula occludens protein 1), regulated the abundance and diversity of the gut microbiota, and increased the levels of short-chain fatty acids (SCFAs) in the intestine. It is worth emphasizing that this study can only demonstrate that fucoidan oligosaccharides have a mitigating effect on intestinal inflammation in mice. Further research is needed in the future to investigate the structure-activity relationship of fucoidan oligosaccharides and their impact on human intestinal microbiota, in order to further elucidate their anti-inflammatory mechanisms.
Xu Z, Jia Z, Li L, Zeng F, Sun J, Ma Y, Shi W, Liu S, He Y, Wang Q
Fecal Microbiota Transplantation from Toddler Donors Ameliorated DSS-Induced Colitis in Mice by Reshaping Gut Microbiota. Nutrients | 2026-05-19
Background/Objectives: Gut microbiota dysbiosis is a key driver of inflammatory bowel disease (IBD), and fecal microbiota transplantation (FMT) has emerged as a potential therapeutic strategy. In this study, we investigated the protective effects of toddler-derived FMT against colitis and elucidated the underlying mechanisms. Methods: Firstly, fecal microbiota from healthy toddlers was transplanted into antibiotic-pretreated mice, establishing stable colonization between days 14 and 21 post-transplantation. Results: In a dextran sulfate sodium-induced colitis model, FMT significantly ameliorated colitis symptoms, including reduced disease activity index and restored colon length. Toddler-derived FMT improved the intestinal barrier by preserving goblet cell density and enhancing MUC2 expression. Meanwhile, colonic inflammation was alleviated by FMT, which suppressed pro-inflammatory cytokines, reduced CD4+ T cell counts, and associated with downregulation of JAK/STAT-related transcripts. 16S rRNA sequencing revealed that FMT remodeled the gut microbiota by enriching beneficial genera, including Bacteroides, Parabacteroides, Blautia, and Akkermansia, which correlated positively with colon length and negatively with inflammatory markers. Conclusions: These findings provided a theoretical foundation that toddler-derived microbiota represents a potential donor source for FMT in IBD.
Jing Y, Bai X, Ji Y, Zhai Z, Zhao Y, Hao Y
Gut Microbiota in Irritable Bowel Syndrome and Inflammatory Bowel Disease: Differences in Pathophysiology, Biomarkers, and Treatment Implications.Review Pharmaceuticals (Basel, Switzerland) | 2026-05-17
Alterations in the intestinal microbiota have been implicated in both irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD). However, their biological significance and therapeutic implications differ substantially between the two conditions. Although dysbiosis is a common feature, the mechanisms by which alterations in the microbiota contribute to disease pathophysiology and clinical expression are distinct. Some pathways are more prominent in IBS (e.g., the gut-brain axis), whereas others are more prominent in IBD (e.g., reduced microbial diversity). Equally important are pathways that appear to play a role exclusively in IBD [e.g., Adherent-invasive Escherichia coli (AIEC) and Paneth cells], as well as others that seem to be specific to IBS (e.g., mast cell activation). In IBD, microbiota changes are primarily linked to immune dysregulation, mucosal barrier impairment, and inflammation-driven pathways, whereas in IBS, they are mainly associated with functional disturbances mediated by neuroimmune signaling and microbial metabolites. Furthermore, several microbiome-associated biomarkers differ between these two diseases, and some are already assessed by international guidelines. Although the microbiota plays a key role in IBS and IBD pathophysiology, microbiome-based treatments remain limited, especially in IBD. There are clinically available treatments in IBS (e.g., rifaximin, low-FODMAP diet), but in IBD, only the probiotic VSL#3 is guideline-approved in ulcerative colitis pouchitis prophylaxis. Nevertheless, the dynamic nature of the microbiota continues to support the investigation of already studied (e.g., probiotics, fecal microbiota transplantation) and potential novel therapeutic approaches at the research level. The aim of this review is to compare the gut-microbiota-related pathophysiological pathways and biomarkers between IBS and IBD, to summarize the microbiome-related medications that have already been studied in both diseases, and to suggest new potential therapeutic options based on the gut microbiota.
Pastras P, Aggeletopoulou I, Psalti V, Triantos C
Integrative host transcriptomic and mucosal microbiome profiling reveals region-specific host-microbiome associations across the human intestine. bioRxiv : the preprint server for biology | 2026-05-14
Host genetics shapes gut microbiome composition, yet the physiological mechanisms underlying this relationship remain poorly understood. Characterizing associations between host gene expression and the mucosal microbiome offers a promising route to identifying the host pathways and microbial taxa most likely to interact physiologically. However, existing investigations have been conducted primarily in acute disease contexts and within the colon, leaving host-microbiome associations outside of acute inflammatory contexts and those in undersampled regions such as the terminal ileum poorly characterized. To address these gaps, we profiled paired host gene expression from full-thickness resections and mucosal microbiome data, both from macroscopically non-inflamed tissue from Crohn’s disease patients undergoing surgery across three intestinal sites: terminal ileum (n = 32), cecum (n = 35), and right colon (n = 30). Using a multi-level analytical framework including Procrustes analysis, sparse canonical correlation analysis, and elastic net regression, we identified significant associations between the mucosal transcriptome and microbiome. Intestine-wide, genes enriched in immune and intestinal barrier integrity pathways were associated with heritable taxa including Fusicatenibacter , consistent with patterns observed in microbiome genome-wide association studies. Region-specific analysis identified the terminal ileum as a distinct site of host-microbiome interaction, with associations involving metabolic and barrier-related pathways not observed in the large intestine. Notable terminal ileum-specific associations included PCDH20 with Faecalitalea and ACAT1 with Lactococcus , implicating epithelial barrier maintenance and host-microbiome metabolic interactions, respectively. These findings advance our understanding of the physiological basis of host-microbiome interactions across the intestine. The human gut is home to trillions of microorganisms that interact with the intestinal lining, yet we have a limited understanding of the specific biological processes involved in these interactions. Most studies characterizing the relationships between host gene expression and the gut microbiome have focused on the colon and on active disease contexts, leaving it unclear whether the associations observed reflect fundamental host-microbiome biology or disease-specific responses. By examining mucosal tissue, where host cells and microbes are in direct contact, across three sites in non-acutely inflamed tissue, we show that expression of immune defense and barrier maintenance genes is broadly associated with the microbiome across the intestine. We also identify distinct classes of associations in the terminal ileum, including host genes involved in metabolic processes. These findings provide a foundation for understanding how host biology and the gut microbiome are linked outside of acute disease.
Ryu EP, Keller CA, Nichols RG, Tran HN, Brocious PR, Harris LR, Koltun WA, Yochum GS, Davenport ER
The role of the complement system in gastrointestinal-related diseases.Review Frontiers in immunology | 2026-05-13
The complement system bridges innate and adaptive immunity, orchestrating immune surveillance and maintaining tissue homeostasis. This review summarizes the role of the complement system in gastrointestinal-related diseases, including its function in innate immunity, impact on adaptive immunity, and regulatory role under physiological and pathological conditions in the gut. The activation pathways, regulatory mechanisms, and interactions of the complement system with the gut microbiome are crucial for maintaining intestinal homeostasis. Genetic deficiencies or excessive activation of the complement system are closely associated with the development of various intestinal diseases, including infections, inflammatory bowel disease (IBD), and tumors. This review also explores the role of the complement system in the tumor microenvironment (TME) of the gut and its potential as a therapeutic target. By deepening our understanding of the mechanisms by which the complement system operates in gastrointestinal diseases, we can provide a theoretical foundation for the development of novel treatment strategies.
Yong B, Luo Z, Luo B, Liu J, Zeng Z, Zheng X
Emerging Role of Gut Microbiota in Modulating Response to Therapies in IBD.Review Microorganisms | 2026-05-11
The gut microbiota is increasingly recognized as a key contributor in the pathogenesis and progression of inflammatory bowel disease (IBD). Compared with healthy individuals, patients with IBD show marked dysbiosis, characterized by reduced microbial diversity, an expansion of facultative anaerobes such as Proteobacteria, and a depletion of obligate anaerobes within the Firmicutes phylum. These changes have been implicated in the perpetuation of intestinal inflammation, disruption of mucosal immune homeostasis, and altered metabolic functions, further underscoring the microbiota’s relevance in IBD pathophysiology. However, microbiota-driven insights have not yet been consistently translated into therapeutic stratification or clinical decision-making. A major challenge lies in the complex and dynamic interplay between the gut microbiota and various treatment modalities, including conventional immunosuppressants, biologics, and small-molecule inhibitors. While accumulating evidence suggests that IBD treatments may modulate microbial composition and function, it remains unclear whether these changes represent a direct pharmacological effect or are secondary to inflammation control. Additionally, there is a lack of comparative data on microbiota profiles associated with differential responses to various therapeutic classes, limiting the implementation of microbiota-informed precision medicine. In this review, we synthesize current evidence on the association between gut microbiota composition and treatment outcomes, focusing on biologic agents and small-molecule therapies. Furthermore, we discuss the potential of microbiota-targeted strategies, such as fecal microbiota transplantation (FMT) and precision probiotics, in enhancing therapeutic response. A deeper understanding of host-microbe interactions could enable a more personalized and effective approach to IBD management.
Bartocci B, Del Gaudio A, Murgiano M, Papa A, Cammarota G, Gasbarrini A, Scaldaferri F, Lopetuso LR
Bifidobacterium animalis subsp. lactis 832 Alleviates DSS-Induced Colitis in a Murine Model by Regulating Gut Microbiota and Phospholipid Metabolism. Microorganisms | 2026-05-11
Inflammatory bowel disease (IBD) is a chronic intestinal disorder with recurrent inflammation for which effective therapeutic options remain limited. Probiotics from the Bifidobacterium genus have potential beneficial effects on the prevention of IBD by improving intestinal barrier integrity and modulating immune responses. However, whether these effects are mediated by the regulation of gut metabolism remains largely unclear. This study was designed to explore the protective effect of an infant-derived Bifidobacterium animalis subsp. lactis 832 (B. lactis 832) on dextran sulfate sodium (DSS)-induced colitis in mice and its underlying mechanism. B. lactis 832 treatment significantly alleviated colitis severity (p < 0.05), as evidenced by reduced weight loss, disease activity index (DAI), and colonic injury, accompanied by significantly decreased pro-inflammatory cytokine expression and increased Il10 expression (p < 0.05). It also improved intestinal barrier integrity and modulated gut microbiota composition by reducing potentially pathogenic bacteria while enriching beneficial taxa. Surprisingly, metabolomic analysis revealed that B. lactis 832 intervention enhanced intestinal phospholipid metabolism, particularly increasing phosphatidylethanolamine (PE) and phosphatidylcholine (PC) levels. Notably, PE or PC supplementation recapitulated the protective effects against DSS-induced colitis (p < 0.05). These findings suggest that B. lactis 832 alleviates colitis through microbiota-associated metabolic regulation, highlighting a key role for phospholipid metabolism in mediating probiotic effects.
Chen X, Wang Q, Guo X, Li D, Wu X, Li X, Zheng X, Li Y, Han S, Feng L
Pathogenesis & Basic Science (19 papers)
Transcriptional Modulation of the Nrf2 Antioxidant Pathway and Tight Junctions by a Plant Sterol Food Supplement in an Intestinal Inflammation Coculture Model. Journal of food science | 2026-06
There is growing evidence supporting the anti-inflammatory activity of plant sterols (PS) in preclinical models of intestinal inflammation. However, the underlying mechanisms driving these beneficial effects remain incompletely understood. This study investigates the transcriptional modulatory activity of a PS food supplement (PS-FS) on genes associated with the cellular antioxidant defense system and tight junction (TJ) proteins. A double-chamber coculture model with differentiated Caco-2 cells (apical) and RAW264.7 macrophages (basolateral) was used. Bioaccessible fraction (BF) of PS-FS was obtained following the INFOGEST 2.0 simulated gastrointestinal digestion. A 1/20 dilution of BF was applied to the apical chamber for 90 min, followed by lipopolysaccharide (LPS) stimulation (1 µg/mL, 24 h) on the basolateral side. The interaction between PS-FS and budesonide was also evaluated. The gene expression of Nrf2 (NFE2L2), glutathione S-transferase A1 (GSTA1), NAD(P)H quinone dehydrogenase 1 (NQO1), and heme oxygenase 1 (HMOX-1) was quantified. Additionally, gene expression of TJ-related genes (CLDN1, CLDN3, CLDN4, OCLN, and TJP1) was quantified. Pretreatment with PS-FS significantly increased expression of GSTA1 (26.8%) and HMOX-1 (124.4%) compared to LPS + digestion blank. Furthermore, there was a trend toward increased expression of NFE2L2 and NQO1. Similarly, PS-FS enhanced expression of CLDN3 (33.0%), CLDN4 (211.7%), OCLN (57.1%), and TJP1 (98.9%). However, co-treatment of budesonide and PS-FS resulted in antagonistic interactions. These findings indicate that PS-FS modulates gene expression associated with antioxidant responses and intestinal barrier integrity-related pathways, suggesting to be further developed as a dietary strategy to support the management of inflammatory bowel disease PRACTICAL APPLICATIONS: This research supports the potential use of plant sterol-based food supplements in products aimed at supporting intestinal health. The results suggest that these supplements could help strengthen the gut barrier and support the body’s natural antioxidant defenses during intestinal inflammation.
Makran M, Giardina IC, Garcia-Llatas G, Attanzio A, Cilla A
Codonopsis pilosula as the sovereign herb in Shenling Baizhu formula ameliorates DSS-induced ulcerative colitis via spermidine-AMPK-mediated mitophagy to inhibit the cGAS-STING inflammatory axis. International immunopharmacology | 2026-05-30
Dextran sulfate sodium-induced ulcerative colitis is featured by excessive intestinal inflammation and disrupted mucosal immune homeostasis. Codonopsis pilosula is the sovereign herb in Shenling Baizhu Formula for ulcerative colitis therapy, and Codonopsis pilosula polysaccharides are its key active components, while their immunomodulatory effects and molecular mechanisms in Shenling Baizhu Formula against ulcerative colitis remain elusive. This study explored the critical role of Codonopsis pilosula polysaccharides and the spermidine-AMPK-mediated mitophagy-cGAS-STING inflammatory axis in regulating intestinal inflammation and ameliorating ulcerative colitis. A dextran sulfate sodium-induced ulcerative colitis mouse model was established to evaluate the indispensable role of Codonopsis pilosula polysaccharides in Shenling Baizhu Formula. Ultra-high performance liquid chromatography metabolomics and 16S ribosomal RNA sequencing were performed to identify key metabolites and gut microbiota. In vitro dextran sulfate sodium-induced ulcerative colitis cellular models (human colorectal adenocarcinoma Caco-2 and human normal colonic epithelial NCM460 cells) were constructed to validate the regulatory mechanism of spermidine on AMPK-mediated mitophagy, inflammatory balance and intestinal epithelial injury. Codonopsis pilosula polysaccharides were essential for the anti-ulcerative colitis efficacy of Shenling Baizhu Formula: removal of Codonopsis pilosula significantly aggravated colonic pathological lesions, intestinal inflammatory responses and oxidative stress in ulcerative colitis mice, whereas Codonopsis pilosula polysaccharides supplementation reversed these abnormal phenotypes (P < 0.05). Metabolomics and microbiomics confirmed that Codonopsis pilosula polysaccharides exerted therapeutic effects via spermidine (a key metabolite in glutamate metabolism pathway) and Muribaculaceae. Critically, in vitro dual-cell experiments verified that spermidine activated AMPK-mediated mitophagy to directly inhibit the hyperactivation of cGAS-STING inflammatory axis, thereby restoring intestinal inflammatory homeostasis and alleviating epithelial cell injury in ulcerative colitis. Codonopsis pilosula polysaccharides extracted from the sovereign herb Codonopsis pilosula in Shenling Baizhu Formula ameliorate dextran sulfate sodium-induced ulcerative colitis, and the core mechanism depends on spermidine-triggered AMPK-mediated mitophagy to suppress the cGAS-STING inflammatory signaling axis, which plays a pivotal role in regulating intestinal immunity and repairing mucosal epithelial damage.
Xi X, Li J, Wang Y, Ni Y, Zhou J, Cao L, Wei W, Gao J
RNA Helicase DDX21 Controls CD4+ T Cell Proliferation and Promotes Inflammatory Bowel Disease via Translational Control.★ Advanced science (Weinheim, Baden-Wurttemberg, Germany) | 2026-05-29
Inflammatory bowel disease (IBD) is characterized by dysregulated T cell responses. RNA helicases, including DExD-box helicase 21 (DDX21), are pivotal in RNA metabolism, but their role in T cell-mediated pathology during IBD remains unclear. Here, we demonstrate that DDX21 expression in CD4+ T cells correlates with cell cycle and translation pathways in IBD-affected tissues. Conditional deletion of Ddx21 in mouse T cells disrupts T cell homeostasis and impairs cell proliferation. Consequently, Ddx21-deficient CD4+ T cells exhibit resistance to inducing adoptive transfer colitis, with recipients showing reduced T cell infiltration compared to wild-type (WT) counterparts. Mechanistically, DDX21 ensures ribosome biogenesis after T cell activation and facilitates mRNA translation of Transcription factor dp-1 (TFDP1), a transcription factor critical for cell cycle progression. Given this dependence on ribosome biogenesis, pharmacological targeting of this pathway via KU55933-an inhibitor of ribosome synthesis-related signaling-recapitulated the protective effects of DDX21 loss: KU55933 alleviated dextran sulfate sodium (DSS)-induced colitis in mice and attenuated pathogenic CD4+ T cell expansion. Our findings establish DDX21 as a key regulator of T cell proliferation and highlight its potential as a therapeutic target for IBD and other autoimmune disorders.
Zhang Y, Kan C, Yang X, Hao Y, Cai X, Yang M, Zhang Q, Wang Z, Jiang N, Wang L
Β-Resorcylaldehyde attenuates DSS-induced colitis by inhibiting inflammation and oxidative stress through the Keap1/Nrf2/HO-1 pathway. International immunopharmacology | 2026-05-28
Ulcerative colitis (UC), a bowel condition marked by heightened oxidative stress, ongoing inflammation, and intestinal barrier dysfunction, has limited therapeutic options that are both effective and safe. This study evaluated the therapeutic impacts and mechanisms of β-Resorcylaldehyde (BRAL), the natural phenolic aldehyde derived from Morus alba wood, on dextran sulfate sodium (DSS)-induced UC. A murine DSS-induced UC model was employed to assess the therapeutic effects of BRAL by assessing disease activity, histopathology, oxidative stress, cytokine expression, and intestinal barrier integrity in vivo. To investigate the underlying molecular mechanisms, RNA sequencing, quantitative PCR, and Western blot experiments were conducted. For in vitro validation, RAW264.7 macrophages and THP-1 cells stimulated with lipopolysaccharide and intestinal epithelial cells injured by tert-butyl hydroperoxide were utilized. The assessment of target engagement was carried out using the cellular thermal shift assay, molecular docking, and molecular dynamics simulation. BRAL markedly alleviated the symptoms of DSS-induced UC, reduced oxidative stress and inflammatory reactions, along with restored tight junction protein expression. Transcriptomic and biochemical analyses indicated that BRAL suppressed pro-inflammatory cytokine production while enhancing antioxidant defenses. Mechanistically, BRAL directly bound to Keap1, thereby promoting Nrf2 nuclear translocation and Nrf2/HO-1 pathway activation. Notably, pharmacological inhibition of Nrf2 with the well-known inhibitor ML385 abolished the protective effects of BRAL. BRAL improves DSS-induced UC through targeting Keap1 to activate Nrf2 signaling, thereby restoring redox homeostasis, suppressing inflammation, and preserving epithelial barrier integrity. These findings suggest that BRAL is a promising natural candidate for treating UC.
Xiang L, Yang X, Li Q, Wang G, Hu R, Li M, Hu J, Lei H, Fan A, Gong Z
Loganin alleviates oxidative stress-induced apoptosis by modulating mitochondrial function and STAT3 signaling in DSS-induced colitis and H2O2-injured Caco-2 cells. Scientific reports | 2026-05-28
Ulcerative colitis (UC) is a chronic inflammatory bowel disease characterized by recurrent inflammation and mucosal damage. Loganin, a natural iridoid glycoside with anti-inflammatory and antioxidant properties, has shown protective effects in experimental colitis. However, its role in regulating mitochondrial dysfunction, oxidative stress-induced epithelial cell apoptosis, and barrier injury in UC remains incompletely understood. A dextran sulfate sodium (DSS)-induced colitis model was established in mice, and an H2O2-induced epithelial injury model was established in Caco-2 cells to evaluate the protective effects of loganin in vivo and in vitro. Colonic injury, oxidative stress, apoptosis, and barrier integrity were assessed by histological analysis, biochemical assays, immunofluorescence, Western blotting, flow cytometry, TEER measurement, and FITC-dextran permeability analysis. Mitochondrial dysfunction was evaluated by measuring mitochondrial membrane potential, mtROS accumulation, cytochrome c redistribution, and mitochondrial ultrastructure. In addition, network pharmacology, molecular docking, and IL-6 supplementation experiments were performed to explore the involvement of IL-6/STAT3/Bcl-2-related signaling in the anti-apoptotic effects of loganin. Loganin significantly alleviated histological damage and preserved colonic architecture in DSS-treated mice. It reduced oxidative stress, as evidenced by lower MDA levels, enhanced antioxidant enzyme activity, and improved intestinal barrier function. Loganin treatment also suppressed epithelial cell apoptosis, as shown by decreased BAX and cleaved caspase-3 levels and increased Bcl-2 expression. In H2O2-injured Caco-2 cells, loganin attenuated mitochondrial dysfunction, preserved mitochondrial membrane potential, and reduced mtROS intensity from 16.54% to 10.11%. Loganin also reduced the apoptosis rate from 29.05% to 12.68% and improved epithelial integrity. These findings support the involvement of IL-6/STAT3/Bcl-2-related signaling in the protective effects of loganin. Our findings suggest that loganin alleviates oxidative stress-induced epithelial cell apoptosis and mitochondrial dysfunction in experimental colitis models. These protective effects are associated with modulation of IL-6/STAT3/Bcl-2-related signaling. Collectively, this study extends previous evidence on the protective effects of loganin in colitis and provides additional mechanistic insight into its role in epithelial homeostasis and barrier integrity.
Li G, Zhou S, Zhao X, Cheng Y, Ma Z
MCT1-Mediated Lactate Transport Regulates Ferroptosis in Ulcerative Colitis via Histone Lactylation. Free radical biology & medicine | 2026-05-28
Ferroptosis, an iron-dependent type of controlled cell death caused by lipid peroxidation, contributes to intestinal epithelial injury in ulcerative colitis (UC). Monocarboxylate transporter 1 (MCT1) is a major monocarboxylate transporter in cells that regulates monocarboxylate metabolism in epithelial cells. However, its importance in the intestine and the underlying mechanisms are largely unknown. This study revealed that MCT1 is strongly associated with the degree of ferroptosis in individuals with colitis, and the potential mechanism through which MCT1 regulates ferroptosis caused by colonic damage was explored. In vivo, MCT1 inhibitors, exogenous lactate, and GPR81 knockout mice were used to investigate the underlying mechanism of MCT1-mediated lactate shuttling in DSS-induced colitis. To investigate the mechanism of MCT1 in TNF-α-induced ferroptosis, cells were subjected to MCT1 overexpression, treated with the ferroptosis inhibitor ferrostatin-1 (Fer-1), or exposed to lactate for 0, 4, 8, 12, 24, or 36 hours. The results revealed that MCT1 expression was downregulated in UC patients and mouse models and was correlated with increased ferroptosis. MCT1 overexpression reduced epithelial ferroptosis in vitro, whereas MCT1 inhibition exacerbated it. Lactate treatment had the greatest protective effect at 8 h (when GPX4 expression peaked). Mechanistically, extracellular lactate activates a protective GPR81/cluster of differentiation 147 (CD147) negative feedback loop to promote the translocation of MCT1 from the cytoplasm to the plasma membrane, enhancing lactate uptake. Genetic ablation of GPR81 or inhibition of MCT1 abolished this protective feedback loop. The accumulation of intracellular lactate then promotes histone H4 lysine 16 lactylation (H4K16la). Coimmunoprecipitation (co-IP) revealed that TNF-α decreased the binding between GCN5 and H4K16la, whereas lactate therapy increased this interaction. This lactylation enhances the activity of xCT, leading to increased gene expression. This study reveals a novel MCT1-lactate-epigenetic axis that mitigates UC-related ferroptosis through feedback regulation, highlighting the critical time-dependent effect of lactate.
Yan J, Wu Y, Guo Y, Liu J, Shen C, Wang R, Jiang X, Wang L
Macrophage USP9X attenuates colitis by restricting oncostatin M production via K27-linked deubiquitination of STAT1. Cellular & molecular immunology | 2026-05-28
Dysregulated posttranslational modifications drive inflammatory bowel disease (IBD) pathogenesis, yet the specific roles of deubiquitinases in intestinal macrophages remain poorly characterized. Here, we identify ubiquitin-specific peptidase 9X (USP9X) as a critical negative regulator of intestinal inflammation. USP9X expression is reduced in UC patients and inversely correlated with disease severity. Myeloid-specific deletion of USP9X exacerbates colitis in both DSS- and TNBS-induced models, whereas its overexpression ameliorates disease. Mechanistically, USP9X interacts with signal transducer and activator of transcription 1 (STAT1) and removes K27-linked polyubiquitin chains from lysine 544. The loss of USP9X enhances STAT1 nuclear translocation and transcriptional activity, resulting in the upregulation of oncostatin M (OSM) expression and exacerbating inflammation. Mutation of STAT1 at K544 attenuated both basal and USP9X knockdown-induced responses. Notably, neutralizing OSM abrogates the exacerbated colitis phenotype in USP9X-deficient mice. These findings define a USP9X-STAT1-OSM axis that connects ubiquitin editing to transcriptional regulation and represents a potential therapeutic target for IBD. USP9X suppresses STAT1 transcriptional activation by editing K27-linked ubiquitination at lysine 544 In wild-type conditions, USP9X removes K27-linked polyubiquitin chains from STAT1 at lysine 544, limiting its nuclear retention and transcriptional activity. In macrophages, loss of USP9X leads to enhanced K27-linked ubiquitination of STAT1, enhanced STAT1 nuclear translocation, and increased STAT1 occupancy at the Osm promoter, resulting in elevated OSM expression. AAV9-mediated USP9X delivery ameliorates intestinal inflammation by restoring USP9X expression. USP9X, ubiquitin-specific peptidase 9X; STAT1, signal transducer and activator of transcription 1; OSM, Oncostatin M. (Created with Biorender).
Zhang T, Meng F, Zhao W, Meng X, Xiong J, Chu F, Lan Y, Wang J, Chen Q, Zhong W
Integrated RNA-seq and network pharmacology analyses suggest PI3K-Akt and NF-κB pathway modulation in the protective effects of diosmin against experimental colitis. Food & function | 2026-05-27
Ulcerative colitis (UC), a chronic inflammatory bowel disease, remains difficult to treat due to incomplete understanding of its mechanisms and limited therapeutic options. Diosmin, a natural citrus-derived flavonoid, has shown promising anti-inflammatory effects, but its molecular mechanisms in UC are unclear. In this study, we investigated the protective role of diosmin using dextran sulfate sodium (DSS)-induced colitis in mice and LPS-stimulated HT-29 cells, integrating transcriptomic and network pharmacology analyses. Diosmin treatment significantly alleviated colitis symptoms, reduced inflammation, preserved colon length, and enhanced intestinal barrier integrity, with efficacy comparable to 5-aminosalicylic acid. RNA-seq and network pharmacology identified PI3K-Akt and NF-κB as key pathways associated with diosmin-mediated protection, while molecular docking was used as a supportive computational analysis to explore potential interactions with selected hub-associated proteins. Experimental validation confirmed that diosmin inhibited activation of PI3K-Akt-mTOR and NF-κB signaling, decreased pro-inflammatory cytokines (TNF-α, IL-1β and IL-6), increased IL-10, promoted intestinal barrier repair via upregulation of ZO-1, occludin, and E-cadherin, and suppressed apoptosis of colonic epithelial cells. Together, these findings suggest that diosmin exerts multi-target protective effects against experimental colitis by modulating inflammation, supporting barrier integrity, and regulating key signaling pathways, providing mechanistic insight into the actions of this citrus-derived bioactive compound in colitis.
Wang S, Tan C, He H, Li X, Xu M, Guo X, Liu Y, Liao F, Dong W
Reduced miR-193a-3p Modulates Cell Proliferation and Apoptosis in Inflammatory Bowel Disease via Targeting ETS1. Immunological investigations | 2026-05-27
Multiple findings have demonstrated that microRNAs (miRNAs) have a profound impact on inflammatory bowel disease (IBD) pathogenesis. This research was conceived to elucidate the regulatory function of miR-193a-3p in IBDby targeting ETS proto‑oncogene 1 and explore its potential diagnostic value. Expression of miR-193a-3p was determined by reverse transcription quantitative real‑time polymerase-chain reaction (RT‑qPCR). Cell viability, apoptosis, and inflammatory responses were measured in lipopolysaccharide (LPS)-stimulated human normal colonic epithelial FHC cells using the cell counting kit‑8 (CCK‑8) assay, flow cytometry, and enzyme‑linked immunosorbent assay (ELISA), respectively. The dual-luciferase reporter’s assay verified the targeting relationship. miR-193a-3p was downregulated whereas ETS1 was upregulated in patients with inflammatory bowel disease (IBD). Its expression was negatively correlated with IBD severity in both ulcerative colitis (UC) and Crohn’s disease (CD). In vitro, elevated miR-193a-3p alleviated LPS-induced inflammation and apoptosis and promoted cell proliferation. A negative regulatory relationship between miR-193a-3p and ETS1 was validated experimentally. miR-193a-3p overexpression inhibited LPS-mediated upregulation of ETS1. In addition, ETS1 overexpression suppressed cell proliferation and facilitated inflammation and cell apoptosis. miR-193a-3p was involved in the pathogenesis of IBD by directly targeting ETS1.
Cheng H, Xiao L, Xu T
Dietary acrylamide exposure increases susceptibility to ulcerative colitis: A comprehensive analysis from network toxicology to in vivo experimental validation. Food and chemical toxicology : an international journal published for the British Industrial Biological Research Association | 2026-05-27
Acrylamide (AA) is a contaminant present in foods cooked at high temperatures, and its formation is associated with the Maillard reaction. Ulcerative colitis (UC) is a chronic inflammatory disease of the colon mucosa with a complex pathogenesis. This study investigated the effects of AA exposure on UC and its potential mechanisms. First, network toxicology was employed to identify genes that are targets associated with both the toxicity of AA and the pathogenesis of UC, which are enriched in pathways associated with inflammatory cascades and immune cell recruitment. Then, Mendelian randomization was employed to identify two risk proteins (CCL5 and CXCL10) associated with AA and UC. Molecular docking and molecular dynamics simulations revealed that CXCL10 exhibits the strongest binding affinity with AA, and the complex is stable. Furthermore, animal studies have found that AA exposure alone does not induce typical colitis manifestations in mice. However, AA exposure exacerbated the colitis phenotype in the DSS-induced model. CXCL10 has been identified as a potential key target in the process by which AA increases susceptibility to UC. These findings provide scientific grounds for reassessing the safety of AA and offer new insights into understanding the environmental risks of UC and potential intervention targets.
Cui P, Guo B, Yu K, Li Y
miR-16-2-3p enhances glucocorticoid sensitivity in ulcerative colitis by targeting CREB1 and NF-κB1. Human cell | 2026-05-27
In this study, we systematically investigated the role of miR-16-2-3p, a microRNA passenger strand derived from the MIR16-2 hairpin, in glucocorticoid resistance (GCR) and its underlying regulatory mechanisms. The results showed that miR-16-2-3p expression was significantly downregulated in patients with GCR and in glucocorticoid-resistant-like inflammatory models, and was positively correlated with glucocorticoid receptor (GR) expression, accompanied by a reduced responsiveness to the glucocorticoid dexamethasone (Dex). Functional experiments demonstrated that overexpression of miR-16-2-3p enhanced the inhibitory effects of Dex on inflammatory cytokines (interleukin [IL]-1β, IL-6, IL-8, and tumour necrosis factor alpha [TNF-α]) and promoted nuclear translocation of the GR, whereas inhibition of miR-16-2-3p expression attenuated the anti-inflammatory effects of Dex. Mechanistically, cAMP response element-binding protein 1 (CREB1) was identified as a direct target of miR-16-2-3p, and CREB1 silencing promoted GR nuclear translocation and enhanced the anti-inflammatory efficacy of Dex. In addition, miR-16-2-3p further suppressed nuclear factor kappa-B (NF-κB) signalling by targeting NF-κB1 (p105), thereby synergistically strengthening the inhibitory effect of Dex on NF-κB. In vivo, overexpression of miR-16-2-3p significantly improved the pathological phenotype of dextran sulphate sodium (DSS)-induced ulcerative colitis (UC) in mice and enhanced the therapeutic effect of Dex. Our findings revealed a dual molecular mechanism by which miR-16-2-3p enhances glucocorticoid sensitivity (GCS) through targeting CREB1 and NF-κB1, providing experimental evidence for its potential as a novel therapeutic agent for GCR.
Yang T, Luo J, Tang J, Wu J, Xia S, Li M, Huang Q, Yang G, Miao J, Zhu Y
Tangeretin, a bioactive polymethoxyflavone from immature Citrus aurantium L. fruit, ameliorates experimental colitis by targeting the macrophage β2 integrin Mac-1. Journal of ethnopharmacology | 2026-05-26
Zhiqiao, the dried immature fruit of Citrus aurantium L., is a traditional Chinese medicine widely used for treating gastrointestinal disorders. Among its varieties, Quzhiqiao, a geo-authentic herb from Quzhou, China, is highly valued for its superior quality, yet the pharmacological basis for its efficacy in inflammatory bowel disease remains unclear. This study aimed to investigate the therapeutic effects and underlying molecular mechanisms of the ethanol extract of Quzhiqiao (QZCEE) and its key bioactive compound in a mouse model of ulcerative colitis (UC), with a focus on its impact on macrophage-driven inflammation. The efficacy of orally administered QZCEE and its constituent, tangeretin, was evaluated in a dextran sulfate sodium (DSS)-induced colitis mouse model by assessing clinical (DAI score) and pathological (colon length, histology) parameters. Intestinal barrier integrity was examined by Western blot and qPCR. Macrophage infiltration and colonic inflammatory responses were measured by immunohistochemistry, ELISA, and qPCR. The effects of QZCEE and tangeretin on macrophage adhesion, migration, and chemotaxis were assessed in vitro using bone marrow-derived macrophages (BMDMs). The molecular target was identified and validated through molecular docking, pull-down, cellular thermal shift assay (CETSA), drug affinity responsive target stability (DARTS) assay, and Microscale Thermophoresis (MST) assays. The downstream signaling pathway was investigated by Western blot and Rac1 activation assays. Oral administration of QZCEE significantly ameliorated the severity of DSS-induced colitis, evidenced by reduced DAI scores, restored colon length, and alleviated histological damage. QZCEE also repaired the intestinal barrier by upregulating the expression of tight junction proteins ZO-1 and Occludin. Mechanistically, QZCEE markedly suppressed the infiltration of F4/80+ macrophages into the inflamed colon and inhibited the production of pro-inflammatory cytokines (TNF-α, IL-1β, IL-6). Intriguingly, QZCEE did not reduce colonic CCL2 levels but directly inhibited macrophage chemotaxis in vitro. Tangeretin, a polymethoxyflavone in QZCEE, was identified as the key bioactive compound responsible for this effect. We provided compelling evidence that tangeretin directly binds to the β2 integrin Mac-1 (αMβ2) with a dissociation constant (Kd) of 3.87 μM, thereby blocking its interaction with ICAM-1 and suppressing the downstream Vav1/Rac1 signaling pathway. Importantly, oral administration of tangeretin alone recapitulated the therapeutic and immunomodulatory effects of the QZCEE extract in vivo. Our findings demonstrate that the geo-authentic herb Quzhiqiao exerts potent anti-colitis effects. This therapeutic action is primarily mediated by its bioactive compound, tangeretin, which functions as a novel, direct antagonist of the β2 integrin Mac-1. By blocking macrophage recruitment, tangeretin represents a promising natural lead compound for the development of targeted therapies for UC. This study provides a robust scientific rationale for the ethnopharmacological use of Quzhiqiao and unveils a precise molecular mechanism for its efficacy.
Zhu J, Zhu X, Lin X, Zhou Q, Chen W, Liu Y, Cao P, Wu L, Xu J, Tong H
Not all gut cellular circadian oscillators are food entrainable. Proceedings of the National Academy of Sciences of the United States of America | 2026-05-26
Circadian rhythms are ubiquitous, and most of the organs in the body contain circadian oscillators. The intestine comprises diverse cell types with distinct developmental origins and physiological functions. However, which intestinal cells contain cell-autonomous circadian oscillators and how circadian oscillators in distinct intestinal cell types synchronize with one another and with environmental daily cycles remain poorly understood. To address these questions, we generated a Cre-dependent PER2::LUCIFERASE reporter knock-in mouse that enables ex vivo measurement of circadian oscillations in defined cell populations. Ex vivo gut explants from mice expressing the reporter in one of five major cell types of the muscularis externa-enteric neurons (ENs), enteric glial cells (EGCs), interstitial cells of Cajal (ICCs), smooth muscle cells (SMCs), and muscularis macrophages (MMs)-exhibited robust, self-sustained circadian bioluminescence rhythms, demonstrating that each of these cell types harbors a cell-autonomous circadian oscillator. Importantly, circadian oscillators in ENs, EGCs, SMCs, and MMs entrained to feeding-fasting cycles, whereas circadian oscillators in ICCs remained resistant to food entrainment. These findings reveal that distinct intestinal cell types possess unique entrainment properties, and feeding during inactive time induces heterogeneous phase shifts across gut circadian oscillators, leading to temporal circadian misalignment within the intestine. As circadian disruptions, such as those associated with shift work, contribute to intestinal disorders, including inflammatory bowel disease and disorders of the gut-brain interaction, studying how intercellular circadian desynchrony influences intestinal homeostasis should provide chronobiology-based therapeutic strategies to combat these diseases.
Magaña I, Taufique SKT, Shan Y, Shen M, Ehichioya DE, Takahashi JS, Yamazaki S, Obata Y
MODULATING OXIDATIVE STRESS AND INFLAMMATION: SODIUM BUTYRATE’S THERAPEUTIC PROMISE IN EXPERIMENTAL COLITIS. Arquivos de gastroenterologia | 2026-05-25
Oxidative stress and excessive cytokine signalling are central to the pathogenesis of ulcerative colitis (UC). Sodium butyrate (SB) has emerged as a potential therapeutic candidate due to its antioxidant and anti-inflammatory properties. UC was induced in Swiss albino mice using dextran sulfate sodium (DSS). Experiment groups included normal control (NC), DSS, DSS + SB, and DSS + 5-ASA. Clinical severity was assessed by the disease activity index (DAI) and colon length. Oxidative stress (MDA, MPO), antioxidants (SOD, GSH), Pro-inflammatory cytokines (TNF-α, IL-6), and histopathological scoring were assessed. Increased DAI and shortening of the colon length with significantly elevated TNF-α and IL-6 levels and MDA and MPO, along with reduced GSH and SOD levels, which reflect oxidative damage and inflammation induced by DSS administration. Whereas treatment with SB therapy has been shown to lower DAI, preserve colon length, minimize MDA and MPO, restore GSH and SOD activity, and ameliorate cytokine levels, with effects comparable to those of 5ASA. In DSS-induced colitis, the SB effectively attenuated oxidative stress and pro-inflammatory cytokine responses by restoring redox balance and preserving mucosal architecture. These findings suggest that administering SB as a supplementary treatment may be a viable option for managing UC. O estresse oxidativo e a sinalização excessiva de citocinas são centrais na patogênese da colite ulcerativa (CU). O butirato de sódio (BS) tem emergido como um potencial candidato terapêutico devido às suas propriedades antioxidantes e anti-inflamatórias. A CU foi induzida em camundongos albinos suíços utilizando sulfato de dextrano sódico (DSS). Os grupos experimentais incluíram controle normal (CN), DSS, DSS + BS e DSS + 5-ASA. A gravidade clínica foi avaliada pelo índice de atividade da doença (DAI) e pelo comprimento do cólon. Foram avaliados o estresse oxidativo (MDA, MPO), os antioxidantes (SOD, GSH), as citocinas pró-inflamatórias (TNF-α, IL-6) e o escore histopatológico. Observou-se aumento do DAI e encurtamento do cólon, com elevação significativa de TNF-α e IL-6, MDA e MPO, acompanhados de redução de GSH e SOD, refletindo dano oxidativo e inflamação induzidos pelo DSS. O tratamento com BS reduziu o DAI, preservou o comprimento do cólon, diminuiu MDA e MPO, restaurou a atividade de GSH e SOD e melhorou os níveis de citocinas, com efeitos comparáveis aos do 5-ASA. Na colite induzida por DSS, o BS atenuou efetivamente o estresse oxidativo e as respostas de citocinas pró-inflamatórias ao restaurar o equilíbrio redox e preservar a arquitetura da mucosa. Esses achados sugerem que a administração de BS como terapia adjuvante pode ser uma opção viável para o manejo da CU.
Murshed NMF, Swaroopa S, Al-Awadhi SSA, Poonacha SK, D’Souza C, Hosapatna Laxminarayana KP
Microbiota-derived butyrate inhibits colonic epithelial pyroptosis and mitigates DSS-induced colitis via interacting with aryl hydrocarbon receptor. Journal of translational medicine | 2026-05-23
Intestinal barrier defects cause antigen translocation and immune dysregulation. The pyroptosis of colonic epithelial cells (CECs) disrupts the colonic barrier, and its inhibition might be a therapeutic approach for ulcerative colitis (UC), but the mechanisms are not fully understood. A DSS-induced UC model was established to assess the level of colonic epithelial cell pyroptosis. 16S rDNA sequencing and LC‒MS/MS were applied to screen potential candidate bacterial species and metabolites. The roles of target metabolites were evaluated in vivo using GSDMD-knockout mice. FHC cells treated with LPS + ATP were used as a cellular model of pyroptosis, and the underlying molecular mechanism was explored mainly by siRNA transfection and lentivirus infection. We found that DSS-treated mice exhibited increased levels of pyroptosis in the colon. Fecal microbiota transplantation (FMT) significantly suppressed mucosal inflammation and CEC pyroptosis, accompanied by increased levels of butyrate-producing bacteria and butyrate in feces. Butyrate treatment alleviated DSS-induced colitis in mice. Moreover, GSDMD knockout mitigated DSS-induced colitis in mice, whereas a butyrate intervention failed to further ameliorate colitis in GSDMD-knockout mice. Mechanistically, we found that butyrate significantly inhibited LPS + ATP-induced pyroptosis by activating its receptor, aryl hydrocarbon receptor (AhR), in FHC cells, while silencing AhR suppressed this effect. The overexpression of cGAS in FHC increased the level of pyroptosis, whereas the administration of butyrate inhibited the activation of the cGAS-STING pathway. Treatment with a cGAS inhibitor significantly reversed the increase in pyroptosis caused by AhR knockdown in pyroptotic FHC cells. Gut microbiota-derived butyrate levels were increased after FMT. Butyrate suppressed the proinflammatory cGAS-STING-NF-κB signaling axis via AhR to inhibit CEC pyroptosis and thereby alleviate UC.
Zou F, Wu Z, Wang S, Xu M, Xia P, Hu Y, Fang T, Hu P, Huang C, Deng F
Oral ROS-responsive hydrogel with sulfur-doped ginger carbon dots for modulating oxidative stress and restoring gut homeostasis in inflammatory bowel disease. Colloids and surfaces. B, Biointerfaces | 2026-05-21
Inflammatory bowel disease (IBD) involves a complex inflammatory environment marked by excessive oxidative stress, impaired barrier function, and microbial imbalance. These interconnected pathologies are difficult to address with conventional single-target therapies. To tackle these challenges, this study developed an intelligently responsive oral hydrogel delivery system based on sulfur-doped ginger carbon dots (SGCDs). SGCDs, synthesized via a hydrothermal method, not only exhibited remarkable antioxidant capacity but also demonstrated multiple enzyme-like activities, including SOD-like and CAT-like, along with stable fluorescence imaging properties. Simultaneously, thiolated hyaluronic acid (HS1:6), exhibiting ROS-responsive gelation properties, was synthesized via chemical modification and employed as the gel matrix. The oral precursor system (HS1:6@SGCDs), constructed by loading SGCDs into the HS solution, underwent ROS-triggered in situ gelation upon reaching the colonic inflammatory region. This transformation formed a physical barrier, prolonged retention time, and enabled controlled release of SGCDs. This system significantly alleviated pathological symptoms through multiple mechanisms, including efficient scavenging of excessive ROS, modulation of the immune microenvironment, amelioration of intestinal barrier dysfunction, and amelioration of dysbiosis with a trend toward recovery of a more balanced microbial community. Through disease-directed and source-based innovation, the system combined targeted material design with multifunctional therapeutic capabilities. Thus, HS1:6@SGCDs provided an innovative and comprehensive solution for the treatment of IBD.
Liu B, Rui S, Bian D, Wang J, Feng S, Liu Z, Yang Y, Gong W, Wan L, Zhang J
A novel peptide from Periplaneta americana: Development of a long-acting formulation for ulcerative colitis therapy. Biomaterials advances | 2026-05-21
Ulcerative colitis (UC) brings a heavy burden to patients due to its long course, difficulty in cure, high relapse rate, and high carcinoma rate. Limitations of conventional drugs, including poor compliance and high recurrence, are now being addressed by modern approaches like immune-modulating therapies and refined surgical techniques. Therefore, there is an urgent clinical need for a new therapeutic strategy that is safe, long-acting, and has good compliance. In this study, we extracted and fractionated an peptide PAE-P6 with significant anti-inflammatory activity from Periplaneta americana extract (PAE), and it showed certain therapeutic effect in UC mice. To enhance the efficacy and stability of peptides in vivo, we further developed this peptide into a long-acting thermosensitive liposome gel formulation. Following rectal administration, this formulation demonstrated remarkable efficacy in a mouse model of UC by boosting the expression of anti-inflammatory factors, repairing tight junctions, regenerating mucin, and inhibiting the expression of pro-inflammatory factors. This study offers a promising strategy for targeted and sustained drug delivery in UC treatment.
Lv T, Liu H, Zhang Y, Yuan M, Wang Y, Chen Z
Progressive Myopenia and Functional Decline in the Winnie Mouse Model of Chronic Colitis. Muscles (Basel, Switzerland) | 2026-05-12
Muscle wasting contributes substantially to inflammatory bowel disease (IBD)-related disability, but its association with colitis severity across disease stages remains poorly characterized. We therefore assessed skeletal muscle mass, fiber morphology, and voluntary wheel-running performance in Winnie mice-a spontaneous Muc2 mutant model of chronic colitis-in separate female and male homozygous mutant and WT littermate cohorts. Assessments were performed at 5 weeks, before overt colitis, and at 15 weeks, in a cohort with more pronounced colitis. Outcomes included disease activity index (DAI), fecal lipocalin-2 (LCN-2), wheel-running metrics, soleus and tibialis anterior mass, and minimal Feret’s diameter distributions. At 5 weeks, Winnie mice showed no overt disease activity and no consistent structural muscle deficit. In contrast, the 15-week cohort exhibited marked colitis in both sexes, with increased DAI and LCN-2, reduced voluntary wheel-running performance, lower soleus and tibialis anterior mass, and smaller muscle fiber diameters with left-shifted size distributions. Correlation analyses identified associations between fecal LCN-2, skeletal muscle mass and size, and wheel-running distance and velocity, supporting a link between intestinal inflammation and muscle impairment in this model. These cross-sectional data are consistent with reduced voluntary activity and structural myopathy during progression of spontaneous colitis. The Winnie mouse model therefore provides a clinically relevant preclinical platform to study IBD-associated muscle wasting and its association with intestinal inflammation.
Sharma S, Debruin D, Devereaux J, Hayes A, Nurgali K, Duque G
6-Bromoindole-3-acetonitrile Attenuates DSS-Induced Colitis by Inhibiting Epithelial Cell Pyroptosis. Foods (Basel, Switzerland) | 2026-05-12
Ulcerative colitis is a chronic inflammatory bowel disease that requires new treatment approaches beyond traditional anti-inflammatory drugs. In this study, we analyzed publicly available single-cell RNA sequencing data from a DSS-induced colitis mouse model and identified pyroptosis as a key biological process linked to epithelial damage. Based on this, we screened marine-derived brominated indoles for potential pyroptosis inhibitors and identified 6-bromoindole-3-acetonitrile as a promising candidate. Our results show that this compound significantly alleviates DSS-induced colitis in mice, with notable body weight recovery and a drop in Disease Activity Index (DAI) scores from about 8.5 to below 4 (p < 0.05). At the molecular level, it lowers the mRNA levels of Nlrp3, Caspase-1, and other pyroptosis-related genes, indicating suppression of the pyroptotic pathway. Moreover, treatment helps restore the intestinal barrier by supporting goblet cell regeneration and strengthening tight junctions. Molecular docking suggests that 6-bromoindole-3-acetonitrile binds stably to the active site of myeloperoxidase (MPO), with a binding energy of -18.1 kcal/mol, offering a possible structural basis for its anti-inflammatory effects. Together, these findings point to a marine-derived compound that reduces both inflammation and pyroptosis, representing a promising strategy for treating ulcerative colitis. Notably, these results come from preclinical studies and need further validation in clinical settings.
Hong D, Yang X, Chang Z, Yuan L, Du M, Cheng S
Therapeutics & Mechanisms (15 papers)
Vedolizumab for the prevention and treatment of postoperative recurrence in Crohn’s disease: A real- world latium net study. Digestive and liver disease : official journal of the Italian Society of Gastroenterology and the Italian Association for the Study of the Liver | 2026-05-30
Vedolizumab has demonstrated efficacy in randomized trials on postoperative Crohn’s disease; however, real-world data on both prophylaxis and treatment of recurrence are limited. In this retrospective multicenter study, patients with Crohn’s disease treated with vedolizumab after ileocolonic resection (2018-2024) were included. Patients were stratified into a prophylaxis cohort and a recurrence-treatment cohort. Severe endoscopic recurrence (Rutgeerts ≥i3) at 6-12 months was the primary endpoint in the prophylaxis cohort. Endoscopic response (≥1-point Rutgeerts reduction) at a follow-up colonoscopy within 2 years, was evaluated in the treatment cohort. Treatment failure was defined as discontinuation of vedolizumab due to any reason. Treatment persistence was analyzed using Kaplan-Meier and multivariable Cox regression models. A total of 108 patients were included; 50 received vedolizumab as postoperative prophylaxis. Severe endoscopic recurrence occurred in 22% of prophylaxis patients. Prior intestinal resection (OR 5.24, 95% CI 1.03-26.61; p = 0.046) and younger age at surgery (OR 0.93, 95% CI 0.87-0.99; p = 0.042) were independently associated with severe recurrence. In the recurrence cohort (n = 58), endoscopic response was 44.8%. Overall VDZ failure occurred in 31.5%. Prophylactic use was independently associated with reduced failure (HR 0.17, 95% CI 0.05-0.53; p = 0.002). Vedolizumab showed sustained effectiveness for postoperative prophylaxis and more modest effectiveness in established recurrence.
Gaudio AD, Calabrese E, Balestrieri P, Pugliese D, Fiorino G, Vincenzo FD, Marafini I, Baldaro F, Cuccia G, Cascella F
Th1/Th17 cytokine signatures correlate with Crohn’s disease activity in a 54‑week cohort of patients treated with adalimumab. Biomedicine & pharmacotherapy = Biomedecine & pharmacotherapie | 2026-05-29
Crohn’s disease (CD) is a chronic inflammatory disorder of the gastrointestinal tract with a relapsing-remitting course. Cytokine dysregulation plays a central role in its pathogenesis, and biological therapies-such as anti‑TNFα agents, vedolizumab, and anti‑IL‑23 monoclonal antibodies-have improved disease control. However, variability in therapeutic response underscores the need for biomarkers to support personalized treatment strategies. A longitudinal study was conducted in 26 patients with clinical‑remission/mild‑activity CD who were treated with adalimumab over 54 weeks. Serum samples were collected at baseline, week 14, and week 54. Eighteen cytokines were quantified using high‑sensitivity Luminex MAP technology. TNFα values were excluded due to drug interference. Clustering and PERMANOVA analyses were used to explore cytokine profiles and their association with disease activity. Four cytokine clusters were identified: Th1‑like, Th2‑like, Th17‑like, and a mixed inflammatory profile including IL‑1β, IL‑2, IL‑12, IL‑21, and IL‑23. Significant reductions in CDAI, C‑reactive protein (CRP), and fibrinogen were observed during treatment. IL‑2, IL‑10, and CCL20 levels increased significantly in patients with active CD (CDAI ≥ 150). Th1 and Th17 signatures were positively correlated with disease activity. Serum assessment of Th1 (IL‑1β, IL‑7) and Th17 (GM‑CSF) signatures generated ROC curves with an AUC of 0.795, compared with CRP (AUC = 0.686) and fibrinogen (AUC = 0.774). Serum cytokine profiling reveals immunological heterogeneity in CD patients treated with adalimumab and may serve as an exploratory biomarker of disease activity and therapeutic response; however, these findings are hypothesis generating and require validation in larger, independent cohorts before clinical applicability can be established.
de Castro-Martínez P, Guijarro LG, Monserrat J, Chaparro M, Guerra I, Iborra M, Cabriada JL, Bujanda L, Alba C, García-Sánchez V
Human factors validation study of a disposable autoinjector (Bmab 1200 autoinjector) for subcutaneous delivery of Ustekinumab.★ Drug delivery | 2026-05-29
Ustekinumab is approved for treating moderate to severe plaque psoriasis, psoriatic arthritis, Crohn’s disease, and ulcerative colitis. The Bmab 1200 autoinjector is a simple, two-step device for subcutaneous ustekinumab biosimilar delivery. This was an in vitro, nonclinical, simulated-use human factors validation study to evaluate if intended users could safely and effectively use it. Ninety participants (recruited via purposive sampling) were enrolled (mean age: 43 years; range: 12-72 years), including adult and adolescent patients, lay caregivers, and healthcare professionals. Without formal training, participants performed simulated injections into foam pads. Test personnel observed, documented, debriefed, and reported any errors made by participants while completing assigned tasks and sub-tasks. Each participant was observed throughout the session and observational and performance data were collected in real time by data logger. Performance measures included injection success rates, use errors, and 24 knowledge tasks. Across these knowledge tasks, participants were required to locate, identify, and understand 28 distinct measures. Participants also provided feedback on usability and confidence levels. All participants (100%) completed unaided dose injections. A total of 20 use errors were documented: hand hygiene (n = 8), site preparation (n = 5), and device handling (n = 7), none causing device damage or failed delivery. The knowledge task success rate was 99.6% (2,511/2,520 measures). Nine use errors (study artifacts or inattention to instructions) occurred only among caregivers. All participants expressed confidence in safe dosing and found the device user-friendly. The Bmab 1200 autoinjector demonstrated high usability and safety across diverse users for ustekinumab biosimilar delivery in chronic autoimmune conditions.
Moses K S, Kamaraj R, Konda Ramachary Subramanian S
Non-cirrhotic hepatocellular carcinoma during Crohn’s disease therapy with azathioprine : possible involvement of focal hepatocyte glycogenosis in hepatocarcinogenesis. Clinical journal of gastroenterology | 2026-05-29
Hepatocellular carcinoma (HCC) rarely develops in patients with Crohn’s disease (CD) without cirrhosis. Focal hepatic glycogenosis (FHG), characterized by localized hepatocellular glycogen accumulation, has been proposed as a potential preneoplastic lesion, particularly in the setting of long-term azathioprine (AZA) therapy. We report two non-cirrhotic CD patients who developed HCC during prolonged AZA treatment; both exhibited FHG in their background livers. A review of the literature identified only 13 previously reported HCC cases in CD patients, most of which were associated with AZA use or FHG. These findings suggest a possible link between CD, AZA therapy, FHG, and hepatocarcinogenesis. Long-term AZA therapy in CD may be involved in the development of FHG and may contribute to HCC development, even in non-cirrhotic livers, underscoring the need for careful liver surveillance in CD patients receiving prolonged AZA treatment.
Fujii H, Sawada K, Ueno N, Ando K, Izumi K, Hayashi H, Ota Y, Hayashi M, Yokoo H, Fujiyaï M
Engineered Microparticle Morphology for Enhanced Intestinal Retention in Oral Drug Delivery. Acta biomaterialia | 2026-05-29
Microparticle-based drug delivery systems have gained widespread recognition for their ability to enable sustained drug release. However, their utility in oral administration has been constrained by suboptimal gastrointestinal retention. This study systematically evaluated how engineered microparticle morphology and surface topography influence intestinal adhesion dynamics and drug release profiles. Through controlled modulation of surface roughness and particle geometry, we demonstrated that non-spherical architectures, particularly waterdrop-like microparticles (WDMPs), exhibited superior mucoadhesive properties, achieving 1.25-fold prolonged gastrointestinal retention time while maintaining optimal drug release kinetics (71.2% cumulative release over 10 hours). In a murine inflammatory bowel disease (IBD) model, dexamethasone (DXM)-loaded WDMPs outperformed conventional free drug administration, manifesting in significantly improved therapeutic outcomes: 1.16-fold enhanced weight recovery, 1.27-fold greater colon length preservation, and superior histopathological scores. Notably, WDMPs also boosted oral bioavailability of micronutrients by 1.2-to-1.6-fold, highlighting its dual applicability for both pharmaceutical and nutraceutical delivery. These comprehensive findings positioned WDMPs as a transformative oral delivery platform that addresses longstanding challenges in gastrointestinal drug absorption, offering substantial potential for clinical translation. STATEMENT OF SIGNIFICANCE: This study demonstrates the potential of engineered microparticle morphology to address key challenges in oral drug delivery. By investigating the effects of particle morphology and surface topography on intestinal retention and drug release, we show that non-spherical, rough microparticles exhibit enhanced mucoadhesion and sustained drug release. Waterdrop-like Microparticles (WDMPs) provide a significant improvement in gastrointestinal retention and drug release kinetics. WDMPs also outperform free dexamethasone in a murine model of inflammatory bowel disease. Additionally, WDMPs enhance oral bioavailability for micronutrients, offering dual-purpose potential for pharmaceutical and nutraceutical applications. These findings highlight the critical role of microparticle morphology in optimizing drug delivery efficiency and underscore the versatility of WDMPs as a customizable platform for controlled release therapies.
Yang Y, Xiao Z, Chen L, Miao Y, Wu Z, Ma B, Chen Q, Yang Y
Comparison of Ustekinumab and Vedolizumab Effectiveness in Perianal Crohn’s Disease: A Retrospective Propensity Matched Cohort Study. Journal of clinical gastroenterology | 2026-05-28
Perianal Crohn’s disease (PCD) is a severe and disabling phenotype of Crohn’s disease that often requires multidisciplinary medical and surgical management. Although ustekinumab (UST) and vedolizumab (VDZ) are widely used after antitumor necrosis factor (anti-TNF) failure, direct comparative data specifically in PCD remain limited. We conducted a multicenter, retrospective cohort study using the TriNetX US Collaborative Network to compare the effectiveness of UST versus VDZ in adults (18 y or older) with PCD between January 2017 and May 2023. Outcomes were perianal-specific clinical events, including definitive fistula surgery, incision and drainage, diversion procedures, and antibiotic use (metronidazole or ciprofloxacin), assessed at 1 and 2 years after biological initiation. Propensity score matching (PSM) (1:1) was performed to balance baseline variables. Time-to-event analyses were conducted in the matched population using Kaplan-Meier methods, and hazard ratios (HRs) were estimated using Cox proportional hazards models within the matched cohorts. A total of 2936 patients were identified before PSM: 1997 patients in the UST group and 939 patients in the VDZ group. After PSM, 936 patients were included in each cohort. In the matched cohorts, UST was associated with significantly lower risk of definitive perianal fistula surgery (HR: 0.66, 95% CI: 0.50-0.89; P<0.01), and composite surgical events (HR: 0.70, 95% CI: 0.54-0.87; P<0.01) compared with VDZ at 1 year. Rates of antibiotic use, incision and drainage of perianal abscess, and diversion procedures were numerically lower but not statistically significant. At 2 years, these findings persisted, with significantly lower cumulative incidence of definitive perianal fistula surgery (HR: 0.78, 95% CI: 0.61-0.90; P=0.03), composite surgical events (HR: 0.81, 95% CI: 0.69-0.90; P<0.01), and antibiotic use (HR: 0.86, 95% CI: 0.75-0.93; P=0.04) in the UST cohort compared with VDZ. Rates of incision and drainage and diversion procedures remained similar between groups. In this large real-world cohort, UST was associated with lower risks of perianal surgical interventions at one and two years and reduced antibiotic utilization at two years compared with VDZ in patients with PCD. These findings highlight meaningful differences in real-world effectiveness between therapies and support the need for prospective studies to further evaluate comparative effectiveness in this population.
Eldesouki MH, Rabea E, Aldemerdash MA, Tageldin O, Seminerio J, Farraye FA, Hashash JG
Comment on “Real-world outcomes of ustekinumab, vedolizumab, and tumor necrosis factor inhibitors in very-early-onset inflammatory bowel disease”: treatment comparison or treatment sequencing?Letter Journal of gastroenterology | 2026-05-27
A decade of clinical data with vedolizumab: the past, present, and future.Review Therapeutic advances in gastroenterology | 2026-05-25
Inflammatory bowel disease (IBD) is a chronic inflammatory disorder of the gastrointestinal tract, typically classified as either ulcerative colitis (UC) or Crohn’s disease (CD). The treatment approaches for both UC and CD have changed substantially over the last 10 years, going from step-up to top-down approaches and culminating in treat-to-target algorithms. In addition to the evolution of treatment strategies for IBD, disease endpoints have also changed from symptom-based outcomes to more objective measures, including endoscopy, with histology and transmural healing currently under investigation. In this narrative review, we describe recent advances in the treatment of patients with IBD, with a focus on vedolizumab, the first and only anti-lymphocyte trafficking agent approved as a gut-selective biologic for induction and maintenance therapy in IBD. Furthermore, with the approval of more biologic agents, there remains a need to determine the sequence in which biologics should be used, both individually and in combination. Substantial progress has been made in the last decade, and even though biomarkers and algorithmic trials have been largely disappointing, other avenues, such as clinical decision support tools, prognostic tools, and new approaches incorporating computational biology, have the potential to more effectively curate a tailored approach to IBD therapy in the coming years. A decade of progress: how vedolizumab has changed research and medical care for people with inflammatory bowel disease Inflammatory bowel disease, also known as IBD, is a life-long illness caused by inflammation of the gut. This means that the gut becomes swollen and irritated. For reasons we don’t understand, the immune system makes gut inflammation worse over time. In 2014, a medication called vedolizumab was approved for IBD. Vedolizumab works by preventing certain immune cells from reaching the gut, which can help reduce inflammation. This review describes improvements in IBD treatment over the last 10 years, with a focus on vedolizumab. Studies have shown that a person’s symptoms don’t always tell doctors if their IBD is getting better or worse. Instead, experts say that treatments should aim to heal the gut, not just reduce symptoms of IBD. Many studies using vedolizumab have looked at gut healing in people with IBD. Also, many new medications for IBD have become available in the last decade. However, doctors need better guidance on when to use each medication, in what order, and whether they can be used together. Research has looked at how well these medications, including vedolizumab, work and how safe they are. This information can help doctors create better step-by-step treatment plans for people with IBD. Looking to the future, doctors hope to choose medications based on what will work best for each person. This is called precision medicine. To support this, researchers have created a tool that can help doctors predict how well someone will respond to vedolizumab by using details about their medical history. Overall, our understanding of IBD and how to treat it has changed a lot in the last 10 years. Vedolizumab will continue to play an important role in IBD research and patient care.
Jairath V, Armuzzi A, Agboton C, Bressler B, Danese S, Dulai PS, Meyer M, Bautista IR, Atreya R, Feagan BG
Positioning of advanced therapies in patients with moderate-to-severe Crohn’s disease.Review Singapore medical journal | 2026-05-25
The treatment landscape for Crohn’s disease (CD) has evolved substantially in the 21st century with the advent of advanced therapies. Since the introduction of tumour necrosis factor (TNF) antagonists, new classes of advanced CD therapies have been approved for use in the Asia-Pacific region, including anti-integrins, interleukin (IL)-12/23p40 inhibitors, IL-23p19 inhibitors and Janus kinase inhibitors (JAKi). In the last 10 years, biosimilars to infliximab, adalimumab and ustekinumab and generic JAKi have also become available. In this review, we discuss the indications for advanced therapies and whether certain classes of drugs are preferred for specific patient subsets. We also discuss the choice of first- and second-line agents for CD.
Qiu TY, Tan CK, Ong JPL, Ling KL
Pairwise Comparative Safety and Effectiveness of Anti-TNF Blockers, Vedolizumab, and Ustekinumab During Pregnancy: A Systematic Review and Meta-Analysis.Review Digestive diseases and sciences | 2026-05-25
Biologic therapies, including tumor necrosis factor (TNF) blockers, vedolizumab (VDZ), and ustekinumab (UST), are generally considered safe during pregnancy in patients with inflammatory bowel disease (IBD), though comparative data remain limited. This meta-analysis examines their safety and effectiveness. A systematic search of MEDLINE, EMBASE, CINAHL, Cochrane, and Web of Science was conducted through July 2025. Eligible studies reported maternal or neonatal outcomes in pregnant IBD patients treated with biologics. Studies were pooled using a random-effects model to calculate risk ratios (RRs) with 95% confidence intervals. Heterogeneity was assessed using I2. Primary outcomes were preterm birth and disease activity; secondary outcomes included pregnancy and neonatal outcomes. Nine observational studies (n = 6,054) were included. Compared to TNF blockers, VDZ was associated with a higher risk of preterm delivery (RR = 1.35, 95% CI 1.04-1.75, I2 = 0%) and active disease (RR = 1.55, 95% CI 1.01-2.40, I2 = 50%). UST was associated with a higher risk of active disease (RR = 1.30, 95% CI 1.06-1.60, I2 = 0%) and congenital anomalies (RR = 2.08, 95% CI 1.30-3.32, I2 = 0%) compared to TNF blockers. Compared to UST, VDZ was linked to increased risks of preterm birth (RR = 2.60, 95% CI 1.03-6.57, I2 = 0%) and low birth weight (RR = 2.38, 95% CI 1.01-5.60, I2 = 0%). No significant differences were observed for live births, abortions, hospitalizations, or neonatal infections. TNF blockers showed a favorable safety and effectiveness profile, VDZ and UST performed broadly similar, and all three biological classes appeared compatible with safe use in pregnancy to maintain effective disease control. Observed differences reflect that VDZ and UST cohorts likely had longer disease duration, prior biologic exposure, and more active disease. The results of this meta-analysis support the continuation of biologic therapy for disease control in pregnant patients with IBD. Treatment decisions should be individualized and tailored to each patient’s clinical context.
Segun-Omosehin O, Bourdakos NE, Tzanis KG, Macaron MM, Jamal F, Marks L, Hamad A, Malik TA
Regression of vascular wall thickening with upadacitinib in a patient with clinically silent pediatric-onset takayasu arteritis and ulcerative colitis: case-based review. Clinical journal of gastroenterology | 2026-05-25
The coexistence of Takayasu arteritis (TAK) and ulcerative colitis (UC) is rare; however, both are chronic inflammatory diseases that share immunopathogenic mechanisms. In clinical practice, TNF (tumor necrosis factor) inhibitors are often among the first-line biologic agents; nonetheless, treatment responses in both diseases can be heterogeneous, and some patients develop primary non-response or secondary loss of response.We report a case of refractory UC with coexisting TAK that was unresponsive to two different anti-TNF therapies, in whom treatment with the JAK1 (Janus kinase 1) inhibitor upadacitinib was associated with both clinical improvement and favorable follow-up vascular imaging findings. By month 3 of upadacitinib therapy, marked improvement was observed in clinical symptoms and inflammatory markers; by month 15, follow-up CT angiography demonstrated decreased mural thickness at the common carotid artery (2.73 mm to 1.10 mm), thoracic aorta (1.92 mm to 1.24 mm), and abdominal aorta (2.34 mm to 1.58 mm), and surveillance colonoscopy confirmed endoscopic remission. No adverse events were observed during treatment. These findings suggest that upadacitinib may have contributed to concurrent improvement in mucosal disease activity and vascular imaging findings in a patient with concomitant TAK and UC. We also performed a targeted case-based literature review of JAK inhibitors in UC/IBD-TAK overlap and summarized published cases.
Avcu A, Koker O, Kani HT, Akkelle BS, Arik E, Direskeneli H, Alibaz-Oner F
GENERATIVE AI TOWARDS A COMPARATIVE ANALYSIS OF HOSPITALIZATION RATES AMONG PATIENTS WITH ULCERATIVE COLITIS TREATED WITH INFLIXIMAB, VEDOLIZUMAB, AND TOFACITINIB IN THE PUBLIC HEALTHCARE SYSTEM IN BRAZIL: A NATIONWIDE STUDY.Observational study Arquivos de gastroenterologia | 2026-05-22
Ulcerative colitis (UC) is a chronic inflammatory bowel disease that requires advanced therapies, including infliximab, vedolizumab, and tofacitinib. Our aim is to understand the hospitalization rates and outcomes associated with these therapies in real-world scenarios, which is crucial for optimizing patient management and healthcare resource allocation. This nationwide retrospective observational study analyzed real-world data (RWD) from Brazil’s public healthcare system (SUS) between January 2021 and December 2023. Data on hospitalizations, length of stay, mortality, costs, and non-IBD-related hospital admissions were extracted and analyzed using the Techtrials TT Disease Explorer and TT RWE Generator, leveraging generative artificial intelligence (GenAI) for data integration and analysis. A total of 1,313 patients required hospitalization, with 1,434 hospitalizations recorded. The hospitalization rate per 100 patients was highest for tofacitinib (262.5), followed by infliximab (212.88) and vedolizumab (191.67). Patients treated with infliximab had the shortest hospital stay (Median 3.0 days [0-68]) and lowest costs (Median 510.83 BRL [23.45 - 111,594.14]), whilst vedolizumab had the highest hospitalization costs. Surgical intervention rates were highest among tofacitinib users. Non-IBD-related hospitalizations suggested potential adverse drug events, including gastrointestinal disorders, infections, and anemia. This study represents the first AI-assisted RWE analysis of UC hospitalizations in Brazil. The findings highlight the varying hospitalization burdens across advanced therapies, with tofacitinib associated with higher hospitalization rates and infliximab linked to shorter hospital stays and lower costs. These insights can inform clinical decision-making and healthcare policy. Future studies should further explore AI’s role in optimizing RWE research and UC management. A retocolite ulcerativa (RCU) é uma doença inflamatória intestinal crônica que requer terapias avançadas, incluindo infliximabe, vedolizumabe e tofacitinibe. Nosso objetivo é compreender as taxas de hospitalização e os desfechos associados a essas terapias em cenários de mundo real, o que é fundamental para otimizar o manejo dos pacientes e a alocação de recursos em saúde. Este estudo observacional retrospectivo de âmbito nacional analisou dados de mundo real (RWD) do sistema único de saúde (SUS) do Brasil entre janeiro de 2021 e dezembro de 2023. Dados sobre hospitalizações, tempo de internação, mortalidade, custos e admissões hospitalares não relacionadas à DII foram extraídos e analisados utilizando o Techtrials TT Disease Explorer e o TT RWE Generator, com o uso de inteligência artificial generativa (GenAI) para integração e análise dos dados. Um total de 1.313 pacientes necessitou de hospitalização, com 1.434 internações registradas. A taxa de hospitalização por 100 pacientes foi mais alta para tofacitinibe (262,5), seguida por infliximabe (212,88) e vedolizumabe (191,67). Pacientes tratados com infliximabe apresentaram o menor tempo de internação (mediana de 3,0 dias [0-68]) e os menores custos (mediana de R$ 510,83 [23,45 - 111.594,14]), enquanto o vedolizumabe apresentou os maiores custos de hospitalização. As taxas de intervenção cirúrgica foram mais elevadas entre os usuários de tofacitinibe. As hospitalizações não relacionadas à DII sugeriram potenciais eventos adversos aos medicamentos, incluindo distúrbios gastrointestinais, infecções e anemia. Este estudo representa a primeira análise de RWD sobre hospitalizações por RCU no Brasil com o auxílio de IA. Os resultados destacam diferentes impactos das terapias avançadas nas hospitalizações, com tofacitinibe associado a maiores taxas de hospitalização e infliximabe ligado a menores tempos de internação e custos. Essas informações podem subsidiar tomadas de decisão clínica e políticas de saúde. Estudos futuros devem explorar mais profundamente o papel da IA na otimização da pesquisa em RWD e no manejo da RCU.
Valverde DA, Quaresma AB, Villamil MPG, Moraes TP, Kotze PG
Prevalence, patient characteristics, and outcomes of high-dose upadacitinib in inflammatory bowel disease. Therapeutic advances in gastroenterology | 2026-05-21
Off-label high-dose upadacitinib (UPA) may be necessary for select inflammatory bowel disease (IBD) patients. To evaluate the rates, patient characteristics, and outcomes of extended induction and high-dose UPA maintenance in IBD. We conducted a two-center, retrospective cohort study of IBD patients treated with UPA from January 1, 2022, to March 1, 2025. Extended induction was defined as receiving UPA 45 mg for 16 weeks in ulcerative colitis (UC) and 24 weeks in Crohn’s disease (CD). High-dose maintenance was defined as continuing UPA 45 mg after induction/extended induction. Primary outcomes included rates and characteristics of high-dose maintenance. Secondary outcomes included clinical response (CR), steroid-free clinical remission (SFCR), endoscopic remission (ER), and adverse events, comparing standard and high-dose UPA groups. Among 128 patients (46.9% CD, 48.4% UC, 4.7% IBD-unclassified), 51.6% (n = 66) received extended induction and 34.4% (n = 44) continued high-dose UPA maintenance. On multivariate analysis, UPA high-dose maintenance patients were more likely to have a higher number of prior biologic exposures (odds ratio (OR) 1.84, 95% confidence interval (CI) 1.05-3.19, p = 0.022) and concomitant biologic use (OR 6.18, 95% CI 1.15-33.18, p = 0.034). In the high-dose maintenance group, rates of CR were 73.7%, SFCR 65.8%, and ER 36.7%. Adverse event rates were similar between high- and standard-dose maintenance groups (25% vs 26.8%), with no cases of herpes zoster, venous thromboembolism, or major adverse cardiovascular events. One-third of patients remained on high-dose UPA maintenance, reflecting more refractory disease and modest response rates. Treatment was generally well tolerated. Larger, long-term studies are needed to validate safety. Using higher doses of upadacitinib in people with inflammatory bowel disease: What we found. This study looked at how often people with inflammatory bowel disease (IBD) are treated with higher-than-standard doses of a medicine called upadacitinib, and how well this approach works. The researchers wanted to understand who needs higher doses, how patients respond, and whether this treatment appears safe. IBD includes Crohn’s disease and ulcerative colitis. These conditions cause long-term inflammation in the gut and can be difficult to control. Some patients do not improve with standard treatments and need off-label therapy. Upadacitinib is a medicine used for IBD, but some patients need higher doses than usual to control their symptoms. It is important to know if this approach helps and whether it causes more side effects. Researchers reviewed medical records from two hospitals. They studied 128 adults with IBD who were treated with upadacitinib between 2022 and 2025. They looked at how many patients received higher doses for a longer period and how many stayed on a high dose for long-term treatment. They compared symptom improvement, healing of the bowel as seen on colonoscopy, and side effects between standard-dose and high-dose upadacitinib treatment. About 1 in 3 patients stayed on high-dose upadacitinib treatment long term. These patients usually had more severe disease and had tried many other treatments before. In the high-dose group, about 7 out of 10 people improved, about 2 out of 3 reached remission without steroids, and about 1 out of 3 showed bowel healing. Side effects were similar in people on standard and high doses, and no serious safety events were seen.
Azar J, Johnkennedy R, Levine LJ, AlOmar I, AlMutairdi A, Attamimi M, Proctor DD, Gaidos JKJ, Al-Bawardy B
Advances in Drug Delivery Systems for Boswellic Acids from Boswellia serrata: Enhancing Oral Bioavailability and Therapeutic Efficacy.Review International journal of molecular sciences | 2026-05-15
Boswellic acids (BAs), the major bioactive constituents of Boswellia serrata oleo-gum resin, exhibit well-documented anti-inflammatory and antioxidant activities, which correspond to their healing effects in arthritis, inflammatory bowel disease, asthma, metabolic syndrome, liver disorders, and certain cancers. However, their therapeutic potential is hindered by their poor aqueous solubility, low intestinal absorption, extensive metabolism, and overall low oral bioavailability. This review provides a comprehensive analysis of conventional Boswellia serrata products and advanced drug delivery systems designed to enhance the biological performance of BAs. We summarize recent developments in formulation strategies, including phytosomes, micelles, self-emulsifying drug delivery systems, solid lipid particles, polymeric nanoparticles, hydrogels, cyclodextrin complexes, metal-based nanocarriers, and hybrid delivery platforms. Available in vivo and cellular studies are critically evaluated, with a focus on disease-specific outcomes. Results indicate that emerging formulation technologies significantly increase the oral absorption, systemic exposure, and biological effectiveness of BAs. However, despite promising preclinical data, challenges remain regarding the standardization of Boswellia extracts, the stability of novel formulations, their safety, and limited clinical evaluation. By comparing the advantages and limitations of conventional preparations with modern drug delivery systems, this review outlines the most effective strategies to enhance the bioavailability of BAs and highlights future research directions for their translational development.
Rutkowska M, Olszewska MA
Herpes Zoster in Patients Treated with JAK Inhibitors for Immune-Mediated Inflammatory Diseases: Incidence, Associated Factors and Vaccination Uptake in a Real-World Cohort. Journal of clinical medicine | 2026-05-13
Background/Objectives: This study aimed to determine the incidence of herpes zoster (HZ) and risk factors associated with its occurrence in patients receiving Janus kinase inhibitors (JAKis) for immune-mediated inflammatory diseases (IMIDs), while evaluating preventive strategies and zoster vaccine uptake. Methods: We conducted a retrospective single-center cohort study including patients with rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, inflammatory bowel disease, atopic dermatitis and alopecia areata treated with upadacitinib, baricitinib or tofacitinib. The primary outcome was incident HZ during JAKi exposure. Incidence rates (IRs) were calculated per 100 person-years (PY) and Cox regression identified factors associated with HZ. Results: A total of 292 patients contributed 565.5 PY of JAKi exposure. During follow-up, 23 patients (7.9%) developed HZ, corresponding to an overall IR of 4.07/100 PY (95% CI 2.40-5.73). Incidence rates were numerically lower with upadacitinib and varied across disease groups; differences were not statistically significant. Diabetes mellitus (HR 3.05, 95% CI 1.28-7.29) and chronic kidney disease (HR 3.24, 95% CI 1.17-8.95) were independently associated with HZ. Herpes simplex infection requiring systemic antiviral therapy was more frequent among patients who developed HZ. Recombinant zoster vaccine (RZV) uptake was low (9.9%), but higher among patients evaluated in a dedicated infectious risk consultation. No HZ events were observed among RZV-vaccinated patients. Although six HZ events (26.1%) were severe, all cases resolved completely. Conclusions: HZ remains a relevant complication of JAKi therapy across IMIDs. Diabetes mellitus and chronic kidney disease may help identify higher-risk patients, while structured infectious risk assessment could improve vaccine uptake.
Parchão A, Monteiro C, Araújo-Andrade L, Dias CC, Abreu C
Biomarkers & Precision Medicine (14 papers)
Impact of non-surgical periodontal therapy on biomarker levels in inflammatory bowel disease patients with periodontitis. Journal of periodontology | 2026-05-30
This study investigated the effects of non-surgical periodontal therapy (NSPT) on saliva and serum levels of T cell immunoglobulin and mucin domain-containing protein 3 (TIM-3), tumor necrosis factor (TNF)-α, interleukin (IL)-6, IL-17, and serum levels of C-reactive protein (CRP) in patients with inflammatory bowel disease (IBD) and/or periodontitis. The study included 72 participants, 18 in each of the four groups: systemically and periodontally healthy (HH), systemically healthy with periodontitis (HP), IBD and periodontally healthy (IBH) and IBD with periodontitis (IBP). Clinical periodontal parameters and biomarker levels were evaluated at baseline in all groups and 3 months after NSPT in the periodontitis groups. Biomarker levels were analyzed using ELISA. At baseline, salivary IL-6 and IL-17 levels were significantly elevated in the IBH and IBP groups compared with those in the HH group (all p < 0.05). NSPT led to significant improvements in periodontal clinical parameters. Following NSPT, significant reductions in salivary IL-6, IL-17, TIM-3, and the serum CRP levels were observed in the IBP group (all p < 0.05). No significant changes in serum IL-6, IL-17, TNF-α, or TIM-3 levels were detected (all p > 0.05). Salivary IL-6 levels showed strong diagnostic potential for distinguishing IBP from HH (AUC = 0.932) and HP from IBP (AUC = 0.889). NSPT may contribute to the modulation of local and systemic inflammation in patients with IBD and periodontitis. Salivary TIM-3 emerged as a potential novel biomarker for periodontal disease detection in this population. This study has been registered in the ClinicalTrials.gov protocol registration system (Identifier: NCT06245278). Periodontitis and inflammatory bowel disease (IBD) are common diseases that are related to each other and have a high risk of occurring together. Dysbiosis and chronic immune activation are common features of both diseases. Cytokines such as interleukin (IL)-6, IL-17, and tumor necrosis factor-alpha (TNF-α), as well as inflammatory markers such as C-reactive protein (CRP), are involved in the inflammatory cascades of both diseases. Although the role of T cell immunoglobulin and mucin domain-containing protein 3 (TIM-3) in the pathogenesis of periodontal disease and IBD is not clearly understood, it is thought to play a role in immunity and disease severity. This study included systemically healthy and periodontally healthy individuals (HH), systemically healthy individuals with periodontitis (HP), periodontally healthy individuals with IBD (IBH), and individuals with IBD and periodontitis (IBP). Serum and saliva samples were collected from all participants at baseline and additionally from individuals with periodontitis after non-surgical periodontal therapy (NSPT). Our findings showed significant improvements in clinical parameters following NSPT, particularly in IBD patients, along with concurrent decreases in saliva TIM-3, IL-6, IL-17, and serum CRP levels. In conclusion, periodontal inflammation may increase systemic immune activation in IBD, and periodontal treatment may offer potential benefits in reducing this burden.
Bulut H, Öğüt E, Nuriyev K, Beşışık F, Karaduman B
Identification and validation of fecal complement component 3 and fibronectin as potential biomarkers for monitoring disease activity in ulcerative colitis based on a mouse model. Animal models and experimental medicine | 2026-05-30
Ulcerative colitis (UC) is a typical inflammatory bowel disease requiring long-term management. Although fecal calprotectin (FC) is widely employed for assessing disease activity, it is still considered insufficient as a standalone tool. New biomarkers are needed to better predict risk and comprehensively reflect biological pathways. This study aimed to identify potential fecal biomarkers to monitor disease activity in UC. C57BL/6J mice were exposed to dextran sulfate sodium (DSS) treatment for 7 days. Feces were collected and subjected to proteomic analysis and enzyme-linked immunosorbent assay (ELISA). Mouse colon tissues were subjected to histopathological and immunofluorescence analyses. The correlations between the selected fecal proteins and disease severity were evaluated and compared with FC. Proteomic analysis revealed increases in fecal complement component 3 (C3) and fibronectin (FN) in the DSS group. Next, we measured fecal C3 and FN levels in mice using ELISA. Significant elevation in C3 and FN levels was observed as early as day 1 after DSS treatment, preceding the increase in FC. Both fecal C3 and FN demonstrated significant correlations with disease activity, with C3 exhibiting a stronger correlation than FC. Using immunofluorescence, we observed distinct C3 and FN expressions in both the colonic tissues and the intestinal lumen. These findings demonstrate that fecal C3 and FN are promising candidate biomarkers for monitoring UC disease activity, and their utility requires further validation in other colitis models and human cohorts.
Guo Y, Yan Z, Ye J, Yang R, Song Y, Yue H, Zhao Y
Serum proteomics in paediatric inflammatory bowel disease from a case-control study: biomarker discovery and ulcerative colitis-Crohn’s disease differentiation.★ EBioMedicine | 2026-05-29
The diagnosis of inflammatory bowel disease (IBD), ulcerative colitis (UC), and Crohn’s disease (CD), relies on clinical and pathological criteria. Non-invasive precision medicine tools to diagnose IBD and discriminate between UC and CD are needed to personalise management. Serum proteomics identified protein biomarkers capable of diagnosing IBD and differentiating CD from UC subtypes. We obtained serum samples from a retrospective study of 47 patients with IBD and non-IBD patients seen in a tertiary care paediatric gastroenterology clinic and applied SomaScan proteomics to measure 1305 proteins to discriminate between IBD and non-IBD and UC and CD. Four proteins were further validated by immunoassays in two retrospective cohorts of 295 and 105 individuals and multi-protein predictors were developed using Support Vector Machines (SVM). The SomaScan discovery phase identified 95 serum protein biomarkers (BH p < 0.01) that differentiated IBD from non-IBD and 70 proteins (p < 0.01) that distinguished UC from CD. Pathway analysis linked specific inflammatory processes and vascular functions to IBD and UC versus CD. An 8-protein classifier achieved an AUC of 0.95 for identifying IBD. Significant elevation of four key predictor proteins (MMP1, MMP3, Resistin, Haptoglobin) in IBD was validated by ELISA in the expanded cohort (N = 295). The 4-protein SVM predictor achieved an AUC of 0.86 and 0.90 for IBD discrimination in two independent cohorts. A separate 4-protein SVM predictor for differentiating UC from CD achieved an AUC of 0.93 in independent validation. Patients with paediatric-onset IBD have a unique serum protein signature associated with pro-inflammatory and vascular pathways. Additional studies are needed to determine whether these dysregulated proteins can be used in conjunction with traditional risk factors to support non-invasive biomarkers that identify IBD and discriminate between its subtypes. Martin Schlaff, The Diane and Dorothy Brooks Foundation, The Manessis Family, Thomas and Lynn Kuzma, and The Hasso Serrano Foundation.
Omede M, Otu HH, Grossberg LB, Huang JY, Gu X, Dillon ST, Can H, Morhardt TL, Pursley C, Winter HS
Integrative transcriptomic analysis unveils FXR as a key regulator of intestinal stemness and inflammation in ulcerative colitis. International journal of molecular medicine | 2026-05-29
High‑throughput transcriptomic technologies offer a systems‑level approach to unravel the mechanisms of complex immune disorders. Inflammatory Bowel Disease (IBD), a classic example of such disorders, involves intricate interactions between genetics, microbiota and immune dysfunction. The nuclear receptor farnesoid X receptor (FXR) is implicated in IBD, but its precise mechanisms remain unclear. To investigate the role of FXR in ulcerative colitis (UC), the present study employed an integrative transcriptomic strategy, combining bulk transcriptomics (GSE75214, GSE13367 and GSE87466) and single‑cell RNA‑sequencing data (GSE116222) of human UC samples obtained from the Gene Expression Omnibus database. Subsequently, these findings were validated in a dextran sulfate sodium‑induced colitis model using FXR global knockout mice. The results revealed that FXR expression is downregulated in UC and co‑localizes with the stem cell marker CD133 in intestinal crypts. FXR deficiency exacerbated dextran sulfate sodium‑induced colitis, impaired the expression of stemness‑associated transcription factors (octamer‑binding transcription factor 3/4, homeobox protein NANOG, transcription factor SOX2 and Sal‑like protein 4), and activated the NF‑κB pathway, leading to increased production of pro‑inflammatory cytokines, specifically TNF‑α and IL‑1β. By integrating bulk and single‑cell transcriptomics with genetic validation, the present study uncovered an FXR‑dependent mechanism linking intestinal stem cell dysfunction to NF‑κB‑driven inflammation in colitis, and established a generalizable multi‑layer transcriptomic dissection strategy for complex inflammatory disorders.
Lin H, Cheng X, Ren Y, Zhang Y, Chen W, Lu Q, Tian Y
Association between circulating metabolic biomarkers and the risk of inflammatory bowel disease: a prospective cohort study.Letter International journal of colorectal disease | 2026-05-27
Abstract not available.
Fan M, Wang M, Chen H, Lin S, Bai H, Han H, Chen L
Global research trends in ferroptosis in autoimmune diseases: a bibliometric and visual analysis (2018-2025). Autoimmunity | 2026-05-25
To systematically examine global research trends in the association between ferroptosis and autoimmune diseases from 2018 to 2025, thereby informing future mechanistic and translational investigations in this field. On March 17, 2026, relevant publications were obtained from the Web of Science Core Collection and PubMed databases. This included articles and reviews written in English and published between 2018 and 2025. Bibliometric visualization was conducted using CiteSpace 6.4.R1, VOSviewer 1.6.20, and Scimago Graphica to map countries, authors, institutions, keywords, journals, and references. Data processing and descriptive statistical analysis were performed using Microsoft Excel 2019. Seven hundred and nineteen publications from 27 countries were included in the analysis. The annual number of publications showed a consistent upward trend, with China contributing the largest share (487 publications). High-frequency keywords included rheumatoid arthritis, ulcerative colitis, inflammatory bowel disease, oxidative stress, and lipid peroxidation, indicating research hotspots in this field. Research on the association between ferroptosis and autoimmune diseases has expanded substantially over the past 8 years. However, the field remains in a relatively early stage of development. These findings suggest that the field is receiving increasing scholarly attention and may provide useful references for future biomarker discovery and novel therapeutic strategy development.
Li R, Song K, Chen Q, He Y, Yang S, Ren L, Jiang J, Wang L
Matrix metalloproteinases in intestinal fibrosis and fibrostenosing Crohn’s disease: Current evidence, mechanistic hypotheses, and translational challenges.★ Inflammatory bowel diseases | 2026-05-25
Fibrostenosing complications in Crohn’s disease arise from mixed transmural remodeling that includes inflammation, fibrosis, and muscular hypertrophy/hyperplasia. Matrix metalloproteinases (MMPs) are implicated in extracellular matrix turnover and inflammatory remodeling, but their precise role in stricture evolution remains incompletely defined. We review current evidence (2020-2026) on MMP biology in intestinal fibrosis and fibrostenosing disease, emphasizing assay limitations, tissue-layer heterogeneity, and the predominance of cross-sectional rather than longitudinal human data. This review examines current evidence on MMP classification and substrate specificities, current evidence on cytokine-MMP interactions and proposed spatial and contextual patterns of remodeling, MMP contributions to fibrosis and smooth muscle cell proliferation, assay caveats and interpretation guardrails that distinguish expression from activity across gut layers, candidate biomarkers (such as PRO-C3/-C6 and fecal or serum MMP-9, which remain investigational), and emerging but unproven therapeutic strategies highlighting clinical trials and optimization strategies. We propose a state- and layer-aware conceptual framework to organize these findings, while acknowledging that the proposed states likely overlap and have not been prospectively validated. Despite recent advances, clinical trials of anti-MMP agents such as andecaliximab have yielded limited efficacy, likely attributable to challenges in timing, drug specificity, and outcome assessment. Candidate biomarkers and emerging therapeutic strategies remain investigational, and no MMP-directed approach has yet demonstrated clinical utility for routine fibrosis staging or stricture prevention. Future research directions should prioritize longitudinal human studies, mechanistic elucidation of how MMPs influence fibrosis and/or smooth muscle hyperplasia, improved linkage between tissue biology and imaging, fibrosis-specific endpoints, and rigorous validation before clinical trial translation can be justified. This narrative review evaluates current evidence connecting matrix metalloproteinase (MMP) biology to intestinal fibrosis and fibrostenosing Crohn’s disease. It introduces a hypothesis-generating, state- and layer-aware framework to organize predominantly cross-sectional and preclinical findings. Key limitations of the evidence, such as the lack of longitudinal human validation, are also addressed.
Kochkarian T, Lopez KM, Ou R, Powell DW, Li Q
CBC-derived inflammatory indices predict adverse outcomes in geriatric emergency patients with acute infectious diarrhea: a MIMIC-IV analysis. Scientific reports | 2026-05-25
Acute infectious diarrhea remains a leading cause of morbidity and mortality worldwide. Similar to pediatric populations, geriatric patients represent a highly vulnerable group with increased hospitalization rates, prolonged length of stay, heightened dehydration susceptibility, diminished physiological reserve, and elevated mortality risk. While pediatric populations benefit from well-established clinical severity scores such as Vesikari and Clark scales, analogous prognostic tools specifically validated for geriatric patients with acute infectious diarrhea remain lacking. Specific inflammatory markers such as procalcitonin and C-reactive protein require additional testing and increase costs. Complete blood count (CBC)-derived inflammatory indices offer a practical alternative as they are inexpensive, universally available, and calculated from routine tests. This retrospective study utilized the MIMIC-IV database (2008-2019) to assess diagnostic accuracy of nine CBC-derived inflammatory indices (AISI, NPAR, HALP, NLR, SII, PLR, MLR, SIRI, PNI) for predicting adverse outcomes in geriatric patients (≥ 65 years) with acute infectious diarrhea. Patients were identified through two independent database queries using ICD-9 codes (008-009 infectious diarrhea, 003-005 bacterial/foodborne; n = 2,208 raw records) and ICD-10 codes (A02-A05 bacterial/foodborne, A08 viral enteritis, A09 infectious gastroenteritis unspecified; n = 1,868 raw records), which yielded overlapping results due to MIMIC-IV spanning both coding eras (2008-2012 ICD-9; 2012-2019 ICD-10); after cross-encounter deduplication retaining one index admission per patient, the non-redundant cohort comprised 3,934 patients. Exclusions (n = 1,087) comprised non-infectious gastroenteritis, inflammatory bowel disease, radiation enteritis, ischemic colitis, drug-induced diarrhea, immunosuppressed patients, missing laboratory data, and C. difficile recurrence. Among 2,847 immunocompetent geriatric patients, comorbidities included hypertension (32.8%), diabetes mellitus (18.6%), and chronic kidney disease (10.4%). Bacterial pathogens were identified in 276 (9.7%) and viral in 151 (5.3%; norovirus 64.1%, rotavirus 23.4%, adenovirus 12.5%). Hospital admission occurred in 668 (23.5%), ICU admission in 34 (1.2%), in-hospital mortality in 14 (0.5%), and AKI in 421 (14.8%). Thirty-day mortality, ascertained via Social Security Death Index linkage, occurred in 31 patients (1.1%). Bacterial infections demonstrated significantly elevated indices versus viral: AISI (9,845 vs. 920, more than tenfold higher), NLR (14.8 vs. 1.82, more than eightfold higher; all p < 0.001). For bacterial-viral differentiation, NLR achieved AUC 0.892. In bacterial infections (n = 276), AISI demonstrated highest accuracy for AKI (AUC 0.896), ICU (0.882), and mortality (0.868); NPAR showed comparable results (AKI 0.854, ICU 0.872, mortality 0.848). In viral infections (n = 151), indices showed moderate performance: AISI for AKI (AUC 0.782), ICU (0.768), mortality (0.754); NPAR for AKI (0.764), ICU (0.756), mortality (0.742). HALP achieved strong mortality prediction in both groups (bacterial 0.874, viral 0.768). In diabetic patients (n = 530), AISI achieved strong discriminatory performance (AUC 0.908 for AKI) with higher complications (AKI 26.8% vs. 12.1%; p < 0.001). CKD patients (n = 296) showed highest complications (AKI 38.6%, mortality 2.1%). Multivariable analysis confirmed AISI (aOR 1.052), NPAR (aOR 1.046), and HALP (aOR 0.91) as independent predictors (all p < 0.001). Among nine CBC-derived indices evaluated in geriatric patients with acute infectious diarrhea, AISI, NPAR, and HALP demonstrate superior diagnostic value for predicting AKI, ICU admission, and mortality, with higher accuracy in bacterial compared to viral infections. These cost-effective biomarkers may address the current gap in geriatric-specific prognostic tools; however, pathogen-stratified AUC values pertain exclusively to microbiologically confirmed cases and represent upper-bound estimates requiring prospective validation with multiplex PCR-based pathogen ascertainment.
Ucdal M, Yurtsever K, Ekingen E
Reference-guided genome assembly of long non-coding rna transcripts reveals target genes associated with Crohn’s disease. Scientific reports | 2026-05-25
Crohn’s disease (CD) is highly heterogeneous in presentation and progression with no cure. Molecular phenotyping has been used to elucidate cellular and tissue-based alterations to characterize drivers and effects of disease. One currently understudied class of functional molecules is long non-coding RNAs (lncRNAs). Studying the full lncRNA landscape in CD is challenging due in part to an incomplete lncRNA annotation and a lack of their functional characterization in tissues of interest. We used a genome-guided alignment strategy to assemble predicted lncRNA transcripts using short RNA-sequencing data from colon tissue of adult patient samples. When combining our predicted lncRNAs with previous lncRNA annotations, we determined 98 that were differentially expressed, recapitulating many from previous IBD studies while also uncovering new ones. We built gene co-expression networks to cluster lncRNAs with functionally characterized protein-coding genes. Clusters containing differential lncRNAs were correlated to disease status and associated with pathways related to the humoral immune response, metabolism, and tissue regeneration. We uncovered multiple differential lncRNAs whose expression significantly correlated with nearby differential protein-coding genes that have also been differentially expressed in other IBD datasets, such as PITX2. We focused on a predicted lncRNA that is antisense to the PITX2-adjacent lncRNA PANCR, which we called PANCR-AS1, and provide multiple lines of evidence that support PANCR-AS1 functioning as an enhancer of PITX2 expression. Overall, we determined lncRNAs that are potential contributors to CD pathogenesis. We developed a robust pipeline for identifying lncRNAs in diseased and non-diseased tissue that are absent from reference annotations. We also outlined a framework to pinpoint significant disease-associated lncRNAs with potential functional activity related to their nearby protein-coding genes.
Kennedy Ng MM, Silverstein S, Nishiyama NC, Beasley C, Lian G, Huan B, Lau G, Weaver D, Awad A, Schaner MR
Dolichocolon May Differentially Associate with Ulcerative Colitis Phenotype in Children. Digestive diseases and sciences | 2026-05-25
Dolichocolon (DC) is an underrecognized anatomic variant associated with constipation; its association with ulcerative colitis (UC) is unknown. We retrospectively reviewed abdominal MRI and CT scans in children with UC, Crohn’s disease (CD), and non-inflammatory bowel disease (non-IBD) controls, classifying DC subtypes. A total of 111 cases (66 with UC) were examined. DC was similarly common (p = 0.4436) in patients with constipated (69%) or non-constipated (NC-UC: 57%) UC. In non-constipated (NC) patients, DC prevalence was higher in children with UC than those with CD or controls. Type 1 DC predominated in NC children with proctitis/left-sided UC (E1/E2), while Type 2 DC was enriched in children with extensive/pancolitis (E3/E4). DC may be associated with different phenotypes of UC and may influence disease distribution independent of constipation. However, given the cross-sectional design of this study, these associations should be interpreted cautiously and require confirmation in longitudinal studies.
Kellermayer R, Berens DP, Szigeti RG
Detection of Calpain-Mediated Beclin-1 Cleavage for Drug Discovery in Inflammatory Bowel Diseases. Cells | 2026-05-18
Inflammatory bowel diseases (IBDs) are diseases of chronic inflammation and intestinal epithelial cell (IEC) death that affect an estimated 7 million people worldwide. Intestinal barrier restoration is the most important determinant of remission in IBD, yet there are very few existing therapies that protect IECs from damage or support epithelial repair. The goal of this study was to develop a model system and tools that can be used to identify therapeutics that promote IEC survival in IBD. We developed a Beclin-1 cleavage reporter (BICR) that detects calpain-mediated Beclin-1 cleavage and the switch from autophagy to programmed cell death. We modified BICR with the HIV Tat peptide (BICR-Tat) and tested it in a model of live bacterial stress using commensal E. coli and IEC. BICR sensitively and specifically detected calpain activity in cell-free assays, and BICR-Tat successfully detected Beclin-1 cleavage and autophagy failure in IEC. Achieving IEC survival in the microbe-challenged IBD gut would be an important advance toward intestinal barrier restoration in this intractable disease. The BICR-Tat reporter coupled with the model of microbial stress developed in this study could enable high-throughput screening approaches to identify therapeutics with the potential to achieve barrier healing and sustained remission in IBD.
Hunter KA, Overstreet AC, Koff BB, Dharan H, Overend S, Messer JS
An Exponential Scale Mixture Model for Metatranscriptomics Data with Application to Inflammatory Bowel Disease. bioRxiv : the preprint server for biology | 2026-05-15
Metatranscriptomic (MTX) sequencing enables profiling of gene expression across microbial communities, providing a framework for linking genetic potential with functional activity. However, standard pipelines report normalized abundances rather than raw counts, limiting the use of count-based RNA-seq methods, while Gaussian-based alternatives rely on transformations and assumptions that are often poorly suited to MTX data. We propose a new modeling framework for differential expression analysis of MTX data, built on a scale mixture of exponential distributions, that incorporates DNA abundance to adjust for genomic potential, accommodates subject-specific random effects, treats zeros as left-censored, and employs a mixture prior to handle extreme sparsity. Applied to the IBDMDB multi-omics cohort, differential expression results vary substantially across models, including among Gaussian approaches with different pseudocount choices. Our approach identifies a distinct subset of candidate genes not detected by existing Gaussian methods; these may provide useful leads toward a novel understanding of transcriptomic patterns associated with dysbiosis in inflammatory bowel disease. Estimated dysbiosis effect directions are consistent between our model and Gaussian-based approaches, while effect sizes from our model tend to be larger in absolute value.
Kim H, Ma L
Integrated metabolomics and gut microbiota analyses reveal the protective effects of matrine in ulcerative colitis. Frontiers in chemistry | 2026-05-13
Ulcerative colitis (UC) is a chronic inflammatory bowel disease driven by gut microbial dysbiosis and metabolic dysfunction. Matrine, a natural alkaloid with anti-inflammatory properties, shows therapeutic potential; however, its mechanisms involving the coordinated modulation of bacteria, fungi, and host intestinal luminal metabolism remain unclear. We evaluated the therapeutic efficacy of matrine using a dextran sulfate sodium (DSS)-induced murine model of ulcerative colitis. Disease severity was assessed via the disease activity index, colon length, and histopathology. Integrated multi-omics approaches, including metagenomics, ITS fungal sequencing, and untargeted metabolomics of intestinal luminal contents, were employed to systematically characterize the regulatory effects of matrine on gut bacteria, fungi, and metabolic profiles. Here, we demonstrated that oral matrine significantly alleviated disease severity in a DSS-induced UC mouse model, as evidenced by improved disease activity index, colon length, histopathology, and restoration of tight junction proteins. Integrated multiomics revealed that matrine restored bacterial homeostasis-suppressing Escherichia while enriching SCFAs-producing taxa (Muribaculum, Paramuribaculum, Clostridium). Metagenomic predictions revealed that matrine treatment reversed the model-induced suppression of carbohydrate metabolism and bile acid biosynthesis while upregulating depleted CAZy enzyme families, thereby correcting dysregulated metabolic functions in colitis. Furthermore, matrine rebalanced the mycobiota by normalizing the Ascomycota/Basidiomycota ratio. Intestinal luminal contents untargeted metabolomics identified 43 matrine-responsive metabolites, implicating correction of bile acid metabolism, attenuation of leukotriene-mediated inflammation, and reversal of acylcarnitine-driven epithelial energy disruption. Critically, pro-inflammatory metabolites correlated positively with Escherichia and negatively with beneficial symbionts. Our findings established that matrine exerted protective effects in UC through a unified “microbiota-metabolism” axis, highlighting its promise as a multi-target therapeutic agent for UC.
Su L, Zhang Y, Xie Y, Wu J, Yang Y, Li Y, Huang Y, Liu X, Wei X, Chen Q
A preclinical investigation into the potential associations of geraniin with ulcerative colitis alleviation through integrated multi-omics and in vivo analysis. Frontiers in medicine | 2026-05-13
This study aims to investigate the potential molecular mechanisms and alleviating effects of geraniin, a natural polyphenol compound, within a murine model of ulcerative colitis (UC), thereby providing preclinical insights that may inform future translational strategies. Potential targets of geraniin for UC were identified by screening databases such as the Comparative Toxicogenomics Database and SwissTargetPrediction. UC transcriptomic and single-cell data were sourced from GEO (GSE47908, GSE214695). Differential gene analysis used limma, co-expression modules via WGCNA, enrichment with ClusterProfiler for GO/KEGG, and immune cells via CIBERSORT. Single-cell analysis employed Seurat and AUCell to identify targeted subpopulations. In vivo, DSS-induced UC mice were grouped as control, model, and model + geraniin (30, 60 mg/kg). Effects were assessed by DAI, histopathology, Western blot, and immunofluorescence. Geraniin targeted 27 genes, which were integrated with 337 UC-related genes to construct a protein-protein interaction network. MCODE analysis identified a key subnetwork comprising 42 genes. GO and KEGG analyses suggested that the potential effects of geraniin may be linked to inflammatory pathways such as IL-17, TNF, and CXCR chemokine signaling. In the single-cell dataset GSE214695, AUCell scores indicated an enrichment of drug targets in macrophage and neutrophil clusters. In this murine model, in vivo experiments indicated that geraniin administration was associated with reduced DAI scores, improved colon length, and the alleviation of mucosal damage and inflammatory cell infiltration. Immunofluorescence analysis revealed that geraniin treatment was associated with a reduced presence of markers for M1 macrophages (F4/80+/CD86+), neutrophils, and NET formation (CitH3+/MPO+), while correlating with an increase in M2 macrophages markers (F4/80+/CD206+). Western blot analysis showed that geraniin treatment correlated with the downregulation of NOS2 and upregulation of PPARG expression, which may contribute to mitigating the inflammatory response observed in this model. These findings suggest that geraniin is associated with the alleviation of DSS-induced UC in mice, potentially through the modulation of phenotypic markers related to macrophages and neutrophils.
Cheng C, Wang W, Zheng T, Shi X, Fu C
Quality of Life & PROs (14 papers)
Metabolic host-microbe crosstalk in stabilization of epithelial HIF. Microbiome | 2026-05-30
The gastrointestinal tract is home to trillions of microorganisms that interact with their host in profound ways. One mechanism by which these microbes interact with their eukaryotic host is through the establishment of “physiologic hypoxia” in the intestinal mucosa, which has been shown to promote gut barrier function and homeostasis in a hypoxia-inducible factor (HIF)-dependent manner. The association between HIF and intestinal homeostasis has been long understood, as activation of HIF signaling has been shown to promote barrier function both in vitro and in vivo. Although it has been previously established that pathogenic bacteria regulate HIF stabilization and activity in the intestinal epithelium independent of short-chain fatty acid metabolism, it is not clear whether this activity extends to noninfectious and/or commensal bacterial species. Here, we demonstrate that nonpathogenic, commensal strains of Escherichia coli stabilize HIF in intestinal epithelial cells in vitro. Further, we show that HIF is transcriptionally active in epithelia and drives a “pro-barrier” transcriptional program. This property was found to be dependent on bacterial aerobic respiration, as genetic elimination of E. coli aerobic respiration abolished HIF stabilization and the subsequent transcriptional phenotype. Finally, we observed stabilization of tissue HIF-1α in vivo using antibiotic-treated mice colonized with wild-type, but not respiration-deficient, E. coli. These findings demonstrate a novel ability for commensal E. coli to regulate intestinal homeostasis through activation of HIF and suggest that this mechanism might be a major component of the interaction between facultative anaerobes and the intestinal epithelium in the gut. In addition, we hypothesize that consumption of oxygen by enteric bacteria might be leveraged as a novel therapeutic to combat intestinal inflammation, such as that observed during inflammatory bowel disease (IBD). Video Abstract.
Dowdell AS, Roer RL, Bhagavatula G, Cartwright IM, Cohen RH, Countess JA, Koch SD, Lee JS, Liu L, Steiner CA
Patient-reported Outcomes in Clinical Trials of Inflammatory Bowel Disease: A Systematic Review and Meta-analysis.Review★ Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association | 2026-05-28
Patient-reported outcomes (PROs) and outcome measures (PROMs) have increasing prominence in clinical trials for inflammatory bowel disease (IBD). This systematic review provides an overview of PROMs used in randomized controlled trial (RCTs), their placebo outcome rates, effect sizes, and operating properties. We first searched MEDLINE, Embase and Cochrane CENTRAL up to March 31, 2025 for RCTs in IBD using PROMs. In a subsequent search, we searched the databases for studies, regardless of design, reporting on the operating properties of PROMs. In the first part, we summarized the PROMs and outcome definitions. We calculated pooled placebo outcome rates and pooled risk ratios using the DerSimonian-Laird random-effects model. In the second part, we summarized the validity of PROMs. A total of 132 (71 in Crohn’s disease, 61 in ulcerative colitis) RCTs reported 29 PROMs, most commonly the IBD Questionnaire (IBDQ), PRO-2, the Euro QoL survey, and the 36-item Short Form survey. Outcome definitions and reporting formats were highly heterogeneous. Pooled placebo outcome rates for different PROMs were 25.2-43.6%. Although superiority over placebo was demonstrated using different PROM-based outcomes, effect sizes were smaller compared to the primary endpoint for the same trials. A total of 171 studies evaluated the operating properties of 78 PROMs. A minority of instruments underwent extensive validation. These included IBD Control, IBD Disability Index, and IBDQ. There is substantial heterogeneity in PROM reporting in RCTs. Placebo rates were high and effect sizes low for PROMs. Only a minority of PROMs were extensively validated; of the latter, none were developed following regulatory recommendations.
Hanzel J, Yuan Y, Goodwin SW, Nardone OM, Roseira J, Solitano V, Vuyyuru SK, Leong RW, Sands BE, Turner D
Impact of depression and anxiety on health-related quality of life changes over time within individuals with rheumatoid arthritis or inflammatory bowel disease: A prospective Canadian cohort study. PloS one | 2026-05-28
In individuals with rheumatoid arthritis (RA), inflammatory bowel disease (IBD), or primary depressive or anxiety disorders without RA or IBD (DEP/ANX) we aimed to evaluate between-person and within-person changes in physical and mental health-related quality of life (HRQoL) over time. We also aimed to compare the impacts of depression and anxiety symptoms on HRQoL, and to examine the roles of physical and cognitive functioning, fatigue, physical comorbidities, and disease activity, on HRQoL over time. As part of a single centre prospective cohort study, individuals with RA (n = 154), IBD (n = 247), or DEP/ANX (n = 306) recruited between November 2014 and July 2016 were seen annually for 3 years. Participants reported symptoms of depression and anxiety (Hospital Anxiety and Depression Scale), fatigue (Daily Fatigue Impact Scale), HRQoL (RAND-36), and completed functional assessments (physical: nine-hole peg test, timed 25-foot walk test; cognition: Symbol Digit Modalities Test). Generalized linear models with generalized estimating equations tested between-person and within-person associations of depression and anxiety with HRQoL in covariate-adjusted models that included socio-demographic characteristics, health status and medication use. Physical (PCS-36) and mental (MCS-36) HRQoL were assessed separately and comparatively for RA, IBD and DEP/ANX. RA participants were older than IBD or DEP/ANX participants [mean age = 59.49(11.66), 47.45(14.80), 43.87(12.94)]. Most participants (>85%) reported meaningful changes in HRQoL. After adjustment, within-person increased depressive and anxiety symptoms were associated with reduced MCS-36 [depression: -7.91 (-9.45, -6.36), anxiety: -5.62 (-6.85, -4.39)]. Increased fatigue and worse cognition were associated with reduced PCS-36 [-0.33 (-0.38, -0.28); -0.31 (-0.64, 0.022)]. After adjustment, increased physical function, IBD or DEP/ANX diagnosis were associated with higher PCS-36 [1.47 (0.63, 2.30); 2.84 (1.60, 4.08); 5.23 (3.92, 6.55)]. Variations in depression, anxiety, fatigue, cognition, and physical function are associated with HRQoL fluctuations in people with RA, IBD and DEP/ANX, highlighting the importance of addressing these issues while treating disease.
Hitchon CA, Bernstein CN, Bolton JM, Dolovich C, El-Gabalawy R, Graff LA, Lix LM, Marriott JJ, Fisk JD, Marrie R
Prevalence of symptoms of anxiety and depression in postoperative patients with Crohn’s disease: a comparative cross-sectional study. BMC gastroenterology | 2026-05-26
Crohn’s disease is a chronic inflammatory condition often requiring surgical intervention, which can significantly impact a patient’s quality of life and mental health. This study aimed to evaluate the prevalence of anxiety and depressive symptoms in surgically treated patients with Crohn’s disease. A comparative cross-sectional study at a tertiary center included surgically and non-surgically treated patients with Crohn’s disease. Anxiety and depressive symptoms were assessed using the Generalized Anxiety Disorder-7 questionnaire and Patient Health Questionnaire-9. Disease activity was assessed using Harvey Bradshaw index and endoscopic recurrence was evaluated using the Rutgeerts score. A total of 97 patients with Crohn’s disease (54 surgical, 43 non-surgical controls) were included. The prevalence of anxiety and depressive symptoms were comparable between groups (57.4% surgical vs. 60.5% controls, p = 0.330) and (70.4% vs. 79.1%, p = 0.761), respectively. Surgical group had significantly better depression severity outcomes, with lower median Patient Health Questionnaire-9 scores (6.0 vs. 9.0, p = 0.007) and no cases of severe depression (0% vs. 14%, p = 0.025). Active disease was significantly associated with anxiety and depressive symptoms, whereas a lower body mass index was significantly associated with symptoms of depression. Previous surgery was not associated with lower prevalence of symptoms of anxiety or depression but was associated with significantly milder depression severity. The strong association of active disease and anxiety symptoms, and of active disease and lower body mass index with depressive symptoms, highlights the need for comprehensive care models that target both physical and psychological symptoms.
Abu Sneineh A, Haj Ali S, Mazzawi T, Mohtaseb MS, Ali R, Abu Farsakh N, Senan F, Hodali S, Agraib L, Khatib O
Eubacterium rectale Mitigates Inflammatory Bowel Disease via Modulation of Glutamine Metabolism Through the GLS2 and NF-κB Pathway. NPJ science of food | 2026-05-26
Inflammatory Bowel Disease (IBD) is a chronic inflammatory intestinal disorder with complex etiology, closely associated with gut microbiota dysbiosis. This study demonstrates that Eubacterium rectale (ER), a beneficial commensal bacterium, alleviates dextran sulfate sodium (DSS)-induced colitis in mice, as evidenced by improved clinical symptoms, restored intestinal barrier integrity, and reduced pro-inflammatory cytokine levels. Mechanistic investigations revealed that ER specifically upregulates the expression of glutaminase 2 (GLS2), ameliorates DSS-induced disturbances in glutamine (Gln) metabolism within intestinal epithelial cells, and subsequently inhibits the NF-κB signaling pathway to exert anti-inflammatory effects. Further validation showed that GLS2 deficiency abolishes the anti-inflammatory effects of ER. Collectively, this work identifies a therapeutically relevant mechanism: ER mitigates colitis via the GLS2/NF-κB axis. These insights pave the way for developing ER-derived live biotherapeutic products for IBD.
Han L, Jin Y, Lin W, Liu Z, Zeng C, Chen Y
An Exploration of Help-seeking Experiences of Patients With Inflammatory Bowel Disease From Healthcare Professionals: A Qualitative Descriptive Study. Gastroenterology nursing : the official journal of the Society of Gastroenterology Nurses and Associates | 2026-05-26
Inflammatory bowel disease (IBD) presents ongoing physical, psychological, and social challenges that can significantly affect quality of life. Despite this, little is known about how individuals with IBD seek help from healthcare professionals. This study used a qualitative descriptive design and latent pattern content analysis of semi-structured interviews (n = 8) to explore how individuals living with IBD seek help from healthcare professionals to manage challenges associated with their condition. The study adheres to the COREQ guidelines. Many participants delayed seeking help until symptoms interfered with daily activities, raised concern about severity, or others encouraged them to seek care. Reasons for delaying help-seeking included not seeing the symptoms as emergent, competing demands and priorities, or uncertainty about whether symptoms were IBD-related. Decisions around who to seek help from were shaped by prior experiences and perceived effectiveness of previous healthcare encounters. Physical symptoms often had a negative effect on participants’ psychological wellbeing. While some participants accessed online support, another emphasized the need for integrated psychological care within IBD services. Findings highlight that patients with IBD frequently navigate physical, psychological, and social challenges but predominantly seek help for physical symptoms. This study strengthens the need for routine inclusion of psychological support within specialist IBD care.
Byron C, Lehane E, Burton A, Cornally N
Two-dimensional GeTe nanosheets for psoriasis through modulation of macrophage activation and psoriatic inflammation. Biomaterials science | 2026-05-26
Psoriasis is a chronic inflammatory disease characterized by thickened erythematous skin lesions covered with white and silvery scales and accompanied by macrophage infiltration into the dermis. Although 2-3% of the world’s population suffers from psoriasis, there is still a requirement for novel, safe, and effective treatment options. Previously, our group demonstrated the theranostic effects of two-dimensional germanium telluride nanosheets (GeTe-NSs) in the treatment of inflammatory bowel disease. However, the precise mechanisms underlying their therapeutic action remained unclear. In this study, the specific anti-inflammatory mechanisms of GeTe-NSs in lipopolysaccharide-stimulated RAW 264.7 macrophages were evaluated, along with their therapeutic potential for psoriasis treatment in an imiquimod (IMQ)-induced murine model. GeTe-NS treatment significantly decreased cell proliferation and reduced the production of reactive nitrogen and oxygen species in activated RAW 264.7 macrophages. The GeTe-NSs lowered the mRNA levels of key pro-inflammatory mediators (Nos2, Tnf, Ccl2, and Cxcl15), while enhancing the mRNA levels of an anti-inflammatory factor (Arg1) and an antioxidant enzyme (Nqo1). Flow cytometric analysis revealed that the GeTe-NSs promoted a shift from the M1 (pro-inflammatory) macrophage phenotype toward the M2 (anti-inflammatory) phenotype. Western blot analysis demonstrated that anti-inflammatory effects were achieved by inhibiting the activation of the TLR4/CD14 and ERK/NF-kB/STAT1/STAT3 pathways. In vivo, the oral administration of GeTe-NSs in an IMQ-induced psoriasis mouse model resulted in significant improvements in clinical scores, epidermal thickening, and the proportions of M1/M2 macrophages in spleen and skin lesions. Taken together, these findings suggest that GeTe-NSs could be a promising nanomaterial for treating inflammatory diseases, including psoriasis.
Han J, Kim JW, Kang I, Lee SM, Park YB
The TECCU-based telemonitoring platform for Inflammatory Bowel Disease is Cost-Effective: A Multicenter GETECCU Trial.★ Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association | 2026-05-25
Evidence on the economic impact of telemonitoring in inflammatory bowel disease (IBD) is limited. We evaluated the cost-effectiveness and cost-utility of nationwide IBD telemonitoring compared with standard care. A multicenter, randomized, non-inferiority trial was performed in 24 Spanish centers including adults with IBD initiating immunosuppressants or biologics. Patients were assigned to telemonitoring using the TECCU app or standard care. The primary outcome for cost-effectiveness analysis was time in remission. Quality-adjusted life years (QALYs) were measured for the cost-utility. Healthcare and patient-incurred costs, including travel expenses, distance and time off work, were compared over 52 weeks. Of 159 randomized patients (75 TECCU, 84 control), 126 completed 52 weeks. At 12 and 52 weeks, TECCU saved €698.47 (95% CI -24,561 to 23,164) and €8.29 (95% CI -20.9 to 37.5) per additional week in remission. Overall, TECCU was less costly than standard care in 73.5% of simulations. Considering QALYs, TECCU saved €998 (95% CI: -4,257 to 2,261) and €1,441 (95% CI: -6,362 to 3,408) per additional QALY, with a 90.3% probability of cost-effectiveness at a willingness-to-pay threshold of €20,000. The mean number of contacts/patient was similar (6.9 vs 7.0; p=0.74), but TECCU reduced in-person visits (3.1 vs 4.8; p<0.001). Healthcare costs were lower with TECCU (€326 vs €361; p<0.001), and patients saved 52.27 ± 79.3 km travelled, 12.56 ± 8.2 hours off work and €12.63 ± 15.9 in travel expenses. Telemonitoring with the TECCU app reduces healthcare and societal costs while maintaining disease control, demonstrating its cost-effectiveness as a complementary strategy to standard care on a nationwide scale.
Aguas M, Del Hoyo J, Vicente R, Barreiro-de Acosta M, Melcarne L, Hernandez-Camba A, Madero L, Arroyo MT, Sicilia B, Chaparro M
Association between inflammatory bowel disease and anxiety and depressive symptoms in U.S. adults: a cross-sectional analysis of NHANES 2009-2010. Acta psychologica | 2026-05-25
This study aimed to examine the associations between inflammatory bowel disease (IBD) and self-reported anxiety and depressive symptoms using pre-pandemic, nationally representative data from the National Health and Nutrition Examination Survey (NHANES) 2009-2010. This cross-sectional study analyzed data from NHANES 2009-2010, the most recent cycle in which the PHQ-9, self-reported anxiety-days item, and self-reported physician-diagnosed IBD items were concurrently administered in the adult sample. Depressive symptoms were defined by a total score ≥ 10 on the Patient Health Questionnaire-9 (PHQ-9), while elevated anxiety symptoms were identified by self-reported feelings of worry, tension, or anxiety on ≥7 days within the past 30 days. Logistic regression models were used to analyze the association between IBD and anxiety and depressive symptoms, with exploratory subgroup analyses stratified by age and sex. The study included a total of 6398 participants, who were divided into two analytical groups based on mental health outcomes. The final sample for the anxiety symptoms analysis consisted of 4404 participants (1366 with elevated anxiety symptoms, 3038 without), while the depressive symptoms analysis included 4392 participants (464 with elevated depressive symptoms, 3928 without). Fifty-six individuals were identified as having IBD. After adjusting for covariates, IBD was significantly associated with both elevated anxiety symptoms (OR = 2.73, 95% CI: 1.55-4.80, P < 0.001) and elevated depressive symptoms (OR = 2.90, 95% CI: 1.48-5.28, P = 0.001). Exploratory subgroup analyses showed numerically larger point estimates among adults younger than 65 years and among women, but tests for interaction were not statistically significant (all p for interaction >0.05). In this cross-sectional U.S. sample, IBD was associated with higher odds of elevated anxiety and depressive symptoms. Apparent subgroup differences by age and sex were exploratory and should be regarded as hypothesis-generating rather than a basis for subgroup-specific clinical recommendations. Prospective studies are warranted to clarify temporal and causal relationships.
Mei X
Nanogel-coated nanozymes for ulcerative colitis targeted treatment by restoring redox homeostasis and anti-inflammatory activity. Colloids and surfaces. B, Biointerfaces | 2026-05-25
Excessive accumulation of reactive oxygen species (ROS) and overloaded immune system are key pathological features of ulcerative colitis (UC), but conventional treatments (such as aminosalicylates and immunosuppressants) often prove inadequate and have significant side effects. Here, an orally administrable PSGI utilized inulin (IN) as an outer shell and hollow mesoporous Prussian blue (HMPB) nanoparticles loaded with the aminosalicylate drug salazosulfapyridine (SASP) (PS) was developed to treat UC by scavenging ROS, reducing pro-inflammatory factors. After oral administration, IN can protect the drug-loaded nanoparticles from degradation by the enzymes of the upper gastrointestinal tract, easily penetrate into the lower gastrointestinal tract and reach the colon, where the IN shell could be degraded under the action of the colon-specific enzyme inulinase, to achieve the specific release of drugs that act like a “band-aid”, adhering the inflamed colon through a combination of enzymatic degradation and electrostatic adsorption, thereby prolonging drug retention at the site of inflammation, providing an improved synergistic therapy for UC. PSGI demonstrated a significant preventive effect in the mouse dextran sodium sulfate (DSS)-induced colitis model, with no obvious damage to major organs. This is because the ROS clearance effect of prussian blue (PB) itself enhances and complements the anti-inflammatory effect of SASP, thereby reducing the dosage of SASP and lowering the risk of potential side effects. Overall, PSGI has demonstrated good anti-inflammatory activity and biosafety in both in vivo and in vitro studies. We hope that this oral targeted nanoplatform for the treatment of UC can address key challenges such as targeted drug delivery, improved efficacy, and reduced side effects in the treatment of colitis.
Wang J, Wang Y, Zhu M, Ye R, Shen W, Wang Z, Wang Y, Lai X, Qiu X, Yu C
Protective effect of quercetin on ulcerative colitis via p38 MAPK-MK2/MK3 signalling pathway: mechanism of anti-inflammatory cellular action. Archives of physiology and biochemistry | 2026-05-24
Ulcerative colitis is a chronic inflammatory bowel disease characterised by disrupted anti-inflammatory cell mechanisms in the intestinal mucosa. This study explores quercetin’s protective role by restoring anti-inflammatory mechanisms and regulating this pathway. Experimental models included DSS-induced mice and LPS-stimulated RAW264.7 cells, assessed via disease activity scoring, histopathology, qPCR, ELISA, and Western blot. Quercetin intervention could effectively repair the anti-inflammatory cell function, reverse the imbalance of inflammatory factors, inhibit the phosphorylation of p38 MAPK and the expression of MK2 and MK3, improve the intestinal mucosal damage and disease activity in mice, and reverse the pro-inflammatory polarisation of macrophages in vitro. Quercetin could further enhance the anti-inflammatory effect when combined with p38 MAPK inhibitor. Therefore, quercetin can repair the anti-inflammatory cell action mechanism, inhibit the activation of p38 MAPK-MK2/MK3 signalling pathway, alleviate the inflammatory damage of intestinal mucosa in ulcerative colitis, and provide experimental basis for anti-inflammatory cell-targeted treatment of ulcerative colitis.
Zhang J, Wen Y, Zhang Q, Wang Y, Shen N, Guo M, Zhou Z, Zhang Q
Mental Health Disorders in Pediatric Inflammatory Bowel Disease: Epidemiology, Mechanisms, and Interventions.Review Journal of inflammation research | 2026-05-22
This review aims to synthesize current evidence on the association between pediatric inflammatory bowel disease (IBD) and mental health disorders, with a focus on epidemiology, underlying pathophysiological mechanisms, and advances in screening and intervention strategies. Pediatric IBD is increasingly recognized as a condition with substantial psychological as well as gastrointestinal burden. Children and adolescents with IBD have a markedly higher prevalence of mental health disorders than the general population, most commonly depression, anxiety, and sleep disorders, with risk appearing particularly higher in adolescents and in those with Crohn’s disease. Based on psychiatric evaluations, the prevalence of mental disorders in this population ranges from 42% to 73%. Accumulating evidence suggests a complex, bidirectional relationship between intestinal inflammation and mental health, mediated through interacting mechanisms that include gene-environment interactions, dysregulation of the gut-brain axis, immune imbalance, and medication-related effects. Although several validated screening tools for anxiety and depression have been introduced into clinical practice, mental health disorders in pediatric IBD remain frequently underrecognized and undertreated. Psychological interventions, family-centered care models, and pharmacologic treatments show potential benefit, but evidence in pediatric populations is limited and largely extrapolated from adult studies. Greater clinical awareness, routine mental health screening, and integrated multidisciplinary care interventions are essential to improve outcomes. Future large-scale, multi-center, and longitudinal studies are needed to clarify underlying mechanisms and optimize prevention and treatment strategies. Unlike previous reviews that often combine adult and pediatric populations, this review specifically focuses on pediatric-onset IBD and provides a dedicated synthesis of mental health comorbidities in children and adolescents.
Liu Y, Hu Y, Zheng J, Wu Z
Disulfide Cross-Linked Thiolated Chitosan/Oxidized Dextran-Oleylamine Micelle-Hydrogel System with pH/ROS Dual-Responsive Cascade Drug Release for Integrated Colon Targeting and Mucosal Repair in Inflammatory Bowel Disease. Pharmaceutics | 2026-05-14
Background: Oral colon-targeted delivery for inflammatory bowel disease (IBD) faces significant challenges, including limited gastrointestinal stability, premature drug release, and insufficient mucosal retention. Methods: To address these limitations, a mucoadhesive polysaccharide-based composite hydrogel incorporating prednisolone-loaded polymeric micelles was developed to enhance colonic delivery and promote mucosal repair. Amphiphilic oxidized dextran-oleylamine (ODEX-OA) copolymers were synthesized to self-assemble into prednisolone-loaded micelles. These micelles were subsequently embedded within a thiolated chitosan (CSSH) hydrogel through a Schiff base reaction, yielding the ODEX-OA-Pred-CSSH composite. The resulting system was comprehensively characterized for particle size, mucoadhesion, degradation, and pH/ROS dual-responsive drug release. Its colon-targeting capability and therapeutic efficacy were subsequently assessed in a dextran sulfate sodium (DSS)-induced colitis mouse model. Results: In vitro, the composite hydrogel demonstrated nanoscale micellar size, enhanced drug release kinetics under simulated inflammatory colonic conditions, and prolonged colonic retention for up to 24 h following oral administration. In vivo, studies confirmed that ODEX-OA-Pred-CSSH significantly alleviated colitis, evidenced by a reduced disease activity index, diminished pro-inflammatory cytokine levels, restored colon length, decreased spleen index, and improved histological mucosal repair. Conclusions: These findings collectively suggest that this mucoadhesive micelle-hydrogel composite represents a promising and effective oral colon-targeted platform for the treatment of IBD.
He J, Gan C, Chi T, Liu J, Bai T, Wu X, Liang G, Li R, Ma Y
Pregnane X receptor (NR1I2) deficiency in mice reveals context-dependent regulation of inflammatory homeostasis.Review Frontiers in immunology | 2026-05-12
Nuclear receptor subfamily 1 group I member 2 (NR1I2; mouse ortholog Nr1i2), also known as the pregnane X receptor (PXR) or steroid and xenobiotic receptor (SXR), is a ligand-activated transcription factor classically known for its role in xenobiotic metabolism and detoxification. Beyond these canonical functions, accumulating evidence identifies NR1I2 as a key regulator of inflammation and intestinal homeostasis, particularly in inflammatory bowel disease (IBD), where dysregulated inflammatory responses are central to disease pathogenesis and NR1I2 expression is often reduced. In this review, we integrate data from whole-body and tissue-specific Nr1i2-deficient mouse models, as well as knockdown and ligand-based approaches, to define the role of Nr1i2 in intestinal inflammation under basal and pathological conditions. These studies collectively show that whole-body Nr1i2 deficiency disrupts intestinal homeostasis, impairs barrier integrity, and enhances innate immune activation, whereas tissue-restricted deletion, especially within the epithelium, frequently fails to reproduce these phenotypes, underscoring the importance of coordinated Nr1i2 activity across multiple cellular compartments. Across experimental models, most often Nr1i2 deficiency commonly exacerbates intestinal injury, particularly in response to microbial toxins or chemical damage, however attenuated inflammatory responses have been reported in selected metabolic or injury contexts. Conversely, pharmacological activation of Nr1i2 confers protective and restorative effects in a ligand-, tissue-, and context-dependent manner. Together, these findings establish NR1I2 not as a simple anti-inflammatory switch, but as an immune-metabolic integrator that coordinates xenobiotic detoxification, microbial-derived signal sensing, and restraint of innate inflammatory pathways. This review provides a conceptual framework for future studies aimed at elucidating the cell- and context-specific functions of NR1I2 and for guiding the development of targeted therapeutic strategies for intestinal inflammatory disorders.
Amini SE
Surgery & Complications (14 papers)
Biologics and small molecules for perianal Crohn’s disease: a systematic review and meta-analyses of randomized placebo-controlled trials.★ Inflammatory bowel diseases | 2026-05-30
Although several advanced therapies (ATs) for luminal Crohn’s disease (CD) have been approved, their efficacy for perianal fistulizing Crohn’s (pCD) has not been comprehensively reviewed. A literature search was conducted in MEDLINE, Embase, and Cochrane CENTRAL up to October 2, 2025. Placebo-controlled randomized controlled trials (RCTs) evaluating treatment efficacy in pCD were included. Outcomes of interest were fistula response and fistula remission during the induction and maintenance trials. Pooled relative risks (RRs) were calculated using a random-effects model. Fourteen studies were eligible; only 4 RCTs were specifically designed for pCD, while the remainder were post hoc analyses of luminal CD studies with moderate to serious risk of bias. In pooled analyses of induction trials (4-28 weeks), ATs were associated with significantly higher induction of fistula response (RR 1.65, 95% CI 1.22-2.22) and remission (RR 1.91, 95% CI 1.37-2.67) compared to placebo. Infliximab and upadacitinib demonstrated significantly greater fistula response and remission, while ustekinumab significantly increased rates of fistula remission. For the maintenance phase (22-52 weeks), ATs were associated with significantly higher maintenance of fistula response (RR 1.54, 95% CI 1.21-1.97) and remission (RR 2.08, 95% CI 1.49-2.90) compared to placebo. Infliximab showed significantly greater maintenance of fistula response and remission compared with placebo, while adalimumab was superior for fistula remission. Findings from our meta-analysis indicate that infliximab is effective for pCD, with limited evidence of benefit with adalimumab, ustekinumab, and upadacitinib. Well-designed RCTs investigating newer advanced therapies are needed to better guide targeted treatment strategies for this patient population. This systematic review and meta-analysis summarizes the current evidence on the efficacy of advanced therapies for pCD, with most data derived from post hoc analyses and few dedicated studies. Infliximab appears effective, while evidence for adalimumab, ustekinumab, and upadacitinib remains limited, highlighting the need for well-designed RCTs.
Yuan Y, Jairath V, Hanzel J, Hupe M, Sedano R, Shehab M, Nardone OM, Magro F, Hart A, Vuyyuru SK
[Appendectomy as a disease-modifying therapy in ulcerative colitis?]. Zeitschrift fur Gastroenterologie | 2026-05-29
Ulcerative colitis is a chronic inflammatory systemic disease with rising incidence and increased mortality. Despite established therapeutic strategies, particularly maintenance therapy with mesalazine, approximately one third of patients experience a relapse within one year. Epidemiological studies demonstrate an inverse association between prior appendectomy and the risk of developing the disease, suggesting an immunological role of the appendix. Against this background, appendectomy has been investigated as a potential disease-modifying approach. The randomized ACCURE trial demonstrated a significant reduction in the one-year relapse rate with adjunctive appendectomy in the maintenance setting (36% vs. 56%; relative risk 0.65; NNT = 5), with a favorable safety profile. In patients with active disease under advanced therapy, the non-randomized COSTA study showed higher rates of steroid-free remission after appendectomy compared with switching to a JAK inhibitor, although no difference in colectomy rates was observed. In the PASSION study of therapy-refractory disease, 30% achieved a clinical response; histologically inflamed appendices were predictive of therapeutic success. In summary, randomized evidence currently exists only for the maintenance setting. Appendectomy appears to be a low-risk, potentially additive strategy for selected patients, but further controlled studies with long-term follow-up and biomarker stratification are required. Die Colitis ulcerosa ist eine chronisch-entzündliche Systemerkrankung mit steigender Inzidenz und hoher Morbidität. Trotz etablierter Therapiestrategien, insbesondere der Rezidivprophylaxe mit Mesalazin, erleiden innerhalb eines Jahres etwa ein Drittel der Patientinnen und Patienten ein Rezidiv. Epidemiologische Studien zeigen eine inverse Assoziation zwischen vorausgegangener Appendektomie und Erkrankungsrisiko, was auf eine immunologische Rolle des Appendix hinweist. Vor diesem Hintergrund wurde die Appendektomie als ein potenziell krankheitsmodifizierender Ansatz postuliert. Die randomisierte ACCURE-Studie belegt im Remissionserhalt eine signifikante Reduktion der Ein-Jahres-Rezidivrate durch zusätzliche Appendektomie (36% vs. 56%; relatives Risiko 0,65; NNT=5) bei günstiger Sicherheitsbilanz. Für aktive Erkrankungen unter fortgeschrittener Therapie zeigte die nicht-randomisierte COSTA-Studie höhere steroidfreie Remissionsraten nach Appendektomie im Vergleich zu einem Wechsel auf JAK-Inhibitoren, jedoch ohne Unterschied hinsichtlich Kolektomierate. In der PASSION-Studie bei therapierefraktären Verläufen erreichten 30% ein klinisches Ansprechen; ein histologisch entzündeter Appendix war prädiktiv für Therapieerfolg. Zusammenfassend existiert randomisierte Evidenz ausschließlich für das Remissionserhaltungs-Setting. Die Appendektomie erscheint als risikoarmer, potenziell additiver Ansatz für selektionierte Patientinnen und Patienten, bedarf jedoch weiterer kontrollierter Studien mit Langzeitbeobachtung und Biomarkerstratifizierung.
Stallmach A, Kolleck M
From preclinical phase of Crohn’s disease to postoperative recurrence: shared mechanisms and potential interventions.Review★ Gut | 2026-05-28
Crohn’s disease (CD) is a chronic inflammatory disorder of the gastrointestinal tract with high risk of surgery. Despite advances in medical treatment, of those patients who undergo ileocolonic resections, up to 70% of patients experience postoperative recurrence (POR) within 1 year of surgery. This underscores the need for a better understanding of the pathogenesis of POR. We hypothesise that the transient ‘disease-free’ state following surgical resection biologically mirrors the earliest preclinical stages of new-onset CD and that shared biomarkers across preclinical and postoperative settings reflect common pathogenic pathways. Identifying these shared signatures may offer a unique opportunity to elucidate mechanisms underlying both disease initiation and recurrence and to inform strategies aimed at prevention of new onset CD as well as POR. In this review, we synthesise insights from recent biomarker and multiomics studies spanning preclinical and postoperative CD cohorts. We highlight predictive biomarkers shared across CD onset and POR, including genetic variants, immune mediators such as CXCL9 and interleukin 6, microbial signatures involving Faecalibacterium and Ruminococcus and markers of gut barrier dysfunction and systemic inflammation. We also discuss emerging omics approaches including glycomics, urine metabolomics and high-dimensional immunophenotyping that may further refine risk stratification, capture pathogenic heterogeneity and provide mechanistic insight into host-microbe-immune interactions. Finally, we outline potential intervention strategies targeting these shared pathways and propose that the postoperative setting could be a pragmatic human model to test biomarker-guided preventive approaches applicable across the CD spectrum.
Chen R, Turpin W, Allez M, Silverberg MS, Croitoru K, Lee SH
Turnbull procedure-analysis of a cohort in the salvage setting. International journal of colorectal disease | 2026-05-28
The Turnbull procedure (coloanal pull-through with delayed coloanal anastomosis, DCAA) serves as a salvage option for complex, therapy-refractory pelvic floor disorders to avoid permanent colostomy. This study evaluated the perioperative outcomes, stoma avoidance, and functional results of 16 patients treated between 2018 and 2024. A retrospective analysis of 16 consecutive patients with hostile pelvis (e.g., post-surgical fistulas, chronic pelvic sepsis, and Crohn’s disease). The key outcomes were time to anastomosis, Clavien-Dindo complications, stoma reversal rate, SF-12 quality of life, LARS, and Wexner continence score. Follow-up = 19-80 months. Anastomosis occurred after a mean of 11 days (range, 6-19 days). Permanent stoma was avoided in 13/16 (81%) patients. Perioperative morbidity was low, and the SF-12 scores (14/16) ranged from 29 to 86%, correlating with the LARS (p = 0.016). In 12 patients, minor LARS was observed in 3/12, major LARS in 7/12, the Wexner incontinence score showed good continence in 4/12, moderate incontinence in 5/12, and severe incontinence in 3/12. The fistula subgroup showed the best functional results. The Turnbull/DCAA procedure enables sphincter preservation in complex pelvic disorders, particularly postoperative fistulas. Despite frequent major LARS and incontinence, 81% of the patients avoided permanent stoma. Meticulous selection and informed consent are essential because of the functional limitations.
Arlt G, Doyon F, Magdeburg R, Kienle P
Impact of advanced therapy initiation on antibiotic dependence in chronic pouchitis.★ Inflammatory bowel diseases | 2026-05-27
A quarter of patients with ulcerative colitis who undergo total proctocolectomy with ileal pouch-anal anastomosis experience chronic pouchitis. While advanced therapies (ATs) are effective in some patients, their impact on antibiotic dependence is unclear. In a multicenter, retrospective study, we identified adults with chronic pouchitis during treatment with AT. Those with complete pre-AT antibiotic data formed the “incident AT user” cohort. Those with only post-AT data formed the “prevalent AT user” cohort. Antibiotic prescription was modeled as percentage of time, calculated as the number of weeks of antibiotic prescription during the weeks of observed time. The pooled prevalence of antibiotic use during AT was calculated in a systematic review and meta-analysis,. Of the 67 incident AT users, 24 (36%) initiated treatment with tumor necrosis factor-α antagonist, 17 (25%) with anti-integrin, 23 (34%), with interleukin (IL) inhibitors (anti-IL), and 3 (5%) with Janus kinase inhibitors. The mean time on antibiotics was unchanged from 38% to 33% after AT initiation, and 61% of patients (n = 44) had a reduction in antibiotic use. Compared to the patients without reduction, the reduction group had a higher proportion of patients on anti-IL (46% vs 15%, adjusted odds ratio [OR] 11.1; 95% CI, 2.12-57.62). There were no differences in disease-related parameters. Seventy-nine percent (22/28) of prevalent AT users required antibiotics. On meta-analysis, pooled prevalence of antibiotic use was 0.46 (95% CI, 0.35-0.57). Just over half of patients on AT for chronic pouchitis saw reduced antibiotic use; however, further studies are needed to identify impact of AT on antibiotic use and define which patients benefit from immune-mediated vs microbiome-directed therapy.
Pan Y, Dunleavy KA, Ananthakrishnan AN
Interpretation of surgical recurrence in the dynamic phenotype of Crohn’s disease. European journal of gastroenterology & hepatology | 2026-05-27
A propensity score-matched NSQIP analysis comparing open, laparoscopic, and robotic approaches for total abdominal colectomy with end ileostomy in inflammatory bowel disease. Techniques in coloproctology | 2026-05-27
Minimally invasive surgical techniques have improved outcomes in colorectal surgery, but comparative data on their use in total abdominal colectomy with end ileostomy for inflammatory bowel disease remain limited. This study aimed to compare postoperative outcomes among patients undergoing robotic, laparoscopic, or open total abdominal colectomy for inflammatory bowel disease. We performed a retrospective cohort analysis using propensity score matching to control for baseline differences across patients. Data were obtained from the 2022 American College of Surgeons National Surgical Quality Improvement Program, a national surgical outcomes registry. Adult patients who underwent total abdominal colectomy with end ileostomy for ulcerative colitis or Crohn’s disease were included. Patients were treated with robotic-assisted, laparoscopic, or open total abdominal colectomy with end ileostomy. The primary outcome was any postoperative complication within 30 days of surgery. Secondary outcomes included operative time, conversion to open surgery, length of hospital stay, 30-day readmission, and other specific postoperative complications such as surgical site infection and renal insufficiency. A total of 581 matched patients were analyzed, including 83 robotic, 415 laparoscopic, and 83 open cases. There were no significant differences in overall 30-day morbidity across groups. Robotic surgery had significantly longer operative time than laparoscopic but not open surgery. Organ space infections and renal complications were more common in the robotic group compared with laparoscopic. Although robotic surgery was associated with shorter hospital stay, it also had the highest 30-day readmission rate. Robotic total abdominal colectomy demonstrated similar overall morbidity and conversion rates compared with other approaches but was associated with longer operative time, increased complications, and higher readmissions. Further refinement of perioperative protocols and patient selection may improve outcomes.
Alam IS, Aydinli HH, Gajic Z, Atallah C, Safar B, Simon J, Grieco MJ, da Luz Moreira A
Endoscopic recurrence of Crohn’s disease following laparoscopic versus robotic ileocolic resection. Techniques in coloproctology | 2026-05-26
Robotic approach is increasingly being used for surgery in Crohn’s disease. Robotic ileocolic resection (ICR) for Crohn’s disease (CD) is comparable to laparoscopic ICR for short term outcomes; however, no studies have compared longer-term recurrence rates between these approaches. The objective was to compare longer-term recurrence rates between these approaches. We performed a retrospective cohort study using a deidentified single institution research database containing data extracted from the electronic health record. We included all patients with CD who underwent minimally invasive ICR between 2017 and 2024. The primary outcome was endoscopic recurrence within 18 months postoperatively, defined as Rutgeerts score ≥ i2. The time-to-event analysis was performed to compare time to endoscopic recurrence between laparoscopic versus robotic ICR. A total of 164 patients were included in study, with a predominant majority prescribed an advanced medical therapy postoperatively (93.9%). Within 18 months postoperatively, 22/164 (13.4%) patients experienced endoscopic recurrence: 16/127 (12.5%) in the laparoscopic cohort and 6/37 (16.2%) in the robotic cohort. In the time-to-event analysis, there was no statistically detectable difference in Kaplan-Meier curves compared between laparoscopic and robotic ICR (log rank p = 0.115). In multivariable Cox proportional hazards models adjusted for smoking history and history of ICR, there was no statistically detectable difference in endoscopic recurrence rates within 18 months postoperatively compared between laparoscopic and robotic ICR (HR 1.12, 95% CI 0.341-3.74, p = 0.842). In this retrospective cohort, no statistically detectable differences in endoscopic recurrence between approaches was observed; however, conclusions are limited by small sample size, low event rates, and widespread postoperative biologic use and should be interpreted as exploratory only..
Kuo MC, Younan SA, Williams PJ, Lee H, Pabla B, Horst S, Hawkins AT, Khan A
[Textbook outcome after ileoanal pouch operation for ulcerative colitis: results of nationwide multicenter study]. Chirurgie (Heidelberg, Germany) | 2026-05-26
10 Strategies for prevention of perineal wound dehiscence after intersphincteric proctectomy for perianal Crohn’s disease. Techniques in coloproctology | 2026-05-25
Non-healing perineal wounds (NHPWs), including persistent presacral sinuses, remain a common and morbid complication after elective intersphincteric proctectomy (ISP) for fistulizing perianal Crohn’s disease (pCD), with reported healing rates of approximately 70% at 1 year. These complications significantly impair quality of life and increase healthcare utilization, highlighting the importance of prevention. This narrative review summarizes contemporary evidence and expert practice to present ten pragmatic strategies to reduce perineal wound dehiscence after ISP for pCD. Prevention begins with comprehensive preoperative optimization, including correction of malnutrition and anemia, minimization of corticosteroid exposure, smoking and nicotine cessation, and optimization of relevant medical comorbidities. Careful assessment and control of Crohn’s disease activity are emphasized through current disease staging, proactive therapeutic drug monitoring, and aggressive surgical control of perianal sepsis. These measures often involve repeated examinations under anesthesia, drainage of abscesses and fistula tracts, fecal diversion when indicated, and selective use of hyperbaric oxygen therapy to improve local conditions before definitive surgery. Operative strategies focus on technical decisions that minimize perineal wound burden and promote healing. Key elements include performing proctectomy in the intersphincteric plane with total mesorectal excision when feasible, meticulous debridement and management of fistula tracts, and robust multilayered perineal closure. Adjunctive techniques such as horizontal mattress suturing of the levators to enhance tissue apposition, use of pedicled omental flaps with fluorescence angiography to confirm perfusion, and prophylactic incisional negative pressure wound therapy are highlighted. Collectively, these strategies provide a practical framework to reduce perineal wound complications after ISP for pCD.
Holubar SD, Tozer P
Histopathologic characterization and clinical associations of ileal pouch polyps in inflammatory bowel disease. Gastroenterology report | 2026-05-24
Polyps are frequently found in patients with chronic inflammatory disorders of the pouch. While neoplastic transformation is the major concern, most pouch polyps are non-dysplastic. Benign polyps may lead to anemia or obstruction; however, their histologic features remain poorly defined. Patients with pouch polyps and inflammatory bowel disease (IBD) were identified from a prospectively maintained database at Columbia University Irving Medical Center between 2020 and 2023, with two additional cases from the University of California, San Francisco. Patients with familial adenomatous polyposis were excluded. The primary outcomes were the histologic characterization and its correlation with clinical features. Seventy polyps from 21 patients were evaluated. Two polyps from the same patient showed low-grade dysplasia (2.9%). The remaining 68 non-dysplastic polyps were classified as pyogenic granuloma-like (PGLP; n = 46, 67.6%), prolapse-like (PLP; n = 13, 19.1%), or inflammatory (IP; n = 9, 13.2%). PGLPs were more common in the proximal pouch, while PLPs and IPs predominated in the distal pouch (P = 0.021 and P = 0.002, respectively). An endoscopic snow-capped appearance was significantly associated with PGLPs (P < 0.001). On histology, PGLPs (87.0%) and PLPs (92.3%) were more commonly associated with fibrinous exudate than IPs (44.4%, P = 0.011 and P = 0.023, respectively). Nineteen patients underwent endoscopic polypectomy. Mean serum hemoglobin levels increased from 12.1 ± 2.2 to 12.8 ± 2.2 g/dL post-polypectomy (P = 0.285). Pouch polyps recurred in 8 patients (42.1%), with a median interval of 2.4 years. Neoplastic transformation is rare in pouch polyps, but benign polyps may have clinical consequences. PGLPs were most common, presenting distinct endoscopic and histologic features, followed by PLPs and IPs. Polypectomy may improve hemoglobin levels.
Guo Y, Wang S, Choi WT, Shen B, Ko HM
Organ Preservation After Total Neoadjuvant Therapy in a Patient With Low Rectal Adenocarcinoma and Crohn’s Disease.Case report ACG case reports journal | 2026-05-22
Inflammatory bowel disease (IBD) is a relative contraindication to radiation. This case report describes a 53-year-old man with colorectal adenocarcinoma and a history of Crohn’s disease who was treated under the organ preservation for rectal adenocarcinoma protocol to avoid total mesorectal excision. Over 30 months of follow-up, the patient continues to tolerate chemoradiotherapy and consolidation chemotherapy with manageable toxicity and achieved a sustained complete clinical response. This case supports emerging evidence that radiation may be feasible in select patients with IBD and highlights the potential role of non-surgical organ preservation strategies in colorectal cancer, even in the context of underlying IBD.
Leong R, Goodwin R, Moloo H, Shabana W, Locke G
ASSOCIATED FACTORS AND CLINICAL ASPECTS OF COLECTOMY IN PATIENTS WITH ULCERATIVE COLITIS - EXPERIENCE OF A BRAZILIAN SOUTHEASTERN COHORT.Observational study Arquivos de gastroenterologia | 2026-05-22
Despite recent advances in the medical treatment of ulcerative colitis (UC) involving the use of biological agents and small molecules, a proportion of patients with UC still require surgical treatment. This study evaluated patient characteristics and factors associated with colectomy in patients with UC at a tertiary IBD center. This is a retrospective and observational study utilizing the database at our university hospital. The sample comprised 232 patients diagnosed with UC, with a mean age of 46.45±15.00 years, 60.3% of whom were women. The patients were divided into two groups depending on whether or not they had undergone colectomy between January 2001 and December 2018. Of all 50 (21.6%) patients underwent colectomy. Clinical intractability (40.0%) and acute severe colitis (22%) were the main indications for colectomy. Longer disease duration (P=0.035), pancolitis (82.0% vs 6.0%; P<0.001) when compared to proctitis, higher endoscopic Mayo sub-score (Mayo 3: 22.0% vs Mayo 1: 5.5%; P<0.0001), and initial use of biological agents (14.0% vs 1.1%; P<0.001) were significantly associated with the occurrence of colectomy. There was no difference in the distribution of cases according to sex, race, smoking, previous use of corticosteroids, and extraintestinal manifestations (P>0.05). Our study shows that a longer disease duration, extensive disease (pancolitis), and higher severity of UC at diagnosis were associated with a poor prognosis, culminating in a higher need for surgical intervention. Apesar dos recentes avanços no tratamento clínico da Retocolite Ulcerativa (RCU) envolvendo o uso de agentes biológicos e pequenas moléculas, uma proporção de pacientes com RCU ainda necessita de tratamento cirúrgico. Este estudo teve como objetivo avaliar as características dos pacientes e os fatores associados à colectomia em pacientes com RCU em um centro terciário de DII. Trata-se de um estudo retrospectivo e observacional utilizando o banco de dados do nosso hospital universitário. A amostra foi composta por 232 pacientes com diagnóstico de RCU, com idade média de 46,45±15,00 anos, sendo 60,3% mulheres. Os pacientes foram divididos em dois grupos dependendo de terem sido submetidos ou não à colectomia entre janeiro de 2001 e dezembro de 2018. Do total 50 (21,6%) pacientes foram submetidos à colectomia. A intratabilidade clínica (40,0%) e a colite aguda grave (22%) foram as principais indicações de colectomia. Maior tempo de doença (P=0,035), pancolite (82,0% vs 6,0%; P<0,001) quando comparada à proctite, maior subescore endoscópico de Mayo (Mayo 3: 22,0% vs Mayo 1: 5,5%; P<0,0001) e o uso inicial de agentes biológicos (14,0% vs 1,1%; P<0,001) estiveram significativamente associados à ocorrência de colectomia. Não houve diferença na distribuição dos casos segundo sexo, raça, tabagismo, uso prévio de corticoide e manifestações extraintestinais (P>0,05). O nosso estudo demonstrou que a maior duração da doença, a doença extensa (pancolite) e a maior gravidade da UC ao diagnóstico estiveram associadas a um mau prognóstico, culminando numa maior necessidade de intervenção cirúrgica.
Ferreira SDC, Parra RS, Perdoná GDSC, Rezende REF, Aprile LRO, Féres O
A rare and severe case of toxic megacolon: Radiological emergency.Case report Radiology case reports | 2026-05-16
Toxic megacolon is a rare and life-threatening complication of ulcerative colitis, representing a medical and surgical emergency with a poor prognosis. We report the case of a 31-year-old man with no significant past medical history, admitted for a 15-day history of bloody mucoid diarrhea associated with general health deterioration. Endoscopic and histopathological findings were consistent with a severe inaugural flare of ulcerative colitis. Despite optimal medical management, the clinical course was marked by the abrupt onset of septic shock. Abdominal imaging revealed acute colonic dilatation consistent with toxic megacolon, leading to an indication for emergency subtotal colectomy. The outcome was unfavorable, with the patient’s death occurring in the context of multiorgan failure.
Abddaimi S, Benramdane H, Boubacar A, Ziani H, Nasri S, Kamaoui I, Skiker I
Extraintestinal Manifestations (11 papers)
Surgical management of metastatic cutaneous Crohn’s disease: a case series from a tertiary centre in the United Kingdom. Techniques in coloproctology | 2026-05-29
Metastatic Crohn’s disease (MCD) is a rare extra-intestinal manifestation (EIM) of Crohn’s disease (CD), defined by granulomatous inflammation of skin non-contiguous to the gastrointestinal tract. This study describes the clinical features, surgical management and wound healing outcomes of the largest national surgical cohort of patients with severe MCD, a topic that remains poorly represented in the literature. This retrospective single-centre case series included adults (> 18 years) undergoing surgical management for MCD from 2019 to 2024. Diagnosis was confirmed by expert clinical and histopathological assessment. We describe pre-operative optimisation, individualised surgical approaches and post-operative management delivered by a multi-disciplinary team led by consultant colorectal and plastic surgeons. Wound healing was assessed clinically in a specialist complex wounds clinic at 6 and 12 months and at final long-term follow-up. Eleven female patients (median age 37 years) underwent surgical intervention. At 6 and 12 months, 45.5% achieved complete healing, improving to 81.8% by final follow-up (median 36 months). Most underwent a combined medical and surgical approach with proctocolectomy and tailored perineal reconstruction. Persistent lesions and non-healing ulcers required additional adjuncts to treatment which included topical tacrolimus, hyperbaric oxygen therapy and surgical re-excision to improve healing outcomes. MCD is a challenging condition requiring surgical treatment in refractory cases despite medical therapy. Our study highlights the need for multidisciplinary working alongside meticulous pre-operative optimisation and close post-operative follow-up to improve long-term wound healing outcomes for patients with this rare and complex disease.
Selvakumar D, Leiberman D, O’Connor A, Lyon CC, Brass A, McLaughlin J, Winterton R, Cruickshank SM, Hancock L
Choosing NSAID treatment in axial spondyloarthritis: factors guiding clinical decision-making.Review Current opinion in rheumatology | 2026-05-28
Nonsteroidal anti-inflammatory drugs (NSAIDs) are first-line therapy for axial spondyloarthritis (axSpA), improving pain, function, and disease activity. This review evaluates evidence for NSAID efficacy, potential disease modification, and safety considerations in patients with axSpA, particularly those with inflammatory bowel disease (IBD) or elevated cardiovascular risk. Evidence for NSAID-mediated disease modification remains inconsistent. In patients with IBD, contemporary data suggest variable risk of disease exacerbation depending on NSAID selectivity and exposure patterns. Established gastrointestinal toxicities persist outside the IBD context, though risk-mitigation strategies are available. While general-population studies demonstrate increased cardiovascular risk with certain NSAIDs, emerging axSpA-specific observational data suggest a smaller excess risk of major adverse cardiovascular events, potentially reflecting the counterbalancing effect of inflammation control. Pharmacogenomic data increasingly support CYP2C9 variation as a determinant of NSAID exposure and toxicity. NSAIDs remain foundational in axSpA management, but long-term use requires individualized assessment of gastrointestinal, cardiovascular, and IBD-related risks. Pharmacogenomic considerations may further refine patient selection and dosing strategies.
Gensler LS, McKay CE, Mayer AS
Communicating Risk and Safety of Inflammatory Bowel Disease Therapies.★ The American journal of gastroenterology | 2026-05-27
Inflammatory bowel diseases (IBD) often require long-term treatment with advanced therapies, including biologics and small molecules. The use of these agents must be carefully balanced against the risks of uncontrolled gastrointestinal inflammation and the potential for treatment-related adverse events. This review synthesizes contemporary evidence on malignancy, infection, venous thromboembolism (VTE), and major adverse cardiovascular events (MACE) in IBD, integrating risks attributable to underlying disease and those conferred by specific drug classes, with the goal of improving how clinicians communicate these risks to patients. Chronic intestinal inflammation increases the risk of colorectal cancer, small bowel adenocarcinoma, intestinal lymphoma, anal cancer in fistulizing Crohn’s disease, and cholangiocarcinoma in those with primary sclerosing cholangitis, alongside modest excesses in select extraintestinal malignancies. Thiopurines increase the risk for lymphoma, particularly when combined with anti-TNF agents, and non-melanoma skin cancer. Corticosteroid use is the major driver of serious infection, VTE, and MACE, while combination anti-TNF-thiopurine therapy, JAK inhibitors, and S1P receptor modulators are associated with therapy- and context-specific infectious and thrombotic risks, which remain low in absolute terms for most patients. Across outcomes, we emphasize absolute risk and patient-level modifiers, and provide pictorial tools that depict clinically meaningful risks to support shared decision-making and individualized, evidence-based risk communication with patients.
Axelrad JE, Faye A, Siegel CA
Anti-Integrin αvβ6 Autoantibodies as Diagnostic and Monitoring Biomarkers for Pediatric-Onset Primary Sclerosing Cholangitis. Hepatology research : the official journal of the Japan Society of Hepatology | 2026-05-27
Pediatric primary sclerosing cholangitis (PSC) is a rare progressive cholestatic liver disease that often presents diagnostic challenges owing to overlapping clinical and histological features with autoimmune hepatitis (AIH). We hypothesized that anti-integrin αvβ6 autoantibodies may serve as a noninvasive biomarker to differentiate pediatric PSC from AIH and monitor disease activity. We retrospectively analyzed serum samples from 65 patients with pediatric-onset PSC, 39 with AIH, and 66 controls. Anti-integrin αvβ6 autoantibodies were quantified using enzyme-linked immunosorbent assay. Functional activity of the autoantibodies was assessed using a solid-phase fibronectin-binding inhibition assay. Anti-integrin αvβ6 autoantibody levels were significantly higher in pediatric-onset PSC than in AIH and controls. The sensitivity and specificity for distinguishing PSC were 63.9% (95% confidence interval [CI]: 51.4-74.8) and 97.1% (95% CI: 91.9-99.2), respectively. Higher levels were observed in PSC with inflammatory bowel disease than without (p = 0.0069) and in PSC-AIH overlap compared with AIH alone (p = 0.0018). In one case, rising autoantibody levels preceded the clinical transition from AIH to PSC-AIH overlap. Levels declined during remission and after liver transplantation; however, increased again upon recurrence. Functional assays demonstrated that autoantibodies from patients with pediatric-onset PSC inhibited binding of integrin αvβ6 to fibronectin. Anti-integrin αvβ6 autoantibodies may serve as a noninvasive clinically informative biomarker for distinguishing pediatric-onset PSC from AIH and reflecting longitudinal changes in disease activity, including posttransplant recurrence. These findings support their potential clinical utility in the diagnosis and longitudinal assessment of pediatric-onset PSC.
Maeda Y, Umetsu S, Hiejima E, Suzuki M, Iwama I, Kimura T, Kondo S, Inui A, Kondou H, Okamoto T
Recent updates in human leukocyte antigen B27-associated uveitis.Review Indian journal of ophthalmology | 2026-05-27
There has been progressive understanding in etiopathogenesis, clinical presentation, and effective treatment of anterior uveitis (AU) over the years. Sudden onset, symptomatic acute anterior uveitis (AAU) in a young adult, often male, classically arouses suspicion for human leukocyte antigen (HLA) B27-related uveitis. While the ocular presentation is frequently the earliest manifestation, its systemic counterparts within the spectrum, viz., spondyloarthropathies (SpA), including ankylosing spondylitis (AS), reactive arthritis (RA), psoriatic arthritis (PA), and inflammatory bowel disease-associated inflammation, pose greater diagnostic and therapeutic challenges for rheumatologists and internists. This places the ophthalmologist in a uniquely advantageous yet responsible position in initiating etiologic evaluation and facilitating early systemic recognition. Rapid advances in immunology and molecular medicine have significantly expanded the diagnostic and therapeutic landscape of HLA B27-related disease. Emerging insights implicating the gut microbiome, autoinflammatory mechanisms, and innate immune dysregulation have reshaped traditional concepts of pathogenesis. Concurrently, an improved understanding of cytokine networks and immune signaling pathways has led to the development of targeted biologic and synthetic disease-modifying therapies. Given the dynamic, multisystem nature of HLA B27-associated disease and its variable organ involvement, optimal management necessitates close multidisciplinary collaboration among ophthalmologists, rheumatologists, gastroenterologists, and internists. This article briefly explores the evolving concepts of the complex enigma of the HLA B27 molecule and the basis for recent trends in its understanding at the cellular, molecular, biochemical, and clinical levels.
Narain S, Gupta P, Pyare R, Shroff D, Rath PD
Large vessel vasculopathy: An underrecognized complication in Wiskott-Aldrich syndrome. Journal of human immunity | 2026-05-26
Autoimmune manifestations occur in 25-75% of patients with Wiskott-Aldrich syndrome (WAS), commonly including autoimmune hemolytic anemia, skin vasculitis, IgA nephropathy, arthritis, and inflammatory bowel disease. Large vessel vasculopathy is rarely reported in WAS. We present a review of children with WAS and evidence of large vessel vasculopathy at our center, analyzing clinical, radiological, immunological, and genetic data. Among 80 patients diagnosed with WAS over two decades, four children (aged 10-18 years) developed large vessel vasculopathy. Two had classical WAS with bleeding, recurrent infections, and eczema since infancy, while two had milder phenotypes and presented for the first time during this illness. Clinical features included chest pain and heart failure, abdominal pain, upper limb claudication, and differential blood pressure. Imaging demonstrated aneurysmal dilatation of the aorta and its major branches. Epstein-Barr virus viremia was detected in three patients. All received intravenous immunoglobulin and immunosuppressive therapy; none could undergo hematopoietic stem cell transplantation (HSCT), and three patients died. Large vessel vasculopathy is a rare but life-threatening complication of WAS, underscoring the importance of early recognition and timely consideration of HSCT.
Suri D, Nadig PL, Desai D, Sharma Y, Jamal A, Vaitheeswaran GC, Choudhary H, Sudhakar M, Aggarwal R, Basu S
A Tangled Tale: Type 2 Autoimmune Pancreatitis With a Sclerosing Twist.Case report ACG case reports journal | 2026-05-26
Autoimmune pancreatitis (AIP) is an uncommon immune-mediated condition that can mimic pancreatic cancer and present with obstructive jaundice. Type 2 AIP is IgG4-independent and commonly associated with inflammatory bowel disease. We describe a woman with Crohn’s disease who presented with abdominal pain, jaundice, and cholestatic liver injury. Imaging showed pancreatic head enlargement and biliary strictures concerning for malignancy. Initial biopsy and serology were inconclusive with normal immunoglobulin subclass 4 levels. Endoscopic ultrasound demonstrated chronic pancreatic inflammation, and corticosteroid therapy led to marked improvement, supporting a diagnosis of type 2 AIP complicated by secondary sclerosing cholangitis and type 3c diabetes.
Husain KH, Hagen R, Thakkar B, Promagan N, Parikh ND
Metastatic Crohn Disease Manifesting as Granulomatous Cheilitis in a Patient With Well-Controlled Crohn Disease.Case report ACG case reports journal | 2026-05-22
Crohn disease (CD) can affect any organ system outside the gastrointestinal tract, and these conditions are classified as extraintestinal manifestations and include arthritis, uveitis, and cutaneous manifestations. Cutaneous involvement includes erythema nodosum, pyoderma gangrenosum, and metastatic CD. The latter can be defined as a granulomatous skin lesion that is noncontiguous to the intestinal disease. In this article, we report a rare case of a 48-year-old woman with CD in endoscopic and clinical remission with chronic persistent orofacial granulomatosis of the lip secondary to CD, despite the absence of active intestinal disease and describe its management.
Almusabeh H, Shepherd K, Elfert K, Awan R, Beatty C, Tandon K, Hadam-Veverka J
Extraintestinal Manifestations of Inflammatory Bowel Disease: A Focus on Kidney Complications.Review International journal of molecular sciences | 2026-05-21
Inflammatory bowel disease (IBD), comprising Crohn’s disease (CD) and ulcerative colitis (UC), is a chronic relapsing-remitting condition characterized by systemic and intestinal inflammation and immune dysregulation. Up to 47% of IBD patients develop extraintestinal manifestations, yet kidney and urological involvement remain underrecognized. Accumulating evidence has linked IBD to nephrolithiasis, glomerular diseases, tubulointerstitial nephritis, acute kidney injury, chronic kidney disease, and, rarely, amyloid A amyloidosis. Population studies have consistently shown elevated risks for various important kidney disorders in IBD, with CD generally posing a greater risk than UC. The pathogenesis of kidney complications in IBD reflects complex gut-kidney interactions, including metabolic and absorptive abnormalities, shared genetic and immune pathways, intestinal dysbiosis with nephrotoxic microbial metabolites, systemic inflammation, and drug-related nephrotoxicity. Strategies for kidney protection in IBD include increased awareness, close monitoring of kidney function, urinary metabolic profiling in high-risk patients, and prompt nephrology referral for early detection and treatment. Management should include an effective and sustained control of intestinal inflammation, discontinuation of potential nephrotoxic drugs when indicated, and timely diagnosis and treatment of kidney manifestations, as well as integrating kidney complications into IBD guidelines to enhance awareness, ultimately optimizing both the kidney and overall outcomes for IBD patients. Future studies are needed to validate the potential predictive biomarkers for kidney complications and to develop targeted interventions to address shared gut-kidney pathogenic mechanisms in IBD.
Wu H, Lin A, Chi J, Zhang J, Peng B, Ni D, Hao H, Liu Z
Spine structural lesions in ankylosing spondylitis: comparison between radiographic and opportunistic thoraco-abdomino-pelvic computed tomography assessment. Clinical and experimental rheumatology | 2026-05-21
The aim of this study was to evaluate the prevalence and severity of spinal structural lesions on radiographs versus opportunistic thoraco-abdomino-pelvic CT (TAP CT) in ankylosing spondylitis (AS). This monocentric retrospective pilot study included AS patients meeting the modified New York criteria for radiographic sacroiliitis who had both spine radiographs and TAP CT within 12 months. On CT, 36 anterior vertebral corners (C7-S1) were graded for erosion/squaring (grade 1), syndesmophytes (grade 2), and bone bridges (grade 3). Posterior facet joint ankylosis was recorded as present or absent, generating anterior, posterior, and total CT-scores (0-216). Radiographic assessment was performed using the Radiographic Ankylosing Spondylitis Spinal Score (RASSS, 0-84). A total of 142 patients were included (median age 54 years [47-62], 70.4% male, 77.6% HLA-B27 positive, median disease duration 14 years [6-26], 43.5% treated with bDMARDs). Structural spinal damage was identified in 62.6% by RASSS and 71.8% by CT. Anterior vertebral lesions were present in 94 patients, and 68 exhibited posterior facet joint ankylosis. Mean RASSS and total CT-scores were 13.1 (±20.0) and 37.2 (±47.2), respectively. Total CT-score correlated with age, disease duration, male sex, HLA-B27 positivity, inflammatory bowel disease, and CRP >5 mg/L (p<0.05). Multivariate analysis confirmed associations with age, disease duration, male sex, and CRP. Intra-reader reliability was excellent for both modalities (ICC >0.90). Opportunistic TAP CT is a reliable, reproducible, and complementary imaging tool to radiography for evaluating anterior and posterior spinal structural damage in AS.
Morizot C, Favre-Félix I, Mennini A, Bauer E, Chary-Valckenaere I, Loeuille D
The role of a multidisciplinary approach in the early and differential diagnosis of inflammatory bowel disease-related spondyloarthritis: insights from a cross-sectional study. Frontiers in medicine | 2026-05-12
Inflammatory bowel disease-related spondyloarthritis (IBD-SpA) commonly complicates IBD. Early diagnosis is essential; however, it is often delayed due to clinical heterogeneity and the lack of specific diagnostic criteria. This study aimed to evaluate the outcomes of close collaboration between gastroenterologists and rheumatologists in the classification of the musculoskeletal (MSK) manifestations in IBD patients, focusing on the early diagnosis of IBD-SpA and its differentiation from other conditions. Consecutive IBD outpatients underwent a comprehensive rheumatologic evaluation during a joint rheumatologist-gastroenterologist consultation, including the DETection of Arthritis in Inflammatory boweL diseases (DETAIL) screening questionnaire, and, when appropriate, laboratory and imaging investigations. Suspected IBD-SpA cases were classified as newly diagnosed IBD-SpA, having an alternative arthropathy diagnosis, or having non-specific arthralgias, and their characteristics were analyzed. A total of 605 IBD patients were evaluated. At the first assessment, 81 patients had a pre-existing diagnosis of SpA and 117 patients of suspected IBD-SpA cases were identified. Among the latter assessment, 18 (15%) were confirmed as new IBD-SpA diagnoses, resulting in a 22% relative increase in the total number of SpA cases and raising the overall prevalence from 13.4 to 16.4%. Patients with axial involvement experienced a longer diagnostic delay (mean 12.4 vs. 2.9 years, p = 0.035). Of the new IBD-SpA diagnoses, 72% resulted in treatment modifications jointly decided by the gastroenterologist and rheumatologist. However, 85% of suspected IBD-SpA cases were ultimately excluded, with 60% classified as other arthropathies (primary osteoarthritis and fibromyalgia) and 25% as non-specific arthralgias. The swollen joint count was the only significant predictor of a new IBD-SpA diagnosis (adjOR 5.70, p < 0.001), with a trend toward significance for fecal calprotectin levels ≥200 μg/g (adjOR 2.88, p = 0.070). The multidisciplinary approach enables early and accurate diagnosis of IBD-SpA, minimizing the risk of misclassification of musculoskeletal manifestations and unwarranted treatment changes.
Floris A, Sichi L, Favale A, Falconi M, Pace A, Angioni MM, Italia A, Piras R, Olla F, Onnis F
Pediatric IBD (9 papers)
Update on Novel Biologic Therapies for Crohn Disease and the Impact of Imaging on Clinical Decision Making.Review Radiographics : a review publication of the Radiological Society of North America, Inc | 2026-06
As Crohn disease treatment rapidly evolves, imaging has a critical role in treatment response assessment and clinical decision making. Therapy is often “top down,” with the most powerful and potent therapies selected first. Disease activity assessment remains multifactorial, integrating source data from biomarkers, symptoms, endoscopy, and imaging. The “treat-to-target” approach also integrates these markers to escalate, de-escalate, or switch therapies. Given the transmural nature of Crohn disease, endoscopic mucosal healing (ie, the current treatment target) may not be sufficient evidence of remission, and imaging assessment of transmural healing could prove a better predictor of treatment response and long-term patient outcomes. Quantitative imaging methods have been developed to standardize treatment response assessment, including emerging radiologic techniques such as contrast-enhanced US, T1 mapping at MRI, standardized stricture assessment, and velocity-encoded phase contrast imaging. Morphologic changes of resolving inflammation at imaging may lag behind clinical response, and complete normalization of inflamed bowel segments may occur infrequently. In these cases, evaluating changes in bowel motility may be may be more helpful for detection of early treatment response. The radiologist is critical in the assessment of Crohn disease, providing insight into disease management and endoscopically occult and subclinical inflammation. The goal of this article is to highlight the role of imaging in driving management of Crohn disease, including endoscopically occult and subclinical disease, transmural healing, and treatment decision making in patients undergoing biologic therapies. ©RSNA, 2026 See the invited commentary by Srinivasan and Taylor in this issue.
Patel RD, Keyashian K, Nazarian M, Dillman JR, Deepak P, Fletcher JG, Fidler JL, Anupindi SA, Dane B, Gee MS
Retrospective Review of Pediatric Psoriasis and TNF-Inhibitor Induced Psoriasiform Disease in Patients With Skin of Color. Journal of cutaneous medicine and surgery | 2026-05-28
Psoriasis affects ~3% of the adult U.S. population, with known differences in prevalence, presentation, and treatment outcomes across racial and ethnic groups. In pediatric populations, disparities in psoriasis recognition may lead to delayed diagnosis and undertreatment, especially in patients with skin of color (SoC). To compare clinical presentation and treatment patterns in pediatric patients with psoriasis with and without SoC at a single tertiary-care pediatric center. We conducted a retrospective, case-control cohort study of patients diagnosed with psoriasis (including TNF-associated psoriasis) before age 18 at SickKids Hospital (January 2008-March 2024). Inclusion criteria were systemic treatment before or after diagnosis of psoriasis and available photo documentation. Patients were stratified by skin phototype based on the Massey-Martin Scale for SoC. Demographics, clinical features, and treatment patterns were compared between SoC and non-SoC groups. Among 115 patients, 42.6% were classified as SoC. Scalp involvement (P = .008), inflammatory bowel disease (P = .05), and arthritis were more common in non-SoC patients. SoC patients had a shorter time to diagnosis and were more likely to receive cyclosporine initially and methotrexate overall. Non-SoC patients had higher biologic use throughout care (77.2% vs 63.2%). Topical corticosteroids were the most prescribed treatment across both groups. Pediatric patients with and without SoC showed distinct trends in disease presentation and management. Differences in clinical presentation and medication use highlight the need for increased awareness of psoriasis manifestations in diverse skin types. Prospective studies with standardized assessment tools could help addressing the differences described in this study.
Muylaert Barrett B, Pastukhova E, Lansang P, Sibbald C
Dietary fiber in pediatric gastrointestinal health: a narrative review of evidence and challenges. Clinical and experimental pediatrics | 2026-05-27
Dietary fiber plays a central role in pediatric gastrointestinal health; however, most children worldwide consume amounts well below recommended levels. Current pediatric guidelines from the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition (2014) and global nutrition guidance from the World Health Organization recommend adequate dietary fiber intake as part of a balanced diet to support digestive health and prevent noncommunicable diseases. These recommendations generally correspond to daily fiber intake levels of approximately 14-31 g/day, or the practical rule of age (years) + 5 g/day for children, yet more than 80%-90% of children fail to meet these targets. This shortfall is clinically significant, as inadequate fiber intake is associated with increased risk of functional constipation, a condition affecting approximately 3%-29% of children globally. Dietary fiber contributes not only to stool bulk but also to the modulation of gut microbiota, gastrointestinal barrier function, and immune and metabolic pathways during critical developmental stages. Among common pediatric gastrointestinal disorders, the strongest evidence supports fiber use in constipation management, where supplementation or increased intake through whole foods has been shown to improve stool frequency and consistency in approximately 50%-60% of affected children. However, clinical trial outcomes remain inconsistent, varying according to fiber type, dosage, duration of intervention, and diagnostic criteria. Evidence for recurrent or functional abdominal pain remains limited and heterogeneous, with small sample sizes, differing endpoints, and high placebo response rates complicating interpretation. In pediatric inflammatory bowel disease, fermentable fibers have been shown to enhance short-chain fatty acid production. Nevertheless, robust pediatric clinical evidence remains insufficient, and findings from adult ulcerative colitis studies cannot be directly extrapolated to children. Dietary fiber represents an important supportive component of pediatric gastrointestinal management, but standardized dosing recommendations and high-quality pediatric clinical trials are still needed to establish evidence-based guidelines for clinical practice.
Das R, Thatal B, Tamang B
THE IMPACT OF OBESITY ON THE CLINICAL COURSE OF INFLAMMATORY BOWEL DISEASE.Observational study Arquivos de gastroenterologia | 2026-05-25
The incidence and prevalence of disorders such as obesity, metabolic syndrome (MS), and inflammatory bowel disease (IBD) have increased over recent decades. MS is a complex condition represented by a cluster of cardiovascular risk factors with a multifactorial origin-including genetic, behavioral, dietary factors, and alterations in gut microbiota. IBD reflects a complex and heterogeneous immune-mediated condition that typically, though not exclusively, affects the intestine. To evaluate the impact of obesity on the clinical course of IBD in a cohort of patients followed at a referral center for IBD. This was a retrospective longitudinal observational cohort study including patients of both sexes and all ethnicities, followed at the Inflammatory Bowel Disease Referral Center of the University Hospital of the Federal University of Juiz de Fora, between January 2019 and August 2023. A total of 404 adults aged 18 to 80 years with a diagnosis of IBD-established by clinical, endoscopic/histological, and/or imaging criteria-were included. IBD cases were classified as either Crohn’s disease (CD) or ulcerative colitis (UC). To assess DII annual activity, electronic medical records were reviewed for outpatient visits and hospitalizations from 2019 to 2023. CD was considered active when the Harvey-Bradshaw Index (HBI) was ≥5, and UC was considered active when the total Mayo score was ≥3 or the partial Mayo score was ≥2. The mean age at IBD diagnosis was 37.79±13.44 years, with an average disease duration of 12.50±8.3 years. Biologic therapy was used in the majority of patients (58.4%), with treatment failure occurring in 56.8% of these cases during the study period. No statistically significant differences were observed in most outcomes, except for a higher frequency of biologic use in non-obese patients with CD (P=0.028). There was a trend toward a greater number of years with active disease in obese patients with CD (P=0.062). IBD patients with obesity were predominantly female. Among those with CD, the phenotype was mainly non-stricturing, non-penetrating, with a clinical course characterized by greater disease activity over time, suggesting that obesity may be an unfavorable factor for disease control. This trend was not observed among patients with UC. A incidência e prevalência de desordens como obesidade, síndrome metabólica (SM) e doença inflamatória intestinal (DII) aumentaram nas últimas décadas. A SM é um transtorno complexo representado por um conjunto de fatores de risco cardiovascular, tendo origem multifatorial: envolve fatores genéticos, padrões comportamentais e dietéticos, e alterações na microbiota intestinal. A DII reflete uma condição imuno mediada complexa e heterogênea que tipicamente, mas não exclusivamente, afeta o intestino. Avaliar o impacto da obesidade no curso clínico da DII em uma coorte de pacientes acompanhados em um centro de referência em DII. Trata-se de estudo de coorte observacional longitudinal retrospectivo, que incluiu pacientes de ambos os sexos e de qualquer etnia, acompanhados no Centro de Referência em Doenças Inflamatórias Intestinais do Hospital Universitário da Universidade Federal de Juiz de Fora (HU-UFJF), no período compreendido entre janeiro de 2019 a agosto de 2023.Foram incluídos 404 adultos entre 18 e 80 anos, utilizando-se de alguns critérios de exclusão, que possuíam o diagnóstico de DII, estabelecido por critérios clínicos, endoscópicos/histológicos e/ou de imagem. Quanto ao tipo de DII, foi dividido em DC ou RCU. Para avaliação da atividade da doença, foram analisados os registros eletrônicos de cada paciente durante suas consultas ambulatoriais ou hospitalizações entre os anos de 2019 e 2023, sendo que, para DC, foi considerado como atividade de doença HBI ≥5, e para RCU, quando classificado pelo Mayo total, foi considerada atividade de doença quando Mayo total ≥3, e quando analisado pelo Mayo parcial, atividade com Mayo parcial ≥2. A média de idade ao diagnóstico de DII foi de 37,79±13,44 anos e média de duração da doença de 12,50±8,3 anos. A terapia biológica foi empregada na maioria dos pacientes (58,4%), sendo que houve falha da terapia em 56,8% desses pacientes durante o período analisado. Não foi observada diferença estatisticamente significante nos diversos desfechos analisados, exceto no uso de biológicos mais frequente em pacientes com DC não obesos (P=0,028). Houve uma tendência para maior número de anos com atividade da doença em pacientes obesos com DC (P=0.062). Foi possível concluir que pacientes com DII e obesidade eram predominantemente mulheres. Aqueles com DC apresentaram fenótipo principalmente inflamatório e curso evolutivo caracterizado por maior atividade de doença ao longo do seguimento, sugerindo que a obesidade pode ser um fator desfavorável para o controle da DC. A mesma tendência não foi observada entre os pacientes com RCU.
Borsato ROR, Chebli JMF, Ribeiro TCDR, Borsato LHS, Sales MPM, Barra MAL
Benefits of Surgical Management in Ileocecal Crohn’s Disease: A Review of the Past Decade (2020-2026).Review Medicina (Kaunas, Lithuania) | 2026-05-13
Background and Objectives: The management of localized ileocecal Crohn’s disease (CD) is undergoing a significant paradigm shift from traditional “step-up” medical escalation toward proactive early surgical intervention. With the evolution of surgical therapies as well as various minimally invasive procedures, as well as a better understanding of inflammatory bowel diseases, surgery is playing a more important role in the treatment of inflammatory bowel disease. One of the most common occurrences in Crohn’s disease, the ileocecal localization can present with a lot of dilemmas regarding the optimal treatment in both adult patients and pediatric patients alike. One of the biggest challenges remains the decision between early surgery and continuous biological treatment, which can prove a challenge from multiple standpoints ranging from cost-efficiency to recurrence rate. This review highlights the latest changes in surgical management in ileocecal Crohn’s disease, focusing primarily on the anastomotic type, comparison with biological therapy, early aggressive surgery and pediatric surgery. Materials andMethods: After respecting the review criteria, 16 articles were included in our study, which emphasize the importance and the recent trends in the surgical management of the ileocecal disease. Results: All 16 articles met criteria for good quality, suggesting a low risk of bias, focusing primarily on early surgery, the role of Kono-S anastomosis as well as pediatric considerations. Conclusions: While the choice of the Kono-S anastomosis remains debatable, significant progress has been made in terms of early surgery which improves the long-term outcomes in patients while minimizing the risk of morbidity and mortality.
Balint I, Zaharie R, Dan V, Moiș E, Popa C, Ciocan A, Al-Hajjar N, Zaharie F
Incidence of Clostridium difficile infection and enteric pathogens in children with inflammatory bowel disease presenting with disease exacerbation. Frontiers in pediatrics | 2026-05-13
Pediatric patients with inflammatory bowel disease (IBD) are at increased risk of gastrointestinal infections including Clostridioides difficile infection (CDI), which can trigger disease exacerbations. Since treatment for disease flares and infections differs, identifying the infection and causative microorganisms is crucial. There is limited data on the frequency of CDI in pediatric patients with IBD in our region. This study aimed to determine the incidence of CDI and other enteric infections in pediatric patients with IBD presenting with symptoms suggestive of a flare, and to identify potential predictors of CDI. We conducted a retrospective study from 2017 to 2024, including pediatric patients with inflammatory bowel disease who presented with exacerbation of gastrointestinal symptoms suggestive of a flare-up and underwent stool testing. Demographic and clinical data, including IBD type, treatment regimens, and hospitalization status, were collected. Stool samples were analyzed for infectious pathogens. We analyzed the association between categorical variables using the Chi-square test to identify predictors of Clostridioides difficile infection (CDI). Statistical significance was set at a P-value <0.05. Stool testing was performed in 144 encounters, of which 47 (32.6%) were positive for infectious pathogens. The most commonly identified organisms were Clostridioides difficile (11.8%) and E.coli (11.8%). Patients with Crohn’s disease (CrD) had a higher rate of Clostridioides difficile infection (CDI) compared to those with ulcerative colitis (UC) (17.2% vs. 8.5%). Patients receiving biological therapies were at significantly higher risk of developing CDI compared to those not on biological therapy (17.9% vs. 6.9%, P = 0.042). Among patients hospitalized for flare-up symptoms, one-third were confirmed to have CDI. Overall, stool testing was positive in over 30% of cases, CDI and E. coli were the most common identified infections in pediatric patients with IBD presenting with exacerbating symptoms, highlighting the significance of routine pathogen testing, in patients presenting with symptoms of suggestive of flare. CDI was particularly more prevalent among patients with Crohn’s disease, those receiving biological therapy, and those hospitalized for their symptoms. Additionally, our findings highlighted the limited utility of traditional stool culture in detecting enteric infections.
Al-Shaibah K, Jasem R, Alsarhan A, Tzivinikos C
Ear, Nose, and Throat Manifestations in Inflammatory Bowel Diseases: A Systematic Review of the Clinical Spectrum.Systematic review Medicina (Kaunas, Lithuania) | 2026-05-12
Background: Inflammatory bowel disease (IBD), including ulcerative colitis (UC) and Crohn’s disease (CD), represents a chronic immune-mediated disorder frequently associated with extraintestinal manifestations. While musculoskeletal, dermatologic, and ocular complications are well recognized, ear, nose, and throat (ENT) involvement remains underrecognized despite its potential morbidity. Objective: To systematically evaluate the spectrum of ENT manifestations in IBD, focusing on clinical presentation, diagnostic approaches, and outcomes. Methods: A systematic literature search was conducted in PubMed and Scopus in accordance with PRISMA 2020 guidelines. Eligible studies included English-language human studies (2015-2026) reporting ENT manifestations in UC or CD. Following screening, 23 studies were included in the qualitative synthesis. Extracted data comprised study design, IBD subtype, patient demographics, ENT manifestations, diagnostic methods, and clinical outcomes. Results: The majority of studies consisted of case reports and small observational series. Sensorineural hearing loss (SNHL) was the most frequently reported manifestation in both adult and pediatric populations, with evidence suggesting immune-mediated mechanisms and variable responsiveness to corticosteroids. Nasal involvement included pyoderma gangrenosum, pyoderma vegetans, and aseptic nasal septal abscess, occasionally resulting in severe structural complications such as saddle-nose deformity. Laryngeal and airway involvement included dysphonia, tracheitis, and rare but potentially life-threatening inflammatory airway disease. Additional findings included associations with chronic rhinosinusitis. Diagnosis relied on audiometry, imaging, endoscopy, and histopathology. Systemic corticosteroids were frequently effective; however, delayed recognition may lead to irreversible sequelae. Conclusions: ENT manifestations in IBD constitute a clinically heterogeneous but important group of extraintestinal complications. Increased awareness of ENT manifestations may support earlier diagnosis and multidisciplinary management of IBD, potentially reducing irreversible complications.
Litsou E, Psychogios G, Saridi M, Katsanos KH, Fousekis F
Clinical Phenotypes and Genetic Findings in Very-Early-Onset Inflammatory Bowel Disease: A Vietnamese Pediatric Cohort Study. Children (Basel, Switzerland) | 2026-05-11
Background/Objectives: Very early onset inflammatory bowel disease (VEO-IBD), frequently associated with monogenic defects, is increasingly recognized worldwide but remains poorly characterized in Vietnam. This study aimed to characterize the clinical phenotypes and genetic spectrum of Vietnamese children with VEO-IBD. Methods: We conducted a retrospective cohort study at a tertiary pediatric referral center in Vietnam from July 2016 to January 2026. Clinical, laboratory, endoscopic, histopathological, genetic, and treatment data were systematically collected and analyzed. Monogenic variants were identified using next-generation sequencing and classified according to ACMG criteria. Results: Thirty-six children were included, with a median age at onset of 7.5 months, and 72.2% presenting before 24 months. Crohn’s disease predominated (72.2%). Disease burden was high, with growth impairment in 75.0% and anemia in 91.7%. Extraintestinal manifestations were frequent, particularly recurrent infections (72.2%), dermatitis (44.4%), and oral ulcers (44.4%). Perianal disease occurred in 58.3%, with early complications including perianal ulcer (44.4%), perianal abscess (30.6%) and fistulas (33.3%). Inflammatory markers were markedly elevated, and disease activity indices indicated moderate-to-severe disease at diagnosis. Genetic testing was performed in 91.7% of patients, identifying monogenic etiologies in 30.3%. Identified variants involved genes related to immune regulation (IL10RA/IL10RB, FOXP3, XIAP), autoinflammation (TNFAIP3), host defense (CYBB), and epithelial function (MYO5B). Conclusions: Monogenic etiologies account for a substantial proportion of VEO-IBD and are associated with distinct clinical phenotypes and therapeutic implications. Early integration of genomic testing with clinical phenotyping is essential to improve diagnostic precision and enable pathway-based treatment, supporting precision medicine in pediatric IBD.
Nguyen MC, Nguyen TVH, Nguyen L, Dang TH, Tran T, Nguyen TVA, Hoang NT, Nguyen NQL, Do TMP, Nguyen VT
Preliminary IL-1 Family Cytokine Signature for Crohn’s Disease Onset in Pediatric Juvenile Idiopathic Arthritis. International journal of molecular sciences | 2026-05-10
Crohn’s disease (CD) in children with juvenile idiopathic arthritis (JIA) is frequently diagnosed late due to overlapping symptoms and non-specific biomarkers. We hypothesized that longitudinal cytokine profiling could identify a pre-symptomatic signature predictive of CD conversion in pediatric JIA patients. Ninety pediatric participants (JIA, CD, psoriatic arthritis, healthy controls) underwent serum cytokine profiling (IL-1α, IL-1β, IL-36α, IL-37, IL-6, IL-18, IL-27, IL-31) at baseline and 12 months. Statistical analysis used Mann-Whitney U tests for two-group comparisons, the Kruskal-Wallis test with Dunn’s post hoc for multi-group comparisons, Fisher’s Exact Test for categorical outcomes, and exploratory principal component analysis (PCA). Baseline screening identified a subgroup of JIA patients (N = 4) with significantly elevated IL-1α, IL-1β, and IL-36α. At 12 months, all four patients in this subgroup received a secondary CD diagnosis (4/4 converters vs. 0/21 non-converters; Fisher’s Exact Test: p < 0.0001). The longitudinal analysis at conversion revealed a broader pro-inflammatory shift, with marked increases in IL-18 and IL-31, alongside elevated IL-37, suggesting a compensatory regulatory response. PCA confirmed that converters clustered distinctly from both stable JIA and established CD. A baseline IL-1 family signature may represent a preliminary predictive signature for CD onset in pediatric JIA. Although constrained by the small converter subgroup (N = 4), these data support cytokine profiling for earlier diagnosis in high-risk populations.
Polyanskaya AV, Soboleva AG, Mezentsev A, Sobolev VV, Chebysheva SN, Geppe NA, Zholobova ES, Osminina MK, Podzolkova VA, Shakhnazarova MD
Epidemiology & Outcomes (8 papers)
Epidemiology of diagnosed inflammatory bowel disease in Taiwan population from 2011 to 2021: a population-based study. BMC gastroenterology | 2026-05-29
Inflammatory bowel disease (IBD) has shown a steadily rising prevalence in Asian populations over recent decades, coinciding with rapid industrialization, Westernized dietary habits, and lifestyle changes. This study aimed to report the annual trends and sociodemographic-specific rates of the prevalence and incidence of diagnosed IBD in Taiwan from 2011 to 2021. A population-based study of all residents enrolled in the National Health Insurance (NHI) program, the Catastrophic Illness Patient Database, was conducted to identify patients diagnosed with IBD. The annual prevalence and incidence of diagnosed IBD were identified using International Classification of Diseases, Ninth and Tenth Revision, Clinical Modification (ICD-9-CM and ICD-10-CM) diagnostic codes, stratified by age, sex, insurance premium, and degree of urbanization. Logistic regression analyses were performed to estimate odds ratios for associated risk factors; while Joinpoint regression analyses were used to assess temporal trends in age-standardized annual prevalence and incidence from 2011 to 2021. The age-standardized annual prevalence of IBD more than doubled from 9.56 per 100,000 persons in 2011 to 19.54 per 100,000 in 2021 (annual percent change [APC]: 7.35%), while incidence rates rose from 0.89 to 2.46 per 100,000 persons over the same period (APC: 11.04%). Males consistently showed higher prevalence and incidence rates than females throughout the study period. Prevalence was highest among individuals aged 50-60 years, those with high income levels, and residents of highly urbanized areas, whereas incidence peaked in the 40-50-year age group and was also elevated among individuals with high income. Nationwide NHI data showed a substantial increase in IBD prevalence and incidence in Taiwan from 2011 to 2021, with a disproportionately increased burden among men, middle-aged individuals, high-income groups, and residents of highly urbanized areas.
Wu YH, Li TC, Li CI, Liu CS, Cho DY, Lin CH, Lin CC
IBD in transition: a decade of data from the Malaysian Kinta Valley cohort.★ Inflammatory bowel diseases | 2026-05-28
Inflammatory bowel disease (IBD) is emerging in the Asia-Pacific region including Malaysia. The aim of this study is to compare the current incidence and prevalence of IBD in Malaysia from the previous decade, as well as comparing the incidence rates between the urban and rural population. Kinta Valley was selected as the urban catchment area while Hilir Perak was selected for the rural catchment area within the same state. Patients newly diagnosed with IBD were prospectively recruited, and all confirmed IBD cases were included for the prevalence analysis. Baseline demographic information and disease characteristics were recorded. The crude incidence rates of IBD, ulcerative colitis (UC), Crohn disease (CD) and IBD unclassified (IBD-U) in Kinta Valley were 1.13, 0.45, 0.60, and 0.08 per 100 000 person-years, respectively, compared to 0.68, 0.46, and 0.20 per 100 000 person-years in 2013. The incidence of UC:CD was 0.75:1 compared to 2.3:1 from the previous study. The prevalence rates were 15.08, 10.13, 4.84, and 0.11 for IBD, CD, UC, and IBD-U per 100 000 population, respectively. The matching incidence rates in a nearby rural area were higher, at 3.29, 1.88, 1.41, and 0.47 per 100 000 person-years, respectively, but the overall incident cases were very low. Our findings suggest an increasing incidence of IBD in Malaysia, in keeping with the second stage of the global evolution of IBD. There is a potential shift in the relative incidence of CD compared to UC, but larger population studies are required for confirmation. The incidence of inflammatory bowel disease (IBD) in Malaysia has increased by 1.5 fold in just a decade, with a corresponding increase in prevalence rates. There is an apparent reversal in the ratio of ulcerative colitis (UC) to Crohn disease (CD), although this finding has to be interpreted with caution due to the small absolute numbers.
Hilmi I, Khoo XH, Kwong DY, Tan PO, Cheong SY, Skantha R, Chua ASB, Singh H, Ng TH, Kong WH
Mid- to Long-Term Outcomes of the MESOCOLIC Trial Evaluating Extensive Versus Limited Mesenteric Excision in Crohn’s Disease.★ Gastroenterology | 2026-05-27
Abstract not available.
Duan M, Zhang X, Liu W, Ke J, Zhou W, Li Y
The Prevalence of Fibromyalgia in the General Population and At-Risk Subpopulations: A Systematic Review and Meta-Analysis. Anesthesia and analgesia | 2026-05-27
Estimates of fibromyalgia prevalence vary widely worldwide due to differences in diagnostic criteria, study methodology, and population characteristics. Accurate estimates are essential to inform population-level surveillance, guide resource allocation, and highlight disparities in disease recognition and access to care. The objective of this systematic review and meta-analysis was to determine the global prevalence of fibromyalgia in the general population, and secondarily to identify factors moderating prevalence variation and to assess prevalence in defined at-risk subpopulations. Pooled prevalence estimates with 95% confidence intervals (CIs) were calculated using the inverse variance heterogeneity model with Freeman-Tukey transformation. Subgroup analyses were performed by sex, diagnostic criteria, country, and other study characteristics, and meta-regression assessed moderators including publication year and Human Development Index (HDI). Of 21,645 records identified, 1,728 underwent full-text review and 882 studies were included in the final analysis. Across 38 countries and 30,070,032 individuals (188 studies), the pooled fibromyalgia prevalence in the general population was 1.40% (95% CI, 0.49-2.47), with substantial heterogeneity (I2 = 100%) and very low certainty of evidence. Among at-risk subpopulations (9,771,123 participants; 768 studies), prevalence was markedly higher in autoimmune and inflammatory conditions, such as chronic urticaria (37.1%), interstitial cystitis (30.8%), systemic sclerosis (20.6%), celiac disease (20.5%), and inflammatory bowel disease (19.9%), and elevated in chronic pain, rheumatologic, and post-infection cohorts. Meta-regression identified publication year (β = 0.008, P < .001) and HDI (β = 0.725, P = .002) as significant moderators of prevalence. In conclusion, fibromyalgia affects 1% to 2% of the global population, with substantially higher rates in at-risk subpopulations. Temporal and socioeconomic trends emphasize diagnostic inconsistency and global disparities in care.
D’Souza RS, Klasova J, Morsi M, Vincent A, Mohabbat AB, Whitfield S, Radlicz C, Sheen S, Wang D, Zhitnitsky M
Berberine Improved the Therapeutic Efficacy of UC-MSCs for DSS-Induced Colitis via Aerobic Glycolysis. Phytotherapy research : PTR | 2026-05-24
The global prevalence of inflammatory bowel disease (IBD) continues increasing, but effective targeted treatments remain elusive. Recently, mesenchymal stem cells (MSCs) have emerged as a promising candidate for IBD treatment, with energy metabolism playing a critical role. Berberine (BBR), a natural extract from Berberidaceae plants, has been shown to modulate various cell functions by reprogramming metabolism in immune-related diseases. This study aims to investigate the influence of BBR on the therapeutic effectiveness of MSCs in colitis. Using the colitis mice model, we compared the therapeutic effects of BBR treated MSCs (MSCBBR) and untreated MSCs by evaluating colon length, Disease Activity Index, and histopathological change. Various methods were employed to detect the differences of MSCBBR and MSCs, including seahorse analysis for energy metabolism, RNA-seq and qPCR for gene transcription, western blotting for protein expression, flow cytometry for phenotypic analysis, and cytokine production. Our results revealed that BBR treatment activated the AMPK signaling pathway, upregulated the expression of glucose transporter 1 (GLUT1), and promoted aerobic glycolysis in MSCs. Comparing to MSCs, MSCBBR exhibited the increased expression of tumor necrosis factor-stimulated gene-6 (TSG-6), enhanced immunomodulatory function and superior therapeutic efficacy. Inhibition of either glycolysis or TSG-6 expression impaired the therapeutic effect of MSCBBR, while overexpression of GLUT1 or TSG-6 obviously improved the therapeutic efficacy of MSCs. BBR treatment improved the therapeutic effect of MSCs in colitis by promoting aerobic glycolysis, providing a safe new approach for optimizing MSCs-based therapy in IBD through reprogramming energy metabolism.
Wu M, Li C, Feng J, Guo X, Fang R, Lian Q, Zhang X, Ma J, Li Y, Xie S
Inflammatory Bowel Disease Is Associated With Persistent Functional Impairment and Increased Short- and Long-Term Complications Following Total Knee Arthroplasty. Orthopedic reviews | 2026-05-22
Inflammatory bowel disease (IBD) is increasingly prevalent, and more affected patients are undergoing total knee arthroplasty (TKA). However, the effect of comorbid IBD on short- and long-term postoperative outcomes after TKA remains incompletely defined, particularly for functional and implant-related complications. Existing TKA-specific literature has not clearly established whether this risk persists across multiple postoperative time points. We performed a retrospective cohort study using the TriNetX Research Network. Adults undergoing primary TKA were identified and stratified by IBD status. Propensity score matching (1:1) balanced demographics and comorbidities, yielding 6134 patients per cohort. Outcomes were assessed at 90 days, 6 months, 2 years, and 5 years and included infectious, thromboembolic, medical, functional, and implant-related complications. Risk ratios with 95% confidence intervals were calculated for each endpoint. Matched cohorts were followed longitudinally across four predefined postoperative intervals after surgery. Patients with IBD demonstrated significantly increased risks of sepsis, pulmonary embolism, acute kidney failure, and periprosthetic joint infection/deep surgical site infection as early as 90 days. Several risks persisted through 5 years, including thromboembolic events, ischemic stroke, fall risk, abnormal gait, and implant failure. At 5 years, revision TKA rates did not differ significantly between cohorts despite the greater complication burden observed in patients with IBD. Preoperative IBD was associated with sustained postoperative morbidity after TKA, spanning infectious, thromboembolic, functional, and implant-related domains. These findings support enhanced perioperative optimization, closer long-term surveillance, and targeted management strategies for this high-risk population.
Harhash T, Almaat A, Elnaggar A, Shafau AL, Jawich B, Hilo K, Abdalla O, Forbes T, Elnaggar A, Jaura F
Evaluation of the Anti-Inflammatory Activity of Selected Plant Extracts in an In Vitro Model of Inflammation Using LPS-Stimulated Macrophages. Biomedicines | 2026-05-21
Background: Inflammatory bowel disease (IBD), including Crohn’s disease (CD) and ulcerative colitis (UC), is a group of chronic gastrointestinal (GI) diseases with complex and multifactorial pathophysiology. The global prevalence of IBD is increasing, highlighting the need to develop new therapeutic approaches. Plant-derived extracts have recently gained prominence due to their anti-inflammatory properties. Methods: This study investigated: apricot leaves (ALE), peach leaves (PLE), black chokeberry fruit (BCHE), rosehip seeds (RSE), passion fruit seeds (PSE), and linden blossom (LBE) (all at the concentration 10-200 µg/mL) in RAW 264.7 mouse macrophages. Cytotoxicity was assessed using the neutral red uptake (NRU) assay, and anti-inflammatory activity was assessed using Griess assay in the lipopolysaccharide (LPS)-induced inflammation. Additionally, the mRNA expression levels of key inflammatory genes (interferon-γ (Ifn-γ), interleukin-6 (Il-6), nitric oxide synthase (Nos2), and tumor necrosis factor-α (Tnf-α)) were analyzed. Results: ALE and PLE exhibited minimal cytotoxicity and strong anti-inflammatory activity, reducing the expression of all analyzed genes. PSE demonstrated anti-inflammatory activity in the Griess assay, but did not alter mRNA expression. Conclusions: ALE and PLE exhibit promising anti-inflammatory properties and warrant further preclinical investigation. Comprehensive in vitro and in vivo studies are necessary to confirm these results.
Merecz K, Suska K, Biniszewska O, Hirsa M, Wojdyło A, Tarasiuk-Zawadzka A, Fichna J
A context-dependent METTL1-m7G-SLC7A11 axis links metabolic stress to epithelial fate in ulcerative colitis. International journal of biological sciences | 2026-05-11
Ulcerative colitis (UC) is characterized by chronic intestinal inflammation accompanied by epithelial barrier dysfunction and profound metabolic stress; however, how metabolic cues are integrated to determine epithelial cell fate remains incompletely understood. Here, we identify a context-dependent METTL1-m7G-SLC7A11 regulatory axis that links metabolic stress to intestinal epithelial outcomes during UC progression. By integrating analyses of human UC tissues, DSS-induced acute and chronic colitis mouse models, and mechanistic in vitro experiments, we demonstrate that METTL1 enhances N7-methylguanosine (m7G) modification of SLC7A11 mRNA, thereby stabilizing the transcript and sustaining SLC7A11 expression in inflammatory settings. Functionally, SLC7A11 exhibits glucose-dependent dual effects. Under glucose-replete conditions, SLC7A11 supports cystine uptake, glutathione synthesis, and redox homeostasis, protecting epithelial integrity and limiting inflammation. In contrast, under glucose deprivation-a characteristic feature of inflamed UC mucosa-persistent SLC7A11 activation induces disulfide stress, cytoskeletal collapse, and disulfidptosis-associated epithelial injury. In vivo, inhibition of the METTL1/m7G/SLC7A11 axis exacerbates chronic DSS-induced colitis but alleviates acute DSS-induced colitis, revealing a switch from adaptive to maladaptive signaling with escalating metabolic stress. Collectively, these findings establish the METTL1-m7G-SLC7A11 axis as a metabolic rheostat that integrates inflammatory cues and nutrient availability to determine epithelial cell fate in UC, highlighting the importance of stage- and context-specific therapeutic strategies.
Yang L, Sun Q, Jiang Z, Yao B, Yang C, Liu G, Yuan L
IBD-associated Neoplasia (6 papers)
Genomic Profiling of Cancerous Areas, Dysplasia, and Background Mucosa in Ulcerative Colitis-associated Colorectal Cancer. Anticancer research | 2026-06
Ulcerative colitis (UC) is associated with an increased risk of colorectal cancer (CRC), and unlike sporadic CRC, colitis-associated CRC (CAC) develops through a dysplasia-carcinoma sequence rather than the traditional adenoma-carcinoma pathway. However, studies that have simultaneously analyzed background mucosa, dysplasia, and carcinoma within the same patient remain limited. This study aimed to identify characteristic genetic abnormalities in UC-associated CRC by analyzing background mucosa, dysplasia, and carcinoma using a targeted gene panel. Herein, 12 cases of CAC were examined. Formalin-fixed paraffin-embedded samples from eight background mucosae, 12 dysplastic lesions, and 15 carcinoma lesions, together with matched blood samples as normal controls, were subjected to targeted gene panel analysis using the Todai OncoPanel. TP53 mutations were identified in two of the 12 dysplastic lesions (16.7%) and 12 of the 15 carcinoma lesions (80.0%). APC and KRAS, which are frequently mutated in sporadic CRC, were detected in one and two patients, respectively. Among the 12 cases analyzed, dysplasia and carcinoma from the same patient were available for comparison in 11 cases; of these, only one case harbored the pathogenic variants KRAS G12S and CHEK2 K373E, as well as the BRCA2 A1652S variant of uncertain significance. CAC exhibits distinct mutational characteristics compared with sporadic CRC and different genetic abnormalities in each lesion may contribute to the dysplasia-carcinoma sequence.
Funakoshi K, Sasaki K, Hata K, Nozawa H, Murono K, Emoto S, Yokoyama Y, Shinagawa T, Kohsaka S, Shinozaki-Ushiku A
Long-Term Outcomes After Endoscopic Resection for Strictly Defined Ulcerative Colitis-Associated Neoplasia: An Exploratory Retrospective Cohort Study. Digestive endoscopy : official journal of the Japan Gastroenterological Endoscopy Society | 2026-06
Ulcerative colitis (UC)-associated neoplasia (UCAN) carries a risk of metachronous development; however, risk stratification based on inflammatory origin remains unclear. This exploratory study aimed to classify UCAN arising in colitis-affected areas and to evaluate long-term outcomes after endoscopic resection (ER). We retrospectively analyzed the data of 102 patients with UC who underwent ER for colorectal neoplasia between 2004 and 2024. Lesions in colitis-affected areas were operationally classified as confirmed UCAN, based on non-polypoid morphology and characteristic p53 and Ki-67 immunostaining patterns, or as probable UCAN. Lesions in colitis-unaffected areas were classified as sporadic neoplasia (SN). Cumulative incidences of metachronous neoplasia and overall survival were estimated using the Kaplan-Meier method, and associations with metachronous confirmed UCAN were assessed using univariate Cox proportional hazards models. The median follow-up period was 4.3 years. Among 102 lesions, 13 were classified as confirmed UCAN, 68 as probable UCAN, and 21 as SN. The 5-year cumulative incidence of metachronous confirmed UCAN was significantly higher in the confirmed UCAN group (52%) than in the probable UCAN (4%) and SN (0%) groups (p < 0.01). Confirmed UCAN remained independently associated with metachronous confirmed UCAN (hazard ratio, 11.05; 95% confidence interval, 2.01-60.7; p < 0.01). Overall survival did not differ significantly among groups. Using an exploratory classification, confirmed UCAN was associated with an increased incidence of metachronous neoplasia after ER. These findings suggest that this subgroup may warrant closer surveillance; however, further validation is required.
Nishio M, Hirasawa K, Chiba S, Takeda Y, Tatsuno M, Nozaki K, Morohashi K, Kanemura T, Atsusaka R, Azuma D
Ferroptosis in colorectal cancer: Molecular mechanisms and regulatory crosstalk with therapeutic prospects (Review).Review Oncology reports | 2026-05-29
Colorectal cancer (CRC) is a common malignancy of the colonic and rectal epithelia. Numerous patients with CRC derive only limited and unsustained benefit from conventional chemotherapy or immunotherapy, underscoring the need for novel treatments. Ferroptosis is an iron‑dependent, lipid peroxidation‑driven form of regulated cell death, controlled by iron and lipid metabolism, as well as antioxidant defense pathways, which represent attractive therapeutic targets. Ferroptosis‑related genes are closely linked to immune status, and metabolic reprogramming within the tumor microenvironment can modulate immune cell activation and antitumor immunity. Induction of ferroptosis suppresses CRC proliferation and overcomes resistance to cytotoxic drugs, whereas inhibition of ferroptosis may alleviate inflammatory bowel disease and limit CRC initiation in specific settings. This review summarizes the molecular basis and immunological relevance of ferroptosis in CRC, and discusses recent advances in combination strategies involving chemotherapy, immunotherapy, gut microbiota‑based therapy and nanotherapy, as well as current clinical progress, potential biomarkers and translational challenges.
Wu M, Zhang M
Microplastic Exposure Aggravates Cardiomyopathy Under Hemodynamic Stress Through the Gut-Heart Axis. Circulation | 2026-05-28
Bisphenol F (BPF) is a common substitute for bisphenol A and the most prevalent bisphenol compound in diverse plastic manufacturing applications. However, the potential toxicity of BPF remains largely unexplored. This study investigates the effects of BPF on the cardiovascular system and intestinal barrier. Germ-free mouse models and fecal microbiota transplantation techniques were used to confirm the role of gut microbiota in BPF-induced cardiovascular injury. Untargeted metabolomics and spatial metabolomics were used to identify the in vivo metabolic products of BPF. Single-cell sequencing was used to identify which cardiac cell types were damaged by BPF exposure. BPF was detected in 90.5% of 285 human urine samples (median, 1.16 ng/μg creatinine). BPF exposure induced cardiomyocyte hypertrophy, cardiac dysfunction, and intestinal barrier damage, effects contingent on the presence of gut microbiota. Metabolomic analysis identified the microbial conversion of BPF to N-acetylputrescine (NAP). Mechanistically, we found that BPF stimulated intestinal epithelial cells to secrete spermidine/spermine N1-acetyltransferase 1 (Sat1), which catalyzed this conversion. Furthermore, NAP impaired the intestinal barrier by disrupting the Golgi-mitochondria axis and caused cardiac hypertrophy by activating the p53 pathway and inhibiting glycolysis in cardiomyocytes. Supplementation with Akkermansia muciniphila or its metabolite tryptophol mitigated BPF-induced cardiac and intestinal injuries by downregulating the Sat1-NAP axis. Clinical analysis further showed elevated serum NAP levels in patients with inflammatory bowel disease, positively correlating with cardiac injury markers. BPF disrupts intestinal barrier function through microbial metabolism involving the tryptophol/Sat1 pathway, leading to NAP production. NAP damages intestinal organelles and enters circulation, inducing cardiac p53 activation and hypertrophy. This study delineates a novel gut microbiota-Sat1-NAP pathway underlying BPF-induced cardiotoxicity, offering new insights for risk assessment and therapeutic intervention.
Wang J, Xu J, Mai H, Niu G, Wu S, Zhang X, Zhu J, Aschner M, Meng Q, Chen R
Trends in Colorectal Dysplasia in Patients with Inflammatory Bowel Disease. Diseases of the colon and rectum | 2026-05-25
Patients with inflammatory bowel disease face an elevated risk for early-onset colorectal cancer due to chronic inflammation and long-term immunosuppression. While immunotherapy improves disease control, its potential for increasing neoplastic transformation warrants further evaluation. To characterize trends in incidence and clinical factors associated with dysplasia among IBD patients undergoing surgery. This is a retrospective cohort study. High-volume United States IBD Centers participating in the American College of Surgeons National Surgery Quality Improvement Program IBD Collaborative, 2017-2023. Adults with IBD undergoing colorectal surgery. Patients with missing covariate or outcome data were excluded. Prevalence of dysplasia (low-grade, high-grade, or carcinoma) on surgical pathology and associated risk factors. Among 5,516 IBD patients, dysplasia was identified in 4.3%. Prevalence was higher in patients with ulcerative colitis compared to those with Crohn’s disease and indeterminate colitis (6.5% vs 3.2% vs 3.4%, respectively, p < 0.05), in those receiving immunotherapy (16.7% vs 12.0%, p = 0.02), and among Asian American patients (8.7% vs 4.5% White, 2.4% Black, p < 0.05). Female sex and older age (mean 53.9 vs 43.1 years) were also associated with increased dysplasia rates (p < 0.05). On multivariable logistic regression analysis, Asian American race (OR 2.54 [CI: 1.4-4.8]), immunotherapy use (OR 1.6 [CI: 1.1-2.3]) and ulcerative colitis (OR 2.0 [CI: 1.6-2.7]) were independently associated with dysplasia. A BMI <18.5 was inversely associated with risk (OR 0.4 [CI: 0.2-0.9]). Data capture is limited to 30 days postoperatively and does not account for surgical indication or dysplasia chronicity. In patients undergoing surgery for IBD, immunotherapy use, Asian American race, ulcerative colitis, and older age were independently associated with colorectal dysplasia. These findings highlight the importance of tailored surveillance strategies in at-risk populations, particularly those receiving long-term immunosuppressive therapy. See Video Abstract.
Newland JJ, Grunhut J, Belcher R, Lopez KE, Brown RF, Eisenstein S, Bafford AC
From inflammation to fibrosis and cancer: the emerging role of AIEC-derived metabolites in intestinal disease progression.Review Experimental & molecular medicine | 2026-05-19
The intestinal microbiota maintains mucosal homeostasis through dynamic host-microbe interactions. When this balance is disrupted, gut dysbiosis drives inappropriate immune activation, leading to dysregulated inflammation that contributes to the pathogenesis of chronic inflammatory diseases, including inflammatory bowel diseases (IBD). Chronic inflammation in patients with IBD increases the risk of intestinal fibrosis and colorectal cancer. However, therapeutic options for patients with IBD with fibrosis or neoplasia remain limited and challenging. Adherent-invasive Escherichia coli (AIEC) have emerged as key metabolic drivers of disease in IBD. We previously demonstrated that the AIEC-derived genotoxin colibactin and the siderophore yersiniabactin (Ybt) promote tumorigenesis through DNA damage and fibrosis via pro-fibrotic macrophage-fibroblast interactions, respectively. Because fibrosis and tumorigenesis involve overlapping pathways such as extracellular matrix remodeling, transforming growth factor-beta signaling, angiogenesis, and epithelial-to-mesenchymal transition, AIEC-derived metabolites may be functionally interconnected and could drive distinct pathological outcomes depending on the context of the disease. This Review highlights how AIEC-derived metabolites amplify inflammation, fibrosis, and neoplasia, outlines potential crosstalk between colibactin and Ybt, and discusses therapeutic opportunities targeting AIEC metabolite production in parallel with host-directed antifibrotic and cancer-prevention strategies.
Ahn JH, Hazelton A, Nguyen J, Arthur JC
AI & Machine Learning (5 papers)
Evolution of Gastrointestinal Inflammatory Diseases and Neoplasm Burden in Super-Elderly Populations: Integrated GBD 2023, CHARLS, and CLHLS Analyses of China and G20 Countries. Molecular medicine (Cambridge, Mass.) | 2026-05-26
Rapid population aging has profoundly altered the epidemiological profile of gastrointestinal diseases in individuals aged ≥75 years. Although enteric infections (EI) have been effectively controlled through public health interventions, the burden of gastrointestinal inflammatory diseases (GIID) and neoplasms (GIN) continues to evolve. Systematic comparisons of temporal trends, sex differences, and age-subgroup patterns between China and G20 nations remain limited. Using GBD 2023 data, we analyzed incident cases, age-standardized rates (ASR), and Disability-Adjusted Life Years (DALYs) of EI, GIID, and GIN among individuals aged ≥75 years in China and 19 G20 countries from 1990 to 2023. Log-linear regression was used to estimate the average annual percentage change (AAPC) in ASR, stratified by sex and 5-year age groups. Complementary individual-level analyses included an XGBoost machine-learning model with SHAP interpretability and disease co-occurrence network analysis. In China, EI ASIR declined sharply (AAPC = -2.24%), while G20 countries showed an upward trend (AAPC = +0.65%). GIID ASIR remained essentially stable in China but rose significantly for Crohn’s disease, Inflammatory Bowel Disease (IBD), and ulcerative colitis; G20 countries exhibited an overall decline. GIN shifted toward metabolism-related tumors in China (Colon and rectum cancer AAPC = +1.29%, pancreatic cancer AAPC = +0.74%), whereas esophageal and gastric cancer burdens decreased. China Health and Retirement Longitudinal Study (CHARLS) analysis identified the frailty index as the dominant predictor with clear non-linear threshold effects.Chinese Longitudinal Healthy Longevity Survey (CLHLS) networks revealed arthritis and rheumatic diseases as central hubs strongly linked to digestive disorders, highlighting chronic inflammation as the core driver of multimorbidity. This study integrates GBD population trends with CHARLS and CLHLS cohort data to characterize the evolving gastrointestinal disease burden in China’s super-elderly population.
Wu KJ, Peng W, Li JC, Li JJ, Qin DY, He RQ, Xiong KH, Ling JW, Li H, Chen G
Structure-based machine learning model for discovering pregnane X receptor (PXR) agonists and biological activity validation. Archives of toxicology | 2026-05-25
Pregnane X receptor (PXR), a nuclear receptor superfamily member, maintains bile acid homeostasis by regulating metabolic enzymes [e.g., cytochrome P450 3A4 (CYP3A4), uridine diphosphate glucuronosyltransferase 1A1 (UGT1A1)] and multidrug resistance protein 1 transporter, and alleviates liver/intestinal inflammation via inhibiting the nuclear factor kappa-B pathway, serving as a critical therapeutic target for cholestatic liver diseases and inflammatory bowel disease. In this study, we established a novel structure-based machine learning strategy to identify PXR agonists from a natural product database. With generated bioactive conformations binding with PXR, we integrated ligand-based and structure-based features to construct a comprehensive machine learning model using light gradient boosting machine. This model illustrated an R2 of 0.874 for the internal validation set and an R2 of 0.845 for the external test set, superior to the performance of other machine learning models, e.g. random forest regression, support vector regression, gradient boosting regression, K-nearest neighbors, and extreme gradient boosting. The model was used to predict the PXR agonistic activity of the candidate molecules screened out by the pharmacophore model. Promising candidates were selected out for further assay with HepG2 cell culture combined with a dual-luciferase reporter. Ultimately, natural products like schisantherin A, rhynchophylline, and irigenin were identified as potent PXR agonists, with half-maximal effective concentrations (EC50) of 1.58 μM, 2.57 μM, and 20.67 μM, respectively. These PXR agonists act as potential candidates for targeted therapies against PXR-related diseases. We anticipate that this work will provide support for the design and discovery of PXR modulators.
Huang FF, Luo Y, Chen H, Meng YH, Li W, Liang H, Ai CZ
Healthcare Providers’ Perspectives on the Role of Artificial Intelligence in the Care of Patients with Inflammatory Bowel Disease: An International Survey. Digestive diseases and sciences | 2026-05-24
Artificial intelligence (AI) is transforming inflammatory bowel disease (IBD) care, but concerns over data quality, privacy, and provider familiarity remain. To examine international health care providers’ (HCPs) perceptions, clinical use of, and barriers to applying AI in IBD care. An anonymous 17-item survey was developed and pretested by an international team. The survey was fielded internationally from January to May 2025 via social media, international IBD newsletters and email listservs. Of 323 IBD professionals from North America (35.3%), Europe (26.0%), Asia-Pacific (19.2%), 207 (64.1%) viewed AI as very or extremely promising. AI-assisted endoscopy was reportedly adopted by 131 (40.6%) of respondents, but only 69 (21.4%) reported applying AI in IBD care or research. Males supported AI in IBD endoscopic scoring (89.9% vs. 79.1%, p = 0.009) and radiomics more than females (86.6% vs. 75.2%, p = 0.022), while females endorsed AI for patient education more than males (81.5% vs. 70.6%, p = 0.026). 145 (44.9%) respondents were concerned about AI usage in IBD care. Females were less concerned about cost (18.5% vs. 30.1%, p = 0.019) and more concerned about oversight (28.7% vs. 14.7%, p = 0.003). Concerns regarding AI usage decreased with age (OR 0.021 for age > 55 compared to age 25-34 years old; 95% CI 0.13-0.84). Exposure to IBD-focused AI-based tools was associated with more favorable perceptions of AI use in IBD care (OR 2.63, 95% CI 1.25-5.53). Based upon survey results, HCPs had concerns over insufficient education, regulatory ambiguity, and perplexing implementation strategies for AI. Proven clinical benefit (74.9%) and adequate AI training (72.1%) are the top solutions for enabling the appropriate adoption of AI tools in IBD.
Devi J, Colbert CY, Dar SH, Gros B, Ardabili AR, Ho AHY, Misra-Hebert AD, Sleiman J
Integrative Transcriptomic Analysis Identifies Shared Immune-Fibrotic Transcriptional Programs Across Crohn’s Disease and Idiopathic Pulmonary Fibrosis. International journal of molecular sciences | 2026-05-15
Idiopathic pulmonary fibrosis (IPF) and Crohn’s disease (CD) share overlapping immune and fibrotic processes, yet their convergent molecular mechanisms remain poorly defined. Here, we performed an integrative transcriptomic analysis of nine public datasets to identify shared transcriptional signatures across IPF and CD. The main discovery and validation analyses were based on bulk transcriptomic datasets and combined differential expression profiling, weighted gene co-expression network analysis, and machine-learning-based feature prioritization. We identified 28 shared disease-associated module genes, from which three core genes-ZNF395, EEF2K, and BAHD1-were prioritized based on reproducibility and biological consistency. Functional enrichment analysis revealed their involvement in immune regulation, protein homeostasis, and stress-response pathways. Immune deconvolution and supportive single-cell RNA-sequencing further suggested associations between these genes and T-cell and myeloid cell populations, suggesting coordinated immune-fibrotic regulation. Experimental validation in a repetitive bleomycin challenge model and TGF-β1-stimulated fibroblasts showed consistent downregulation of these genes during fibrotic remodeling, supporting their association with fibrosis-related transcriptional states. Collectively, our study identifies conserved immune-fibrotic transcriptional programs shared across intestinal inflammation and pulmonary fibrosis, providing a hypothesis-generating molecular framework for understanding extraintestinal pulmonary involvement in Crohn’s disease and prioritizing candidate genes for future mechanistic investigation.
Luo R, Zhang Q, Fan Q, Chen Q, Nie Z, Dan L, Luo F, Cao Y, Xie S
Dietary polysaccharides in the management of inflammatory bowel disease: recent advances.Review Frontiers in nutrition | 2026-05-11
The increasing global burden of inflammatory bowel disease (IBD) has renewed awareness of the limitations and adverse effects of conventional pharmacotherapies, highlighting the need for safe, naturally derived, and mechanistically precise interventions. This review summarizes current understanding of IBD pathogenesis and the biological activities of dietary polysaccharides, with particular emphasis on their diverse protective functions in the gut. Robust preclinical evidence indicates that dietary polysaccharides can markedly alleviate colitis through multiple, interconnected mechanisms. These include reshaping the gut microbial ecosystem and its metabolites-such as short-chain fatty acids, tryptophan-derived indoles, and bile acids-restoring both the mechanical and chemical components of the intestinal barrier, and remodeling cytokine networks while rebalancing key immune cell subsets, including Th17/Treg and M1/M2 macrophages. In parallel, dietary polysaccharides modulate critical inflammatory signaling pathways, notably nuclear factor kappa-B (NF-κB), mitogen-activated protein kinase (MAPK), and NOD-like receptor protein 3 (NLRP3) inflammasome, thereby suppressing excessive intestinal inflammatory activity. Despite these promising experimental findings, clinical evidence remains limited, and important questions regarding structure-activity relationships, in vivo metabolic fate, and long-term safety and efficacy in patients with IBD have yet to be fully addressed. Future research should integrate emerging technologies such as nanotechnology and artificial intelligence to dissect molecular mechanisms in greater depth and to guide the rational design of polysaccharide-based therapeutics, dietary supplements, and functional foods tailored to individual patient profiles, thereby advancing precision nutrition strategies for IBD management.
Yang S, Wu J, Xiang J, Wang M, Shen P, He L
Endoscopy & Imaging (non-IUS) (5 papers)
Chishizhi Yuyuliang Decoction Ameliorates Ulcerative Colitis in Mice by Promoting Colonic Epithelial Mucosal Healing via the CAV1/FA Axis. Rapid communications in mass spectrometry : RCM | 2026-08
This study aimed to investigate the therapeutic mechanisms of CY in treating UC using an integrated metabolomics and proteomics approach. A murine UC model was induced using dextran sulfate sodium (DSS). The therapeutic efficacy of CY was evaluated via histological examination (H&E staining) of colon tissues to assess inflammation, epithelial necrosis, and crypt abscesses. Serum and colon tissues were collected for ELISA, immunofluorescence, Western blotting, metabolomics, and proteomics analyses. Additionally, an in vitro intestinal epithelial barrier model was established using LPS-induced Caco-2 cells. Cell viability, barrier function (TEER and FITC-Dextran permeability), cell damage (LDH), and inflammatory cytokine levels (IL-6 and IL-1β) were measured. The expression and distribution of tight junction proteins (ZO-1 and occludin) and signaling proteins (FAK, p-FAK, paxillin, and p-paxillin) were analyzed via immunofluorescence and Western blotting. CY treatment significantly reduced the Disease Activity Index (DAI) and suppressed the levels of pro-inflammatory cytokines (IL-6, IL-1β, and TNF-α) in UC mice. Proteomic analysis identified Caveolin-1 (CAV1) and the focal adhesion pathway as key therapeutic targets and signaling pathways. Metabolomic profiling revealed 17 endogenous metabolites, highlighting tryptophan metabolism and butyrate metabolism as critical pathways. Furthermore, CY intervention modulated arachidonic acid and linoleic acid metabolism. Mechanistically, CY upregulated the expression of CAV1 and FAK while downregulating AKT and paxillin phosphorylation. In vitro experiments demonstrated that CY-containing serum restored the barrier function of LPS-induced Caco-2 cells by regulating FAK/paxillin phosphorylation, upregulating tight junction proteins, and mitigating inflammatory responses. CY involvement in colonic mucosal healing attenuates inflammation and enhances intestinal barrier function in DSS-induced colitis, likely through the modulation of the CAV1/FA axis. These findings provide a theoretical basis for the clinical application of CY and offer novel insights for the development of therapeutic agents for UC.
Hong X, Wen Y, Xiao B, Jiang Q, Chen M, Chen P, Qian R, Wang Q, Li J, Huang F
Association Between Toothbrushing Habits and Mucosal Healing in Japanese Patients with Ulcerative Colitis. Digestive diseases and sciences | 2026-05-28
Evidence regarding the association between oral environment and the inflammatory bowel disease (IBD), including ulcerative colitis (UC), exists. However, evidence regarding the association between oral health parameters and disease activity of UC is limited. This study aimed to evaluate the association between remaining tooth number and toothbrushing frequency and mucosal healing (MH) in Japanese UC patients. The study included 275 patients with UC. Information on lifestyle and oral health parameters was collected via self-administered questionnaires. The definition of MH was based on the Mayo endoscopic subscore (MES) of 0. The prevalence of MH in this cohort was 24.7%. The distribution of remaining teeth was as follows: 13.1% had 20 or fewer teeth, 32.7% had 20-27 teeth, and 54.2% had 28 teeth. Toothbrushing frequency was 23.6% brushed once or less per day, 46.9% brushed twice per day, and 29.5% brushed three or more times per day. No significant difference was observed between remaining teeth and MH. However, toothbrushing frequency is independently positively associated with MH (adjusted odds ratio: 2.87 [95% CI: 1.19-7.29]; p value for trend = 0.021). Toothbrushing frequency but not the remaining tooth number might be independently and positively associated with MH in Japanese patients with UC.
Yagi S, Furukawa S, Miyake T, Yoshida O, Tange K, Kitahata S, Ninomiya T, Hanayama M, Suzuki S, Shibata N
EFFICACY OF WATER INFUSION VERSUS AIR/CO2 INSUFFLATION FOR COLONOSCOPY: A SYSTEMATIC REVIEW AND META-ANALYSIS.Meta-analysis Arquivos de gastroenterologia | 2026-05-25
Colonoscopy is a widely used screening method for colorectal cancer, playing a crucial role in early detection and prevention by allowing visualization and removal of precancerous lesions. It also helps diagnose and manage neoplastic lesions and inflammatory bowel disease by providing direct visualization of the intestinal mucosa. However, traditional air or carbon dioxide (CO2) insufflation may limit complete visualization of the colon. Alternatively, water infusion causes local distension without elongating the colon (unlike air insufflation), while warm water reduces spasms, decreasing insertion time and patient discomfort. This systematic review and meta-analysis aimed to compare water infusion versus air/CO2 insufflation in terms of technical efficacy, evaluate the effect of water immersion on procedural difficulty, and determine the accuracy of water immersion colonoscopy in detecting colon adenomas. We searched MEDLINE, EMBASE, and Cochrane CENTRAL databases for randomized controlled trials published from inception to January 2023. Outcomes included adenoma detection rate, success rate of cecal intubation, cecal intubation time, total procedure time (from insertion to withdrawal), need for abdominal compression, and on-demand sedation rate. Thirty randomized controlled trials were included. adenoma detection rate, success rate of cecal intubation, cecal intubation time, and total procedure time showed no significant difference between the two methods (P>0.05). However, water infusion significantly reduced the proportion of participants requiring on-demand sedation (risk ratio 0.61, 95%CI 0.48-0.77, P=0.02) and abdominal compression (risk ratio 0.65, 95%CI 0.51-0.83, P<0.01). Colonoscopy with water infusion helps the colonoscope reach the cecum more easily, decreasing the need for on-demand sedation and abdominal compression. A colonoscopia é um método amplamente utilizado para detecção de câncer colorretal, desempenhando um papel essencial na prevenção e detecção precoce por meio da visualização e remoção de lesões pré-malignas. Além disso, esse método auxilia no diagnóstico e tratamento de lesões neoplásicas e doenças inflamatórias intestinais, proporcionando visualização direta da mucosa intestinal. No entanto, o uso de ar ou dióxido de carbono (CO2) pode limitar a visualização completa do cólon. Uma alternativa seria o uso de infusão de água, que produz distensão local sem alongamento do cólon (ao contrário da insuflação de ar), uma vez que a água morna minimiza os espasmos, reduzindo o tempo de inserção e o desconforto do paciente. Esta revisão sistemática e metanálise busca comparar a infusão de água com a insuflação de ar/CO2 no que se refere à eficácia técnica, além de avaliar o impacto da imersão em água na dificuldade do procedimento e determinar a precisão da colonoscopia por imersão em água na detecção de adenomas colorretais. A busca foi realizada nas bases de dados MEDLINE, EMBASE, PubMed e Cochrane CENTRAL a fim de localizar ensaios clínicos randomizados publicados desde seu início até janeiro de 2023. Os desfechos incluíram a taxa de detecção de adenoma, a taxa de intubação cecal bem-sucedida, o tempo de intubação cecal, o tempo total de procedimento (tempo desde a inserção até a retirada), a necessidade de compressão abdominal e a taxa de sedação sob demanda. Trinta ensaios clínicos randomizados foram incluídos. A taxa de detecção de adenoma, a taxa de intubação cecal bem-sucedida, o tempo de intubação cecal e o tempo total de procedimento não mostraram diferença significativa entre os dois métodos (P>0,05). No entanto, a infusão de água reduziu significativamente a proporção de participantes que necessitaram de sedação sob demanda (razão de riscos 0,61, IC95% 0,48-0,77, P=0,02) e compressão abdominal (razão de riscos 0,65, IC95% 0,51-0,83, P<0,01). A infusão de água facilita a inserção do colonoscópio no ceco, reduzindo a necessidade de sedação sob demanda e de compressão abdominal.
Rodriguez-Guzman F, Arman ACO, Dias MMF, Paternostro D, Figueiredo-Zwetkoff BH, Micelli-Neto O, Ardengh JC
Personalized Risk Stratification of Residual Histologic Activity in IBD Using Circulating Cytokines. Journal of personalized medicine | 2026-05-21
Background: Persistent histologic inflammation may remain present in patients with inflammatory bowel disease (IBD) despite endoscopic remission. This study evaluated a clinically interpretable cytokine-based framework for risk stratification of residual histologic activity. Methods: In this prospective cohort study, 59 patients with IBD undergoing colonoscopy were included. Primary analyses were restricted to patients with ulcerative colitis (UC) in endoscopic remission (n = 31). Histologic activity was assessed using the Geboes score. Serum interleukin-10 (IL-10), interleukin-23 (IL-23), and C-reactive protein (CRP) were measured prior to endoscopy. Receiver operating characteristic (ROC) analysis and ROC-derived thresholds were used to evaluate biomarker performance and construct a cytokine-based risk stratification framework. Results: Among patients with UC in endoscopic remission, 14/31 (45.2%) demonstrated persistent histologic activity. IL-10 showed the strongest discriminatory performance for histologic activity (AUC 0.850), with a threshold < 3.9 pg/mL associated with sensitivity of 84.6% and specificity of 77.8%. Similar performance was observed using raw assay-reported IL-10 values (AUC 0.906). IL-23 showed limited overall discrimination (AUC 0.615). A combined IL-10/IL-23 framework stratified patients into progressively higher-risk subgroups, with histologic activity observed in 1/14 patients (7.1%) in the low-risk subgroup, 1/2 patients (50.0%) in the Intermediate A subgroup, 9/12 patients (75.0%) in the Intermediate B subgroup, and 3/3 patients (100%) in the high-risk subgroup (p < 0.001), although estimates for smaller subgroups should be interpreted cautiously. Reduced IL-10 levels were independently associated with histologic activity, whereas IL-23 primarily refined subgroup classification without substantially improving discrimination. Conclusions: An exploratory cytokine-based framework incorporating IL-10 and IL-23 may support risk stratification of residual histologic activity in UC during endoscopic remission. Larger multicenter studies are required to validate these findings and define their clinical utility.
Martinos N, Kroupis C, Stamouli M, Lazaris AC, Thomopoulou GE
Systemic Cytokine Patterns and Histologic Disease Spectrum in Inflammatory Bowel Disease. Current issues in molecular biology | 2026-05-15
Histologic mucosal healing is an increasingly recognized therapeutic target in inflammatory bowel disease (IBD), yet reliable non-invasive correlates remain limited. This study aimed to evaluate circulating cytokine patterns as detectability-based immune signals across the spectrum of histologic disease activity. In this prospective cross-sectional study, 59 patients with IBD and 36 healthy controls were enrolled. Serum interleukin-10 (IL-10) and interleukin-23 (IL-23) were quantified by ELISA. Histologic activity was graded using the Geboes score. Associations were assessed using non-parametric methods and multivariable logistic regression with Firth penalization. IL-10 demonstrated apparent separation across histologic states, primarily driven by reduced detectability in active inflammation, and was inversely associated with histologic severity. IL-10 remained associated with histologic status, although estimates should be interpreted cautiously. Detectable IL-23 was confined to moderate-to-severe inflammation and did not show graded discrimination, with interpretation limited by the small number of detectable observations. IL-10 and IL-23 exhibit complementary patterns, reflecting detectability-based regulatory signaling and a severity-dependent inflammatory threshold, respectively, without evidence of independent clinical utility for IL-23 in the present dataset. These findings are exploratory and require validation in larger prospective cohorts.
Martinos N, Kroupis C, Gypari M, Kranidiotis G, Karakoidas C, Konstantinou M, Lazaris AC, Thomopoulou GE
Genetics & Genomics (5 papers)
Exploring causal associations between autoimmune diseases and hearing loss: a mendelian randomization study. Brazilian journal of otorhinolaryngology | 2026-05-28
The causal relationship between Autoimmune Diseases (ADs) and Hearing Loss (HL) remains unclear. This study investigates whether genetic predispositions associated with ADs contribute to HL risk. Mendelian Randomization (MR) analysis was conducted to explore the causal effects of ADs on HL. SNPs from Genome-Wide Association Studies (GWAS) were used as instrumental variables for ADs, including Rheumatoid Arthritis (RA), Type 1 Diabetes (T1D), Systemic Lupus Erythematosus (SLE), Sjögren’s Syndrome (SS), Ankylosing Spondylitis (AS), Multiple Sclerosis (MS), Crohn’s Disease (CD), and Ulcerative Colitis (UC). Outcome data included Sensorineural Hearing Loss (SNHL), Conductive Hearing Loss (CHL), Mixed conductive and sensorineural Hearing Loss (MHL), and Sudden Idiopathic Hearing Loss (SIHL). MR analyses employed Inverse Variance Weighted (IVW) as the primary method, supplemented with MR-Egger, weighted median, and weighted mode. Heterogeneity, pleiotropy, and sensitivity were evaluated using Cochran’s Q test, MR-Egger regression, MR-PRESSO, and leave-one-out analysis. The IVW method identified nine significant associations: MS-SIHL (OR = 1.0494, 95% CI 1.0072-1.0934), AS-CHL (OR = 1.2832, 95% CI 1.0643-1.5472), AS-MHL (OR = 1.5994, 95% CI 1.3696-1.8678), AS-SNHL (OR = 1.1903, 95% CI 1.1104-1.276), AS-SIHL (OR = 1.481, 95% CI 1.22-1.798), SLE-CHL (OR = 1.0593, 95% CI 1.0116-1.1092), UC-MHL (OR = 1.0907, 95% CI 1.0027-1.1865), CD-CHL (OR = 1.0529, 95%CI: 1.0074-1.1005), and CD-SIHL (OR = 1.0597, 95% CI 1.0177-1.1034). Among these, outliers were detected only in AS-SNHL. After outlier removal, the AS-SNHL association remained significant (OR = 1.1722, p < 0.00001), with resolved heterogeneity and pleiotropy. No heterogeneity and pleiotropy were found for the other associations. This study identified nine significant AD-HL associations, emphasizing the need for targeted screening and management of HL in individuals with AD. Level 5.
Huang Y, Gao S, Luo R
IL23R genetic variants associate with Crohn’s disease risk and microbiome changes in healthy first-degree relatives.★ Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association | 2026-05-27
Single nucleotide polymorphisms (SNPs) in the Interleukin-23 receptor (IL23-R) gene are associated with Crohn’s disease (CD), suggesting a role in pathogenesis and several biologic agents targeting this pathway are now established therapies. IL-23 has been suggested to be involved in regulation of intestinal barrier function and may impact gut microbial composition. We investigated whether IL23-R genetic variants predict CD risk and influence gut barrier function and microbiome composition in healthy first-degree relatives (FDRs). 3,055 healthy FDRs with genotypic data from the Genetic Environmental Microbial (CCC-GEM) cohort were included. A weighted IL23R genetic risk score (IL23R-GRS) was generated from seven CD-associated IL23R SNPs and dichotomized as High (top quintile) vs. Low IL23R-GRS. A subset of this cohort was assessed for intestinal permeability (n=1,698) and microbiome profiling (n=2,523). Cox proportional-hazards models evaluated CD onset risk. High IL23R-GRS was associated with increased CD risk (hazard ratio 1.67, 95% confidence interval 1.01-2.75, p=0.044). This association remained significant after adjusting for fecal calprotectin, indicating genetic risk independent of subclinical inflammation. High IL23R-GRS was not associated with intestinal permeability (p=0.84) but was associated with differences in 15 genera, including decreased Faecalibacterium and increased Akkermansia (q<0.1). High IL23R-GRS was associated with increased CD risk in healthy FDRs and was associated with microbial differences, but not with intestinal permeability. These findings suggest potential clinical applications for IL23R-GRS in identifying high-risk individuals who may benefit from closer monitoring or future IL-23 pathway-targeted preventive interventions.
Leibovitzh H, Neustaeter A, Lee SH, Xue M, Espin-Garcia O, Olivera PA, Huynh HQ, Griffiths AM, Turner D, Madsen KL
Gastrointestinal-specific Anxiety in IBD: Associations with Disease Activity, Psychological Symptoms, and Serotonergic Polymorphisms. Biopsychosocial science and medicine | 2026-05-26
Many people living with an inflammatory bowel disease (IBD) experience persistent abdominal symptoms even in the absence of active inflammation. These symptoms are referred to as irritable bowel syndrome (IBS)-like symptoms. Gastrointestinal-specific anxiety (GSA) is a common feature of disorders of gut-brain interaction and may also be relevant in patients with IBD experiencing IBS-like symptoms. This cross-sectional study examined the associations between psychological variables and GSA in individuals with IBD in different states of disease activity (n=308, age: 42.4±19.4; female: 183, male: 125). In two subsamples of 83 patients (age: 41.2±15.9; female: 37, male: 46) and 70 patients (age: 42.1±16.1; female: 32, male: 38), links to single-nucleotide polymorphisms (SNPs) in genes related to serotonin signaling and serum tryptophan metabolites, respectively, were explored. Psychological variables including anxiety (β=.393, P<.001) and depression (β=.284, P<.001) predicted GSA levels. Genetic analyses revealed associations for serotonergic variants; however, none of these associations remained statistically significant after correction for multiple testing. While disease activity was linked to GSA (β=.171, P=.002), inflammatory biomarkers and tryptophan metabolites did not exhibit any significant associations. Our findings suggest that GSA as a specific type of anxiety is strongly related to psychological symptoms in IBD. Anxiety was the strongest predictor of GSA, contributing even more strongly to GSA than disease activity. Screening patients for GSA could help to detect disturbances in gut-brain-interactions and improve individualized treatment.
Atanasova K, Mellein S, Knoedler LL, Niehaus VD, Mirkhan H, Thomann PA, Lis S, Ebert MPA, Reindl W, Thomann AK
Epidermal Growth Factor Receptor Pathway Is a Potential Biological Mechanism in Inflammatory Bowel Disease-Induced Psoriasis. Journal of gastroenterology and hepatology | 2026-05-24
Psoriasis and inflammatory bowel disease are characterized by relapsing episodes of immune-mediated, chronic inflammation and frequently co-occur. However, the potential causal relationship between these two conditions and their shared pathogenesis remains unclear. We aimed to explore the pathogenesis and association between psoriasis and inflammatory bowel disease. We performed longitudinal cohort analyses using the UK Biobank and additionally incorporated three independent external datasets-the International IBD Genetics Consortium GWAS dataset, the FinnGen psoriasis GWAS dataset, and the plasma proteome dataset reported by Sun et al. to conduct Mendelian randomization and proteomic mediation analyses, thereby investigating the association between inflammatory bowel disease and psoriasis and exploring potential underlying mechanisms. Inflammatory bowel disease increased psoriasis risk in the UK Biobank cohort, as indicated by the Cox model and Mendelian randomization analysis. Smoking, body mass index, and air pollution were identified as risk factors for psoriasis in inflammatory bowel disease patients. In addition, multiple intermediary proteins and their activation pathways were implicated. The epidermal growth factor receptor substrate 15-like 1 was demonstrated as a mediating protein for Crohn’s disease and ulcerative colitis in the incidence of psoriasis. Enrichment analysis indicated that the downregulation and signaling of the epidermal growth factor receptor were potential biological mechanisms contributing to the causal relationships between genetic effects and the development of psoriasis and inflammatory bowel disease. The epidermal growth factor receptor pathway is a potential mechanism in inflammatory bowel disease-induced psoriasis. This study may inform the clinical management of psoriasis and inflammatory bowel disease.
Tao K, Sun H, Li F, Chang Y, Tang T, Xu H
Exome sequencing directly implicates 68 genes in inflammatory bowel disease. medRxiv : the preprint server for health sciences | 2026-05-20
Inflammatory bowel disease (IBD) is a chronic immune-mediated disorder of the gastrointestinal tract whose genetic basis is only partly resolved because most risk variants identified by genome-wide association studies (GWAS) lie in non-coding regions, limiting direct gene assignment and biological interpretation1,2. Here we analysed whole-exome and whole-genome sequencing data from 86,213 IBD cases and 478,363 controls of European ancestry. We identified 68 IBD genes directly implicated by conditionally independent protein-coding associations across the allele frequency spectrum. Many newly implicated IBD genes are supported by orthogonal genomic or pleiotropic evidence, pointing to disease-related pathways and nominating targets with therapeutic relevance. We further identified allelic series and non-additive effects at key loci such as NOD2 and TYK2. These results show that large-scale sequencing can resolve disease genes and pathways that remain ambiguous from non-coding association alone, providing a more direct route from human genetics to biological insight and therapeutic hypotheses.
Zhu R, Zhang Q, Yuan K, Zhang R, Turvey AK, Stevens CR, Fachal L, Ahmad T, Bel Kok K, Bernstein CN
Guidelines & Consensus (5 papers)
Shared challenges in the management of difficult-to-treat chronic inflammatory diseases: expert perspectives.Review Expert opinion on biological therapy | 2026-05-27
The concept of difficult-to-treat (D2T)/difficult-to-manage (DTM) disease was first defined in rheumatoid arthritis (RA). Recent definitions for axial spondyloarthritis (axSpA) and psoriatic arthritis (PsA) combine non-response to treatment including targeted and biologic treatment, inflammatory disease activity, and patient symptoms. This concept could apply to other chronic inflammatory diseases such as psoriasis (PsO) and inflammatory bowel disease (IBD). A consensus definition of D2T IBD is available but is yet to be fully articulated in PsO. This article aims to provide an expert overview of the shared elements and potential differences between the definitions and concepts of D2T/D2M in these diseases. D2T/D2M definitions should allow better evaluation of refractory diseases, accurate determination of disease severity, and effective treatment of the D2T areas or domains. Definitions should consider response to previous lines of treatment, control of inflammation, and global disease improvement, and consider the impact of D2T disease on patient status/quality of life. Proof-of-concept studies need to assess the current and future definitions of D2T/D2M populations in axSpA, PsA, PsO, and IBD, to accurately determine the prevalence of patients meeting each of those D2T criteria sets, and to identify risk factors, disease burden, and appropriate management strategies. Difficult-to-treat (D2T) and difficult-to-manage (D2M) disease refers to a disease state where some symptoms persist, with or without detectable inflammation, despite treatment. Patients and physicians consider these diseases problematic to manage. Definitions of D2T/D2M diseases in rheumatic diseases include rheumatoid arthritis (RA), axial spondyloarthritis (axSpA), and psoriatic arthritis (PsA). These definitions are a combination of non-response to treatment (including targeted and biologic treatment), persistent inflammation, patient’s symptoms and dissatisfaction. Other inflammatory diseases are also appropriate for defining D2T/D2M states. These include inflammatory bowel disease (IBD) where a definition has recently been proposed, and psoriasis (PsO). Identifying patients with uncontrolled states of disease such as D2T/D2M states is important, because these diseases may continue to impact quality of life and progressively damage the organs. Clinicians need to be able to accurately define and recognize D2T/D2M states in each type of chronic inflammatory condition. This article provides an expert overview of the current existing definitions, and a discussion of what further information is needed so that physicians can accurately determine which patients fit into each D2T/D2M criteria, their risk factors and disease burden, to guide management strategies for these patients.
Gossec L, Marotte H, Reguiai Z, Hébuterne X, Abitbol V, Habauzit C, Benkhalifa S, Claudepierre P
A Qualitative Study Exploring Psychosocial Care in Inflammatory Bowel Disease: Lessons from Aotearoa New Zealand. International journal of behavioral medicine | 2026-05-27
Existing evidence demonstrates that inflammatory bowel disease (IBD) profoundly impacts physical, psychosocial, and emotional well-being, yet psychosocial support is limited in routine care in Aotearoa New Zealand (NZ). This qualitative study aimed to explore the lived experience of adults with IBD in NZ, focusing on psychosocial challenges and patient-driven recommendations for improving support during diagnosis and disease management. Twelve adults with IBD participated in semi-structured interviews as part of a nested qualitative study. Data were analysed using the framework method of thematic analysis to identify key patterns in participants’ experiences. Four main themes reflected the experience of being diagnosed with IBD: (1) trust and mistrust, (2) care not cure, (3) educate, adhere, empower, and (4) dynamics of coping and adjustment. Participants described difficulties navigating the healthcare system, coping with changes in body and identity, and managing the psychological burden of living with a chronic illness. A consistent lack of integrated psychosocial support was reported. Participants emphasised the need for improved health literacy, support for medication adherence, and tailored psychological care. Their suggestions underscored the importance of embedding psychosocial services within routine IBD management. Adults with IBD in NZ face substantial psychosocial challenges that are not adequately addressed in current care models. Integrating psychosocial support into routine IBD care could alleviate patient burden and enhance health system responsiveness. These findings offer critical insights for developing more holistic, patient-centred approaches to IBD care in NZ and similar healthcare contexts.
MHealthPsyc SP, Jones ASK, MHealthPsyc SE, Babbott K, Serlachius A
Modulate Obesity and relateD metabolic complIcations For Yielding improvements in IBD outcomes (MODIFY-IBD): consensus on obesity and cardiometabolic comorbidities in inflammatory bowel disease using systematic reviews and the RAND/UCLA appropriateness method. BMJ open | 2026-05-26
Obesity and related cardiometabolic comorbidities, including hypertension, dyslipidaemia, diabetes, metabolic dysfunction-associated steatotic liver disease and atherosclerotic cardiovascular disease, are increasingly prevalent among individuals with inflammatory bowel disease (IBD). These conditions influence disease activity, therapeutic response, surgical outcomes and overall quality of life, yet evidence remains fragmented. The Modulate Obesity and relateD metabolic complIcations For Yielding improvements in IBD outcomes (MODIFY-IBD) initiative aims to synthesise evidence and generate consensus recommendations to guide practice and future research in this area. This study describes a protocol for a structured evidence synthesis and Research ANd Development/University of California, Los Angeles (RAND/UCLA) Appropriateness Method (RUAM) consensus process. We will conduct three systematic reviews and a structured evidence synthesis organised into three domains: (1) the impact of obesity on IBD outcomes, (2) the burden of cardiometabolic complications in IBD and (3) the management of overweight, obesity and cardiometabolic comorbidities in IBD. A multidisciplinary international panel of gastroenterologists, surgeons, endocrinologists, hepatologists, cardiologists and dietitians will assess each statement using the RAND/UCLA appropriateness method. Panellists will rate the appropriateness of each statement (only those that fall within their area of expertise) on a 1-9 scale (1-3=inappropriate, 4-6=uncertain and 7-9=appropriate), with medians rounded up (eg, 6.5=appropriate). Agreement will be assessed using the RAND Disagreement Index (DI<1.0=agreement). This study will not involve direct patient participation, as it is based on evidence synthesis and expert consensus; therefore, formal research ethics committee approval will not be required. Patient representatives will contribute to the consensus process to provide contextual perspectives but no identifiable data will be collected.Findings will be disseminated through publication in peer-reviewed journals, presentation at major gastroenterology and IBD conferences and communication with professional societies. A lay summary and patient-friendly infographic will also be developed to facilitate translation of recommendations into clinical practice. CRD420251178843: a systematic review of the impact of obesity on inflammatory bowel disease outcomes.CRD420251178799: a systematic review of cardiometabolic complications in inflammatory bowel disease.CRD420251174653: management of overweight, obesity and cardiometabolic comorbidities in inflammatory bowel disease: a systematic review.
Devi J, Samaan S, Sehgal P, Mohamed M, Vincent M, Coombs S, Doering M, Barnes EL, Johnson AM, Yarur AJ
Consensus on Irritable Bowel Syndrome-like Symptoms in Inflammatory Bowel Disease: A Step Toward Advancing Patient-Centered Care.Editorial★ Gastroenterology | 2026-05-25
Abstract not available.
Burisch J, Marsiglio M, Keszthelyi D
Deciphering the Implications of Escherichia coli in Inflammatory Bowel Disease: From Symbiont to Pathogen.Review Pathogens (Basel, Switzerland) | 2026-05-19
Inflammatory bowel disease (IBD) is a chronic inflammatory condition resulting from complex interactions between the immune system, genetic predisposition, and the gut microbiota. In this context, Escherichia coli (E. coli) plays a dual role in the human gut, ranging from harmless commensal strains to pathobionts capable of promoting intestinal inflammation. A growing body of evidence suggests that specific E. coli pathotypes, such as adherent-invasive E. coli (AIEC) and diffusely adherent E. coli (DAEC), contribute to the development and progression of IBD. This narrative review critically examines the microbiological, immunological, and clinical evidence supporting the role of E. coli in IBD, with particular emphasis on mechanisms of mucosal colonization, host-microbe interactions, and persistence within the inflamed intestinal environment. Furthermore, the lack of a standardized operational definition and the limited reproducibility of the AIEC phenotype are addressed, as well as uncertainty about the role played by E. coli as a primary initiator of the disease or as an opportunistic amplifier of intestinal inflammation, and the varying strength of evidence supporting associations with Crohn’s disease versus ulcerative colitis. Diagnostic implications, antimicrobial resistance, and therapeutic aspects are addressed as downstream and context-dependent consequences of E. coli-host interactions, with relevance for disease management and therapeutic response in patients with established IBD. By integrating data from experimental models, clinical studies, and translational research, the review identifies areas of consensus, ongoing controversy, and major knowledge gaps in IBD pathophysiology and clinical practice.
Aceto GM, Falasca K, Berardinucci D, Cavallo L, Mangiò A, Mancuso G, Muraro R, Ciccocioppo R, Catalano T
Intestinal Ultrasound (IUS) (3 papers)
Nitroreductase-Activated Fluorescent Probes: From Molecular Design to Disease Diagnosis.Review ChemMedChem | 2026-06
Nitroreductases (NTRs), a class of flavin-dependent oxidoreductases, are highly upregulated in hypoxic microenvironments and are closely associated with cancer, bacterial infections, and other hypoxia-driven diseases. Precise and real-time visualization of NTR activity is therefore critical for understanding disease mechanisms and enabling accurate diagnosis and targeted therapy. Fluorescent probes have emerged as powerful and versatile chemical biology tools for NTR sensing owing to their high sensitivity, selectivity, and spatiotemporal resolution. Recent advances in two-photon fluorescence imaging, second near-infrared (NIR-II) fluorescence imaging, and time-resolved fluorescence imaging have markedly enhanced tissue penetration and quantitative accuracy, thereby enabling reliable detection of NTR activity in complex biological environments. This review summarizes representative advances over the past 5 years in the molecular design of NTR-responsive probes, with emphasis on recognition motifs, signal transduction strategies, and structure-function relationships that determine selectivity and sensitivity. Disease-oriented applications in cancer, bacterial infections, and other hypoxia-associated disorders-including myocardial ischemia, inflammatory bowel disease, pulmonary fibrosis, and infertility-are discussed. Finally, current challenges and future opportunities are outlined to guide the development of next-generation NTR-responsive probes for high-fidelity imaging and precision theranostic applications.
Ji W, Xiao X, Xu Y, Zhang Q, Hu HY
Imaging endpoints in inflammatory bowel disease: current evidence and future directions for ultrasound and MRI.Review★ BMC medicine | 2026-05-29
Imaging has become a central and rapidly evolving domain in inflammatory bowel disease (IBD) because it captures disease manifestations that extend beyond the mucosa and, therefore, beyond what can be visualized by endoscopy, including transmural inflammation, extraintestinal complications and small-bowel involvement that are not adequately assessed by conventional approaches. In this narrative review, we synthesize the latest evidence on non-invasive cross-sectional imaging-intestinal ultrasound (IUS) and magnetic resonance imaging/enterography (MRI/MRE)-and outline a pragmatic framework for integrating these modalities into clinical trials. The timing of this review reflects the recent publication of two major consensus statements that specifically address how IUS and MRI can be standardized and operationalized as trial endpoints. We first summarize recommended technical standards for acquisition and reporting. We then outline trial-ready definitions of response and remission for clinical trials using validated scores and discuss the emerging but still variably defined construct of transmural healing, understood as the resolution of inflammation across the full thickness of the bowel wall and increasingly associated with improved long-term outcomes. Building on these components, we propose a practical pathway to incorporate imaging from screening, through on-treatment monitoring at predefined windows to adjudicate response/remission, and, where appropriate, to evaluate transmural healing. We emphasize central reading, harmonized timing, and standardized data repositories to minimize bias. Even though meaningful steps have been taken to integrate cross-sectional imaging, it remains essential to evaluate its use pragmatically in both trials and routine care. Furthermore, cost-effectiveness analyses are needed to determine whether widespread implementation is economically justified, and studies should examine whether incorporating IUS/MRI improves patient adherence to clinical trial protocols and follow-up compared with traditional assessment pathways.
Faggiani I, Danese S, Biroulet LP, Jairath V, Rubin DT, Allocca M
Transperineal contrast-enhanced ultrasound: a rapid and reliable tool for differentiating abscesses from inflammatory masses in perianal Crohn’s disease.★ Inflammatory bowel diseases | 2026-05-26
Perianal abscesses are serious complications of Crohn’s disease (CD) requiring timely and accurate diagnosis. Contrast-enhanced ultrasound (CEUS), which in abdominal intestinal ultrasound (IUS) has shown diagnostic performance comparable to CT/MRI in distinguishing intra-abdominal abscesses from inflammatory masses, has not been systematically evaluated in the transperineal assessment of perianal Crohn’s disease. This study aimed to evaluate the diagnostic performance, inter- and intra-observer agreement, and diagnostic confidence of transperineal CEUS versus conventional B-mode TPUS in CD patients with perianal symptoms and suspected septic complications. We retrospectively reviewed 52 examinations of 37 adult CD patients presenting with painful perianal symptoms and suspected septic complications. Patients were included if TPUS detected lesions > 10 mm requiring CEUS characterization. Exclusion criteria were CEUS contraindications, simple fistulas, or large (>3 cm) obvious abscesses. All examinations were recorded, and three blinded experts independently assessed anonymized videos in random order. Lesions were classified as abscesses, inflammatory masses, or phlegmons. Agreement for lesion size, fluid content, and final diagnosis was evaluated using intraclass correlation coefficients (ICC) and Fleiss-Cohen’s kappa (κ). Diagnostic confidence was assessed using a 5-point Likert scale. On B-mode, 17 abscesses, 32 inflammatory masses, and 3 phlegmons were identified. CEUS reclassified several, yielding 16 abscesses, 31 inflammatory masses, and 5 phlegmons. Of the 17 abscesses diagnosed on B-mode, only 4 were also classified as abscesses on CEUS, while 13 were reclassified; conversely, 11 inflammatory masses were reclassified as abscesses. Intra-observer reliability improved from κ = 0.55 with B-mode to κ = 0.95 with CEUS. Inter-observer agreement for diagnosis was poor with B-mode (κ = 0.31) but excellent with CEUS (κ = 0.83). Transperineal CEUS significantly improves inter- and intra-observer agreement and diagnostic confidence compared with conventional B-mode TPUS when differentiating perianal abscesses from inflammatory masses/phlegmons in CD and frequently leads to lesion reclassification in clinically ambiguous cases. Transperineal contrast-enhanced ultrasound (CEUS) improves diagnostic accuracy and reliability over conventional B-mode ultrasound in detecting perianal abscesses in Crohn’s disease, offering better intra- and inter-observer agreement and effective real-time assessment in urgent clinical settings.
Maconi G, Bezzio C, Saleh A, Silva Mendes S, Lepore F, Abraham BP, Carter D
Nutrition & Lifestyle (3 papers)
β-Glucan and Inulin Estimated Intake Are Associated With Reduced Risk of Crohn’s Disease, Improved Gut Barrier and Systemic Inflammation Markers, and Multi-Omic Signatures in a High-Risk Cohort.★ Gastroenterology | 2026-05-28
The cause of Crohn’s Disease (CD) remains unclear; however evidence suggests fiber intake may play a role. We aimed to investigate the association between intake of total fiber and select fermentable fiber subtypes and future risk of CD in an at-risk population. The Genetic, Environmental, Microbial Project prospectively followed asymptomatic first-degree relatives of individuals with CD. Habitual intake of total fiber and select fiber subtypes was estimated from baseline food frequency questionnaires and biologic samples were collected. Incident CD was confirmed during follow-up. Cox proportional hazards models estimated hazard ratios (HRs) for CD. Associations between fiber subtype intake and urinary fractional excretion of lactulose-mannitol ratio (LMR), C-reactive protein (CRP), gut microbiota (16S rRNA sequencing), and serum proteomics (Olink®) were evaluated using multivariable regression models. During a median follow-up of 8.5 years of 3,314 FDRs, 94 developed CD. Higher β-glucan (HR 0.70, 95% CI 0.54-0.92) and inulin (HR 0.68, 95% CI 0.49-0.96) intake were associated with lower CD risk. Associations were strongest in those with higher baseline relative abundance of Erysipelotrichaceae UCG-003, but weaker with higher Colidextribacter. Higher β-glucan and inulin intake were associated with lower LMR, lower abundance of pathobionts (Ruminococcus torques and Lachnoclostridium), and lower concentrations of inflammation- and barrier-related proteins, including CRP, TREM-1, OSM, and MMP-9. Higher estimated β-glucan and inulin intake was associated with preserved gut barrier function, lower systemic inflammatory markers and lower CD risk which was modified by the microbial context. These findings support microbiome-informed dietary strategies and intervention trials for CD prevention.
Xue M, McShane C, Kim J, Khorasaniha R, Leibovitzh H, Shao J, Chen R, Jeong S, Madsen KL, Griffiths AM
Comparing characteristics and outcomes between hospitalized adults on a pea protein or dairy/soy protein formulas: initial findings. Journal of comparative effectiveness research | 2026-05-26
Enteral formulas are an essential part of nutrition support to prevent or treat malnutrition and minimize hospital length of stay (LOS). Yet not all formulas are tolerated and may leave nutritional needs unmet. Unique pea protein plant-based formulas (PPPBF) are nutritionally complete and have accumulated evidence of good tolerance, but impact on health economic outcomes (HEO) is largely unknown. Aim: To examine differences in patient and clinical characteristics and HEOs of hospitalized adults using PPPBF versus dairy and/or soy protein (DSP) formulas to inform further research. Materials & methods: Retrospective comparative cohort study examined real-world data (Premier Healthcare Database) from adults (≥18 year) admitted to US hospitals who were prescribed a formula between 1 January 2020 and 30 September 2023. Patient and clinical characteristics and HEOs were compared between the PPPBF and DSP groups by unadjusted descriptive analysis. Results: Preliminary analyses were conducted on inpatients (n = 65,338 DSP; n = 243 PPPBF) from 60 US hospitals. PPPBF (versus DSP) group was younger (mean [SD] 63.6 [17.0] vs 66.7 [17.3] years; p = 0.006) and had a higher diagnosis rate for malnutrition, weight loss, food allergies, irritable bowel syndrome and/or inflammatory bowel disease on admission. Overall, formula intake was primarily oral but higher in PPPBF versus DSP (100 vs 78.3%, p < 0.001). Charlson Comorbidity Index indicated PPPBF (versus DSP) was sicker (median 4.0 vs 3.0; p < 0.001). Yet PPPBF group had shorter LOS (by ∼2 days; p < 0.001) and lower mortality rate by discharge (5.8% vs 11.5%; p = 0.005) without significant difference in 90-day readmission/outpatient visit rates after discharge (unadjusted comparisons). Conclusion: Preliminary evidence in hospitalized adults observed a shorter LOS in PPPBF users, despite higher baseline acuity and without significant difference in readmission/outpatient visit rates compared (unadjusted) to DSP users. Adjusted analyses and further research are needed. What was the aim of this research? To identify and compare preliminary clinical and healthcare resource use differences between hospitalized adults who consumed pea protein plant-based formulas (PPPBF) or dairy and/or soy protein (DSP) formulas for further study. How was the research carried out? Real-world deidentified data previously collected by Premier Healthcare Database included adults in US hospitals who were prescribed a formula over 3-year study period (2020–2023). Study groups were assigned based on formula used: PPPBF or DSP. Patient and clinical characteristics and health economic outcomes, like hospital length of stay, were compared between groups. What were the results? Preliminary analyses were performed on large dataset from 60 US hospitals (DSP = 65,338; PPPBF = 243). The PPPBF group was younger and sicker than DSP group based on measures related to risk of death, nutritional status and gastrointestinal function. Initial results showed the PPPBF group had a shorter length of stay, lower rate of death in the hospital and similar percentage of hospital readmissions or outpatient visits after discharge compared with the DSP group. Further testing to confirm these preliminary findings is underway. What do the results of the study mean? The use of PPPBF, as an alternative to DSP formulas, to supplement nutritional intake in the hospital may have benefits for the patient and healthcare system despite greater illness severity and nutritional risk as observed in this study. In this preliminary study, those in the PPPBF group left the hospital sooner and had comparable rates of readmissions or outpatient visits compared with DSP group. More testing of these findings is underway.
Millovich V, Shingara IO, Lopes GS, Tyagi M, Cao Z, Valentine CJ
Anti-inflammatory dietary interventions in inflammatory bowel disease: current insights and future perspectives. Frontiers in nutrition | 2026-05-11
Inflammatory bowel disease (IBD), encompassing Crohn’s disease (CD) and ulcerative colitis (UC), arises from multifactorial interactions involving genetics, gut microbiota dysbiosis, immune dysregulation, and environmental triggers, with diet playing a pivotal role. Anti-inflammatory dietary patterns have emerged as adjunctive therapies to pharmacological treatments, potentially inducing and maintaining remission by modulating microbiota and inflammation. This perspective reviews the mechanistic basis for dietary interventions, evaluates key strategies such as the Mediterranean diet (MD), Specific Carbohydrate Diet (SCD), low-FODMAP diet, IBD-Anti-Inflammatory Diet (IBD-AID), and Groningen Anti-Inflammatory Diet (GrAID), and discusses clinical evidence, challenges, and implications. While promising, evidence is constrained by heterogeneous studies and small cohorts. Future research should prioritize large-scale randomized controlled trials (RCTs) with multi-omics integration for personalized nutrition in IBD management.
Li M, Jiang C, Wang B, Guan Z, Li L
Drug Safety & Pharmacovigilance (1 papers)
Pathological reprogramming of innate immune cells drives resistance to biologics in inflammatory bowel diseases.Review Autoimmunity reviews | 2026-05-25
Inflammatory bowel disease (IBD), encompassing Crohn’s disease (CD) and ulcerative colitis (UC), is a chronic immune-mediated disorder characterized by persist ent intestinal inflammation. With a rising global incidence, IBD poses a significant therapeutic challenge. Although biologic agents targeting TNF, α4β7 integrin, or IL-12/ 23 p40 have improved clinical outcomes, over 40% of patients experience primary non-response or secondary loss of response within the first year, often accompanied by adverse events. This review systematically investigates the dynamic reprogramming of intestinal innate immune cells (particularly macrophages, dendritic cells, and neutr ophils,as well as emerging populations such as eosinophils and ILCs) during biologic therapy and their association with treatment resistance. Under physiological conditions, intestinal innate immune cells maintain barrier integrity, regulate immune tolerance, and facilitate tissue repair. In IBD, however, these cells undergo pathological activation characterized by pro-inflammatory polarization, dysregulated cytokine production, and disrupted interactions with the gut microbiota, thereby sustaining chronic intestinal inflammation. The efficacy of biologic agents in IBD largely relies on their capacity to restrain excessive innate immune activation and rebalance mucosal immune responses. Nevertheless, adaptive reprogramming of these innate immune cells can drive therapeutic resistance through a convergence of mechanisms: sustained activation of inflammatory signaling, metabolic reprogramming that reinforces pro-inflammatory states, induction of pathogenic T cell responses, and self-perpetuating loops that sustain tissue injury. Overall, our findings highlight reprogramming of intestinal innate immune cells as a central mechanism mediating both response and resistance to biologics, offering a mechanistic rationale for future strategies targeting immune cell-microenvironment interactions to overcome therapeutic resistance in IBD.
Diao J, Cao H, Zhou J, Shen J
Pregnancy & Reproductive Health (1 papers)
Gallstones: Physiopathology and treatment of cholelithiasis (part 1).Review Journal of visceral surgery | 2026-05-27
Cholelithiasis (gallstones) is a frequent disease, with an estimated annual risk of 1 to 4% of presenting clinical manifestations. It mainly results from imbalanced bile composition: cholesterol oversaturation, low levels of bile acids and gallbladder stasis resulting in the formation of gallstones. Two main types of gallstones exist: cholesterol gallstones (the most frequent), and pigment gallstones. The risk factors for lithiasis are multiple: age, female sex, rapid weight fluctuations, certain medical treatments, pregnancy, and a number of pathologies (diabetes, obesity, cirrhosis, Crohn’s disease…). While lithiasis is often asymptomatic, approximately 20% of patients present with biliary colic or can develop severe complications: acute cholecystitis, stone migration, cholangitis or acute pancreatitis. In the event of symptomatic complications, laparoscopic cholecystectomy is the standard treatment. In the absence of clinical evidence, however, a conservative attitude is generally recommended, except in situations involving a risk of malignant transformation (large gallstones, adenomatous polyps, incomplete porcelain gallbladder…). Even though surgical technique is codified in terms of Critical View of Safety (CVS), the role of intraoperative cholangiography remains debated. Acute cholecystitis is managed according to the degree of severity and taking into account the Tokyo recommendations; available options range from early surgery to percutaneous drainage in the setting of major surgical risk. Management in pregnant women, elderly patients and cirrhotic patients, is individualized insofar as these populations present a risk of complications needing a personalized therapeutical approach.
Golse N, Boulard P, Ciacio O, Robin F, Mohkam K, Rode A, Faitot F, Couillerot J, Chopinet S, Maulat C
Category Distribution
The Interactive Dashboard lets you filter and search across all categories, download results as CSV or Excel, and explore the full 30-day backlog - useful if you missed a week or want to search by keyword across a wider date range.
Subscribe via RSS to get daily updates automatically, or use the per-category feeds to follow just one subfield.